Degenerative disc disease (DDD) is a physiological breakdown of the intervertebral discs in the spine. Clinical studies have shown that disc degeneration, or the narrowing of at least one intervertebral space, is prevalent in nearly 60% of the population above 40 years of age(1).
DDD can occur in the cervical, thoracic, or lumbar spine. While it is a natural process, you can prevent it from progressing using a range of stabilizing exercises. Read on to find out more about the best exercises for DDD.
The Importance Of Degenerative Disc Disease Exercises
As disc degeneration progresses, the intervertebral cartilage erodes and the intervertebral space narrows. The shorter the disc height, the more unstable the spine becomes due to the pull of gravity and the adjoining muscles.
The deeper muscles gradually atrophy because of the decreased spinal activity. This further destabilizes the spine, resulting in a self-perpetuating cycle of disease progression and loss of function.
A spine specialist can prescribe exercises that will help strengthen and stabilize the spine to slow the progression of the disease. These are known as spine stabilizing exercises. They are usually completed under the supervision of a physiotherapist.
Research has shown that these exercises can relieve pain, improve spinal function, and reduce the limitations of daily activities (2). There are many exercises out there but there are some specific ones that are good for degenerative disc disease.
The 10 Best Exercises For Degenerative Disc Disease
We’ve rounded up the 10 best exercises for degenerative disc disease. Some of them are simple and others may require guidance from a trained physiotherapist. You can start these exercises after a 10-minute warm-up. The spine stabilizing exercises are listed below:
1. Walking
Walking is a daily activity that can help prevent the progression of DDD. Free walking, treadmill walking, or walking with equipment can strengthen the paraspinal muscles and prevent them from atrophying.
Studies have shown that walking reduces back pain(3) when completed consistently. There’s no difference between slow walking and brisk walking, but the goal is to keep the spinal, paraspinal, pelvic, and abdominal muscles active without straining the spine.
2. Hamstring Stretch
You can stretch the hamstrings muscles by leaning over and trying to touch your toes. Alternatively you can use a chair and follow these steps:
