Transcript
Hi, it’s Dr. Centeno. And today we’re going to go over MRI evidence that the Regenexx Perc-ACLR procedure heals ACL tears. So, we invented ACL stem cell injections at the Centeno-Schultz Clinic, which is the headquarters of the Regenexx Network. Regenexx is worldwide at this point.
And the procedure is technically demanding, and places bone marrow stem cells, otherwise known as bone marrow concentrate, into the torn ACL using Fluoroscopy or X-ray guidance.
And the procedure shows good MRI evidence of ACL healing and rapid return to play in about two-thirds of the patients who normally get surgery. So we have to pick the right patients in order to get high success rates with this, but it’s about two-thirds of those people who currently get their knee operated. And the procedure is obviously much less invasive than an ACL reconstruction — which is tearing out the ACL, drilling tunnels, putting in anchors, basically carpentry in the knee — and it’s got much less downtime. So, it gets athletes back to what they do much more quickly.
We’ve published several papers on the technique, and we’ve completed a Randomized Control Trial, which is just winding its way through the system to get published. And over the years, we’ve collected occasional MRIs from select patients that I’ll review here. Now, this is not even close to all the MRIs that we’ve done, before and after. These are just the ones that we stopped enough to put online and I’ve kind of collected those here.
I’ll Show You 23 Before-and-After MRIs
Again, no other clinic or clinic system on Earth — I don’t care if it’s a famous sports medicine clinic that treats this guy or that guy — can show you data like this on a procedure that gets rid of the need for ACL surgery. Now, some of that is because those places do ACL surgery, and this procedure obviously would be a threat to systems like that.
In the meantime, you’re going to learn a thing or two about reading MRIs of torn and normal ACL ligaments.
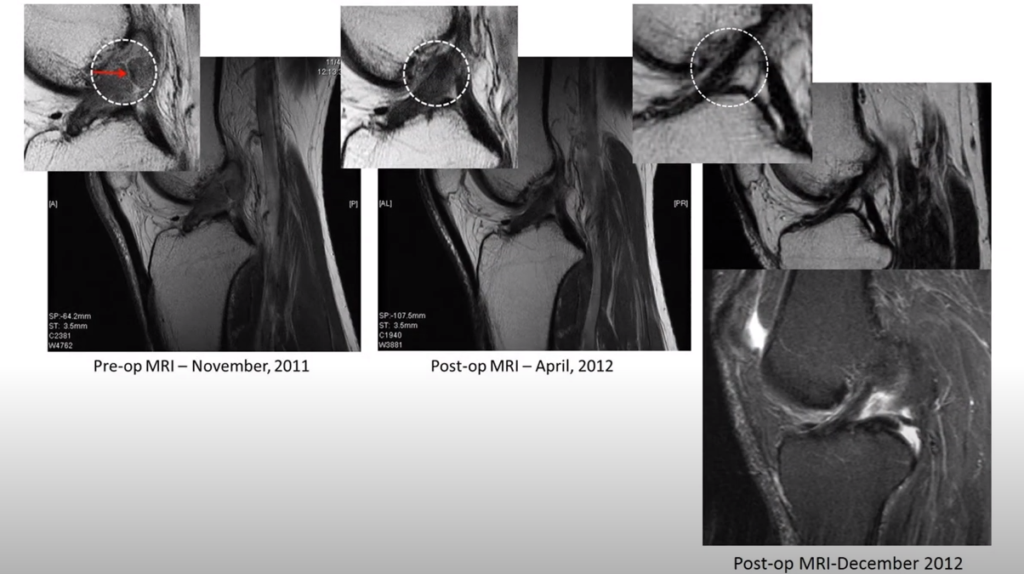
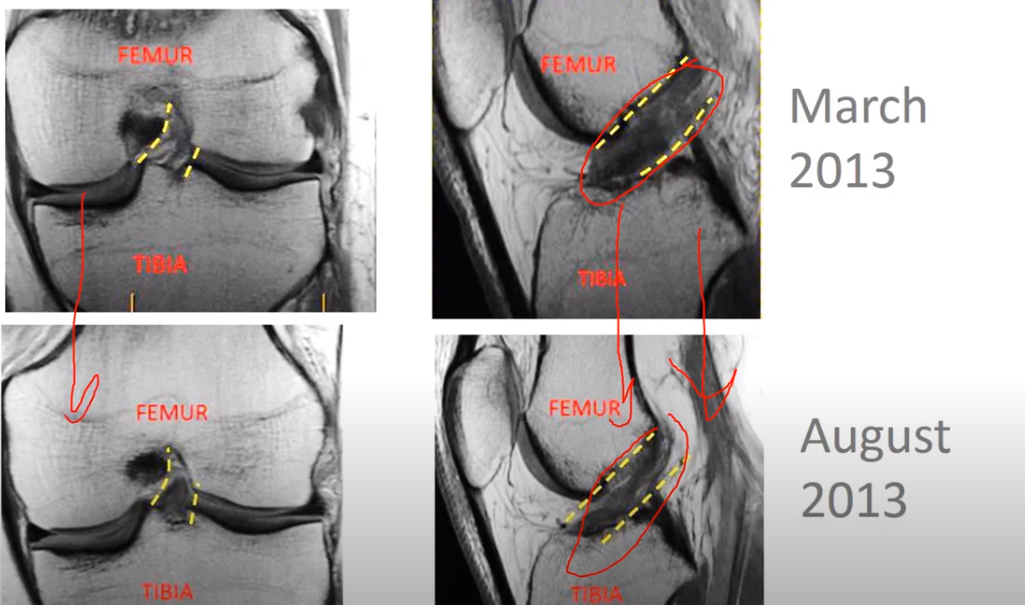
So, here’s a really early one, 2011, we did, here. You can see that up here, this shows an actual frank tear [see figure 2]. You can see a separation in the ACL. Now, the ACL is going along this way here, and then here you can see it as that tear heals, and then you can see the whole morphology of the ACL ligament gets smaller, which is great. That means that it’s more normal.
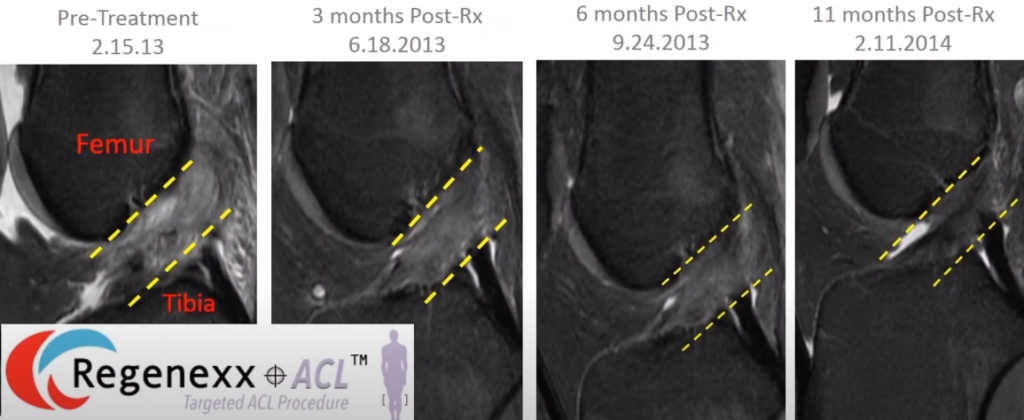
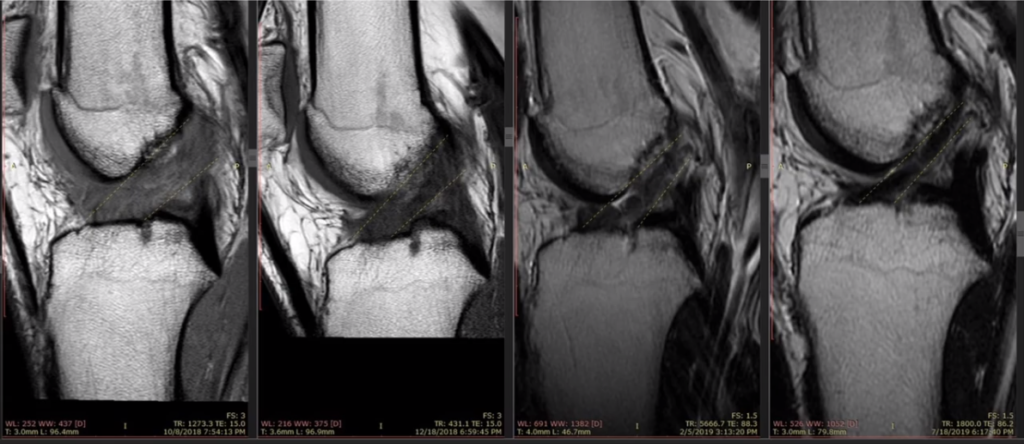
And this is just –these are Sagital images, so side cuts, and you can see, here [see Figure 3, below], the ACL should go between these yellow dash lines. And then as time goes on after the procedure, by this one, the ACL gets a little bit more together. You can see over here on the first one that the ACL is kind of amorphous. Those fibers are kind of going all over the place. But by the second one, it looks better. By the third one, it looks better. And by the fourth one, it looks normal. Now, this is an older patient. So this is something that occurred more slowly, in this patient, than it would in a younger patient.
Here [see Figure 4, below] you can see a frank tear on the ACL. Again, the ACL is this dark line that’s supposed to go up like this and it’s supposed to be continuous. But you can see on the left there’s a frank tear. On the right, there’s not.
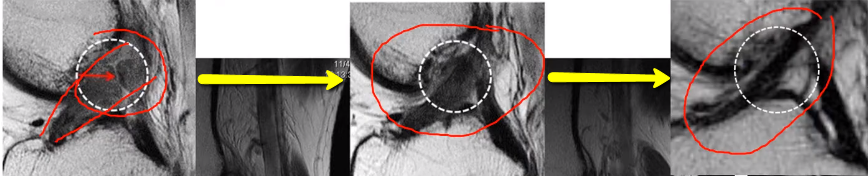
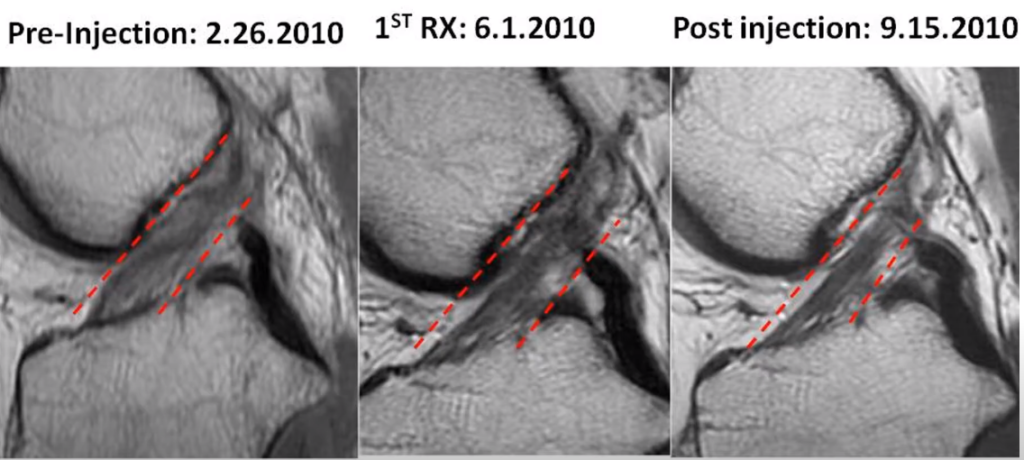
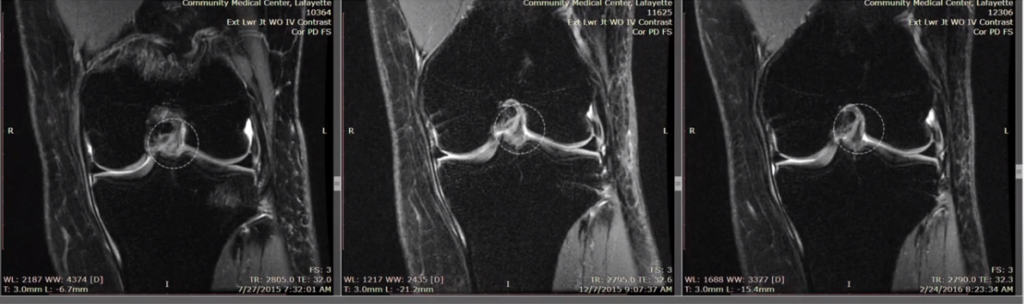
This is one [see Figure 5, below] of our really early patients from 2010. The ACL should be a dark line that’s going diagonally between those red dashes, or red dash lines that you see right there. But you can see it’s kind of blown out and light and amorphous. And you can see over time, here, from this one [middle] to that one [right-most], it gets nice and tight and more dense and smaller, which is evidence of healing.
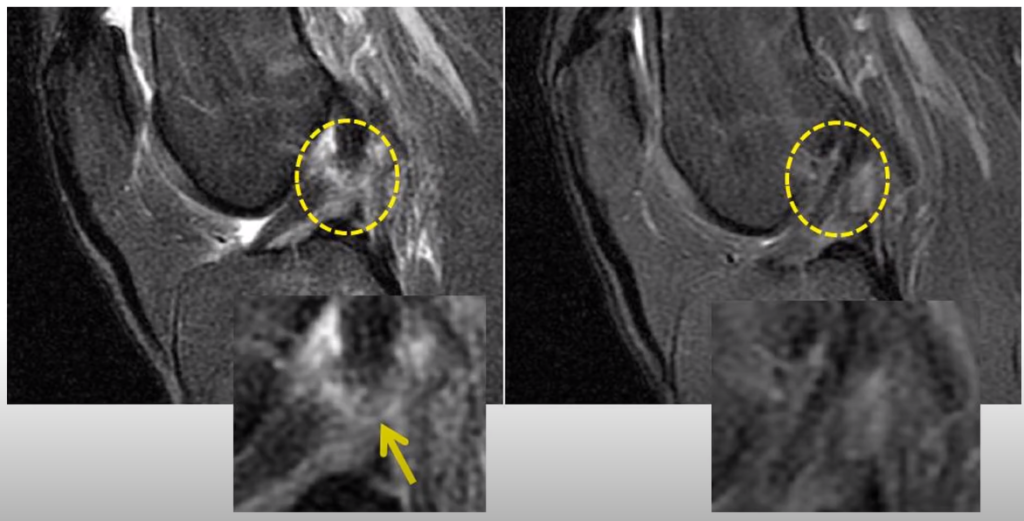
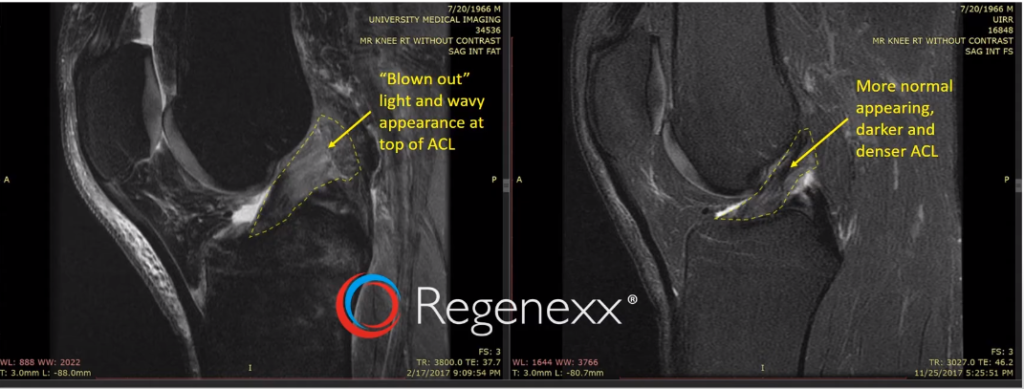
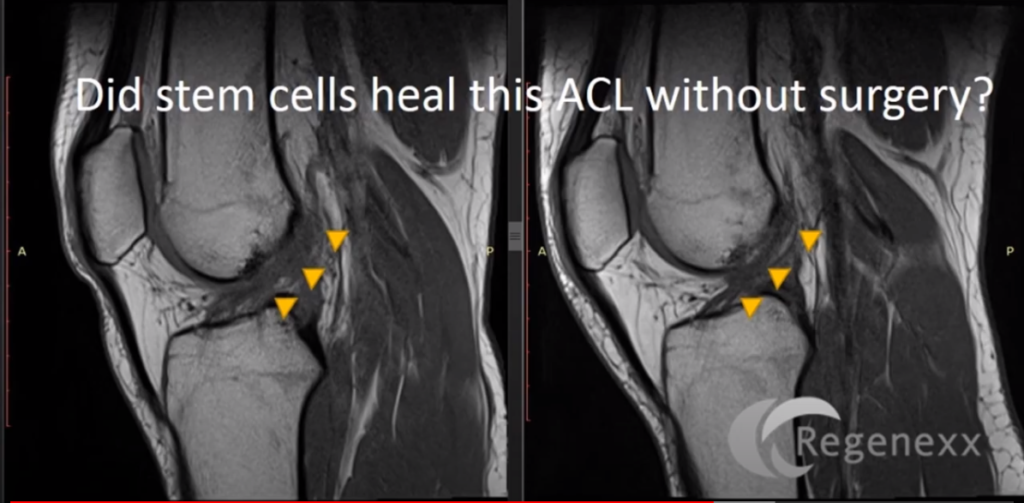
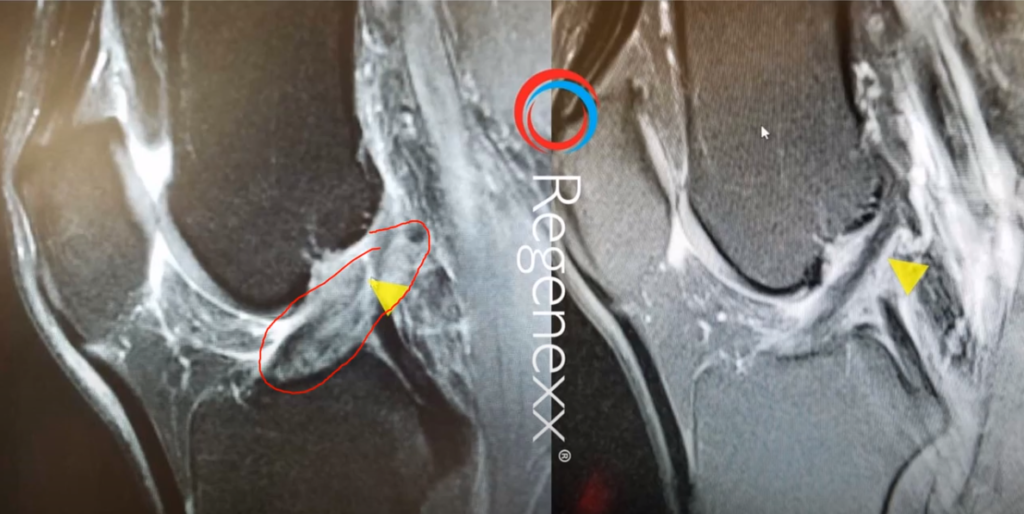
You can see, here [see Figure 6, below], I’ve outlined the ACL in that yellow dash line, and the top part, there, is blown out and wavy. The bottom part on that left image, so down here, the ACL looks pretty normal. Up here [where the yellow arrow points], it looks blown out. The blown-out Is that light color where it actually gets bigger. And then you can see, off on the right, after the procedure, a more normal-appearing, darker, and denser ACL. Again, everything I’ve shown you so far is without surgery, just this percutaneous, meaning through the skin, and precise injection of stem cells into the ACL.
Related: Shoulder MRI
You can see, here [in Figure 7], that there’s actually a tear there, meaning a line going across the ACL. And you can see that that line goes away. And here you have just two different types of images. The one on the left is similar to what you’ve seen so far, which is called a FAT SAT where water is bright. The image on the right is not a FAT SAT. The image on the right is a Proton-Density image — where you’ve got the bone is actually bright now and water is also a little bright. Just two different types of MRI sequences.
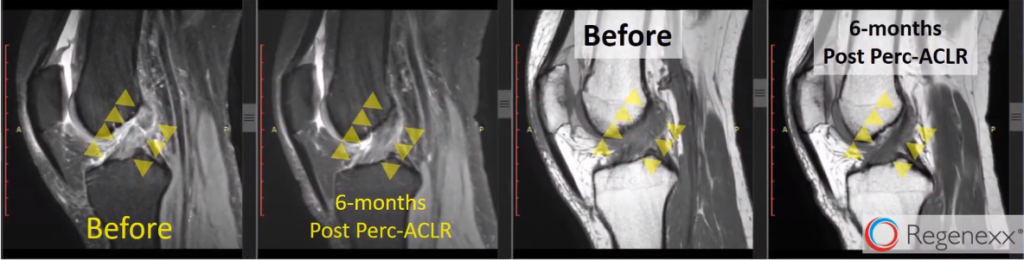
On the left here [in Figure 8, below], we see a totally blown-out ACL. There’s no –you can see it’s bright, it’s big, the fibers are going all over the place. And, then, three months later — this is a young person, so it only takes three months — you see a really beautiful ACL that was read out as normal ACL by the reading radiologist. Again, no surgery — only the Regenexx Perc-ACLR procedure.
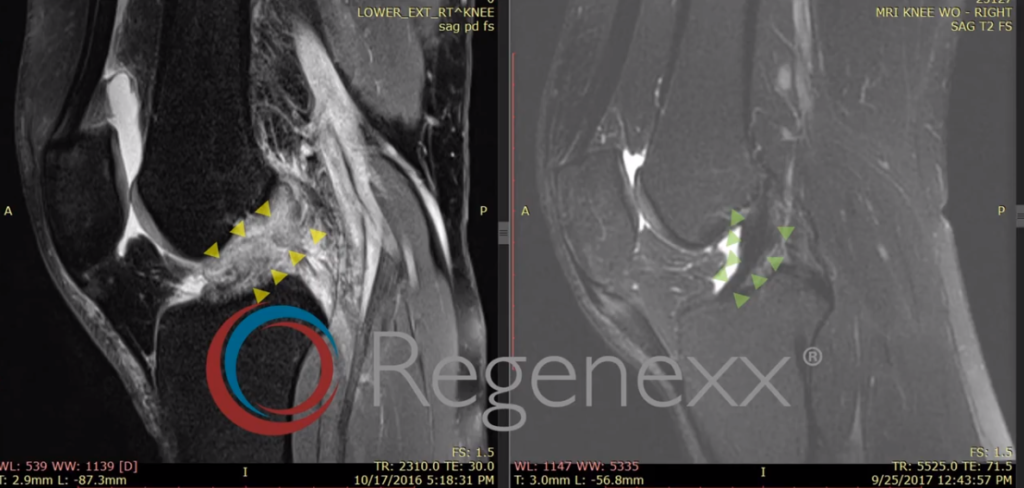
You can see images here [in Figure 9, below], off on the left, again, ACL, which should be a nice dark line going in here, isn’t; it’s this bright amorphous kind of blown out thing. And you can see that after treatment, we’ve now got an ACL, an ACL which looks darker, which looks more robust.
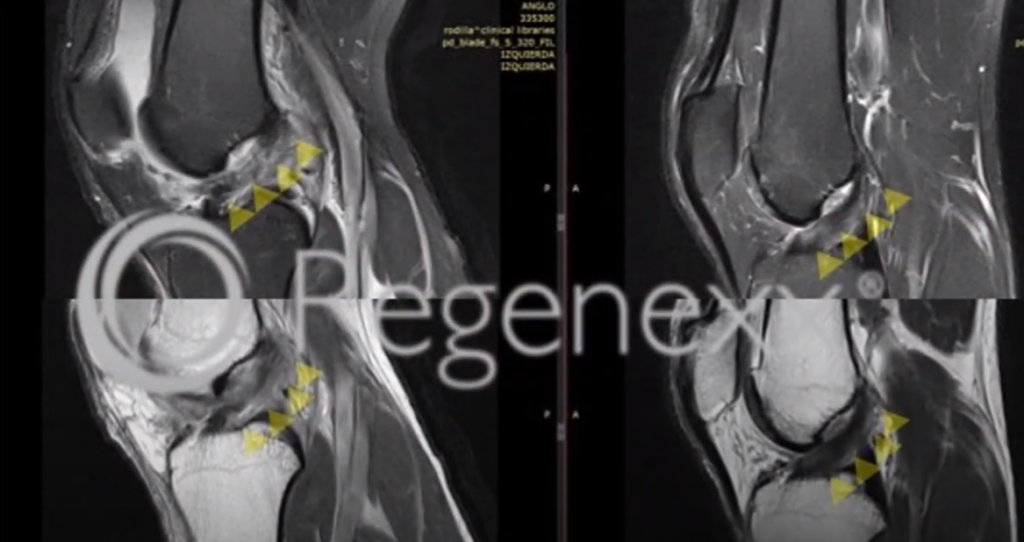
Again, here [in Figure 10, below] we have an ACL, which has an actual tear in it, which is that white line going across it. And, you can see here that the ACL doesn’t have that anymore.
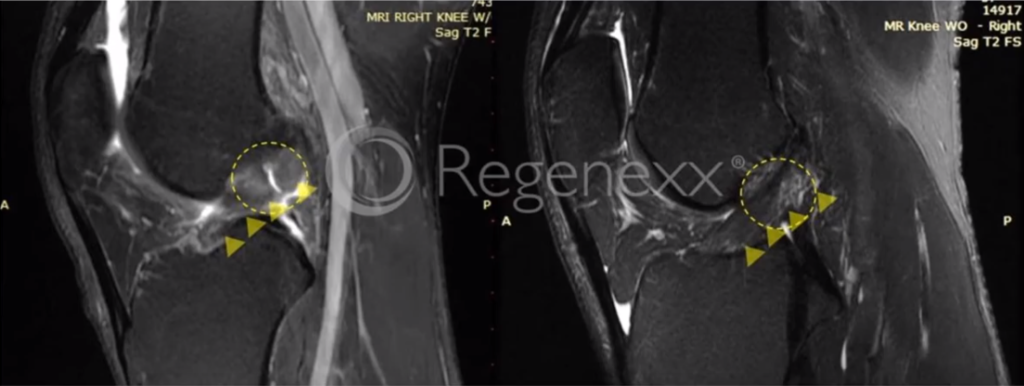
This [in Figure 11, below] is not much of an ACL left. There you can see it’s bright, it’s wavy, and you can see here a much more normal-appearing ACL off on the right. Again, no surgery, just this injection-based procedure.
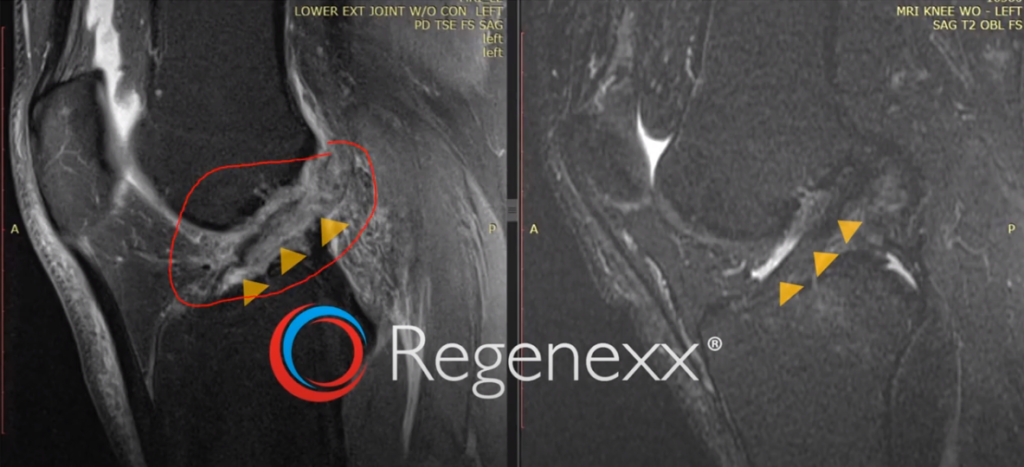
Here [in Figure 12, below], we have an early result – just three months later. The ACL looks kind of wavy, amorphous, bigger than it should. And here looks nice and dense and dark.
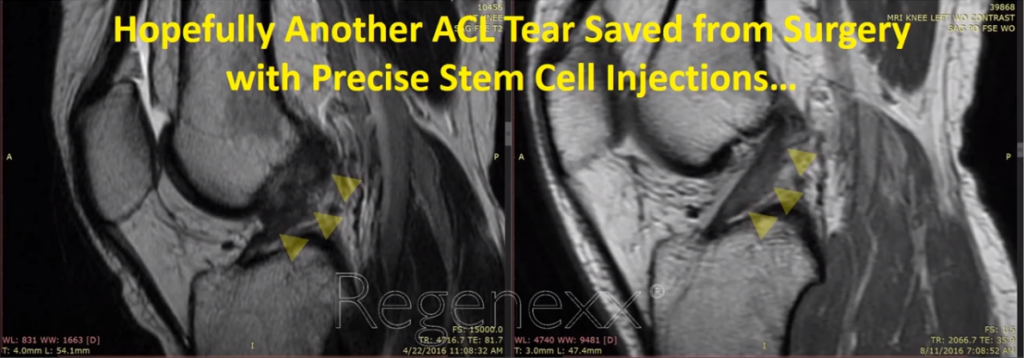
And the same thing, here [see Figure 13, below], we have two different images, the ones on the left are both before, the ones on the right, again are the after the procedure. You can see this, amorphous ACL, turns into this nice, tight, dark ACL on that type of imaging sequence. Same exact knee here from before. But now we have a FAT SAT imaging sequence where water is really, really bright and you can see a nice, dark, dense ACL after the injection procedure.
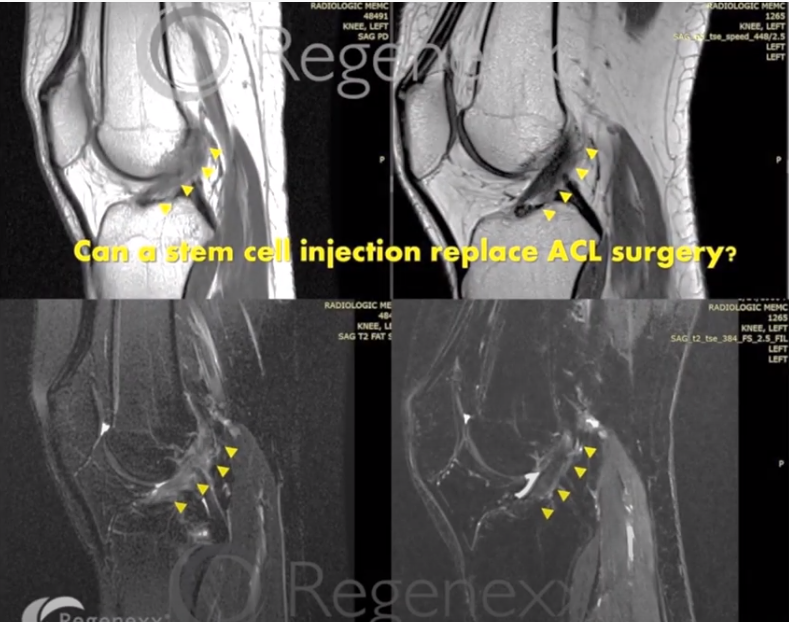
Here [in Figure 14] again, we’ve got an ACL that’s really hard to identify. There’s very little dark tissue in there going diagonally, as an ACL should. But after the procedure, we see that we have some dark tissue going diagonally, as an ACL should.
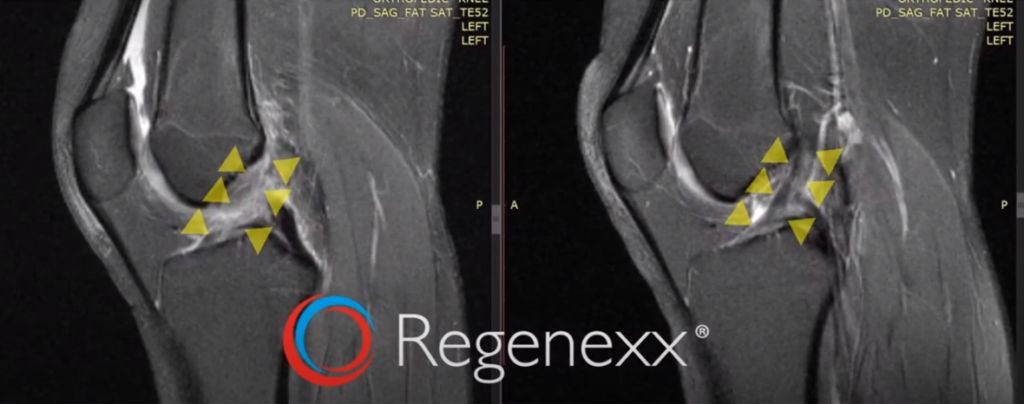
On the left [in Figure 15, below], we’ve got this amorphous thing that is in the vicinity where the ACL should go, diagonally. And it gets some nice form here, although it’s still a little bright, still has a little ways to go in healing. But now it’s nice. It’s denser with actually some fibers all going in the same direction, diagonally.
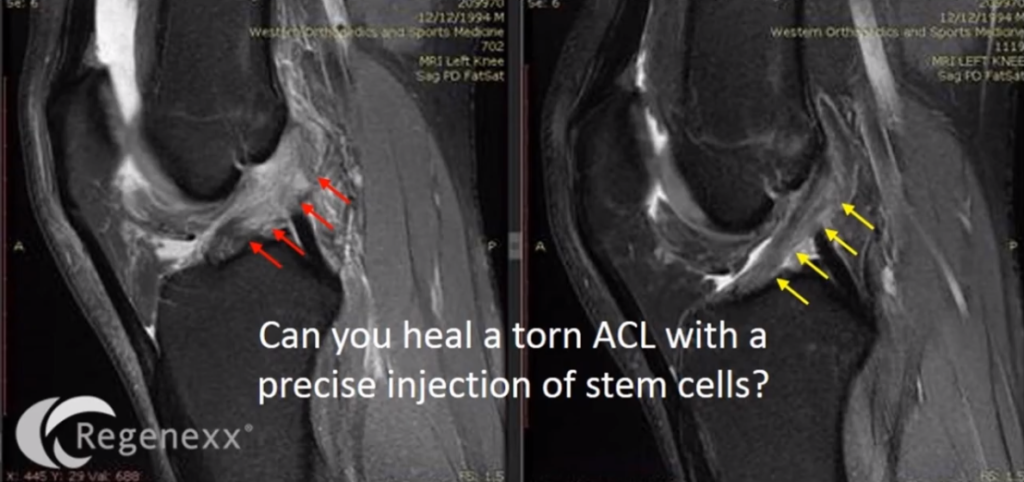
Here [in Figure 16, below], again, kind of amorphous, blown-out ACL goes to nice, tight, dense ACL.
We’re now looking from the front, here [in Figure 17, below], as well as the side. You can see that the Before’s are on top in the After’s go this way. So, again, kind of larger, amorphous blown out ACL goes to much tighter, denser ACL. You can see the same thing happening from the front. But we won’t get too much into that since we’re looking at ACLs from the side today.
So, again, we can see here just a progression over time [in Figure 18, below]. This ACL is kind of blown out, amorphous, big. You can see it gets smaller, tighter, and denser. And this would be read out as a normal ACL here. Off on the right – small, tight, dense, going at a 45-degree angle on the side MRI image.
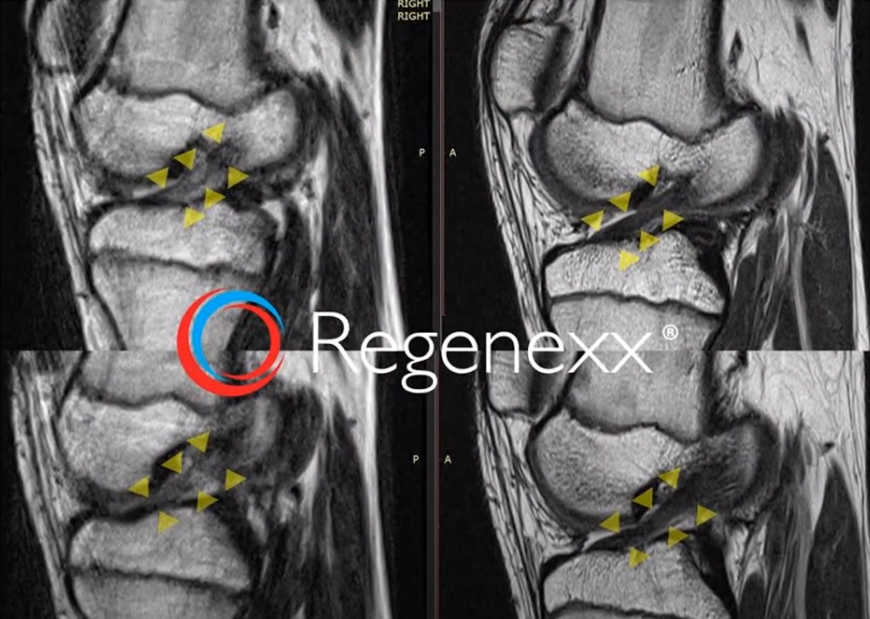
Similar thing here [in Figure 19, below]. These are the Before images on your left. You can see the ACL between the arrows there, which is kind of amorphous, got some white spots in it here and here. These are just images on the After, which are just one after the other. So a slice and a slice. But again, showing a very nice tight, dense, ACL.
This [in Figure 20, below] is a front image; the ACL is actually within that little circle I drew. And you can see here that the ACL starts in this image very, very bright. It’s right in this area here. And then it goes overtime to a much darker ligament inside that circle. We’re looking at the front of the ACL there.
Again [in Figure 21, below], blown out, amorphous goes to smaller, tighter, denser, again. Blown out complete ACL tear; and then an ACL, on the right, that would be read out as normal. The same thing, here, we see again, big blown-out ACL tear going to something nice and tight.
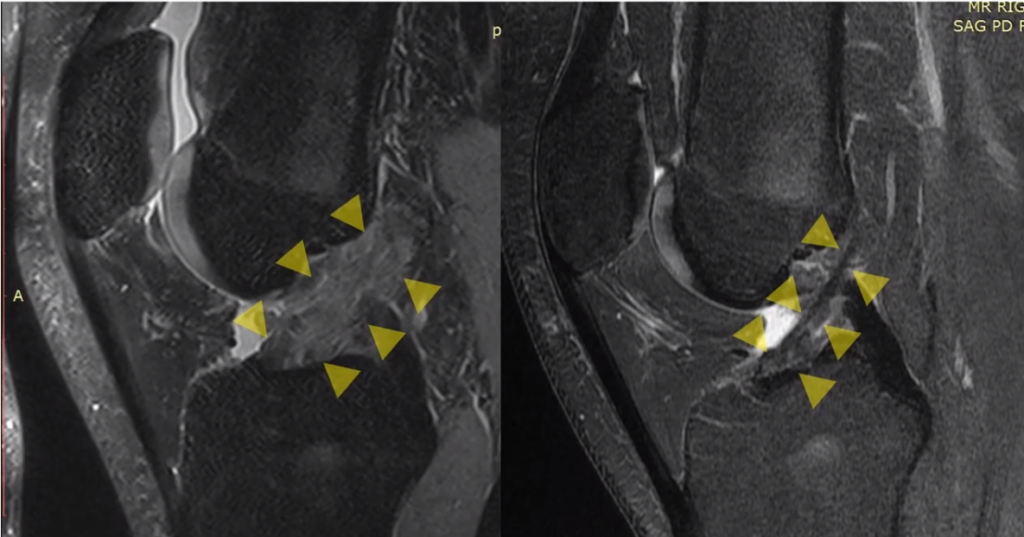
These are two images. [in Figure 22, below] This is the Before here [on the left] and then we go to the After on the [right] side [in Figure 22]. So we see lots of bright stuff in that ACL, then much less bright stuff in that ACL. And then we actually see here a bone marrow lesion, which is where the bone itself got bruised with the initial injury. And then the ACL is in here from the front, and it gets tighter and denser.
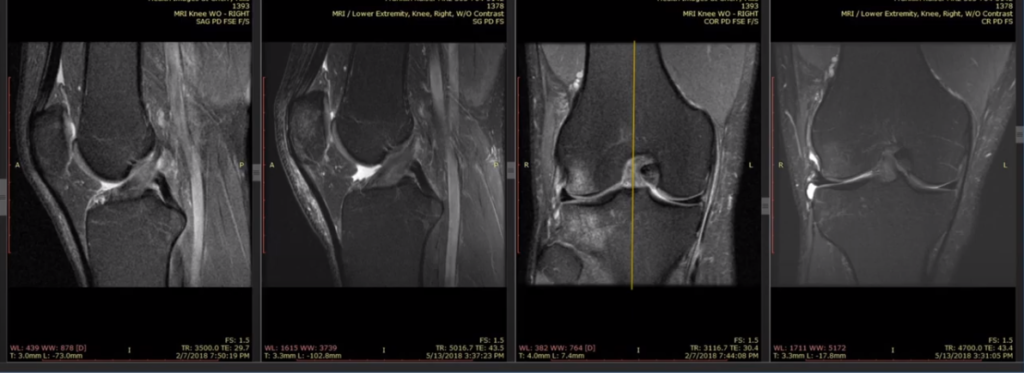
Again, here we see a bright amorphous ACL, going to something recognizable as an ACL, with these tighter fibers that are darker.
So thanks so much for watching. I know that was a little bit of a long slog through lots of images, but I think it’s important to show all these images because we have so much data. Not only that we’ve collected on patients about their pain and their function, and their ability to return to what the love, but also this incredible MRI evidence, which is really the largest data set of Before and After ACL images in existence.
Why? Because we invented this procedure. No one else has got a data set like that of Before and After ACLs, with regard to stem cell injection procedures. So thanks so much for watching. Please subscribe. Please like the video and obviously leave any comments. Thanks so much. Have a great day!
To learn more about the Perc-ACLR, you can read more about it here.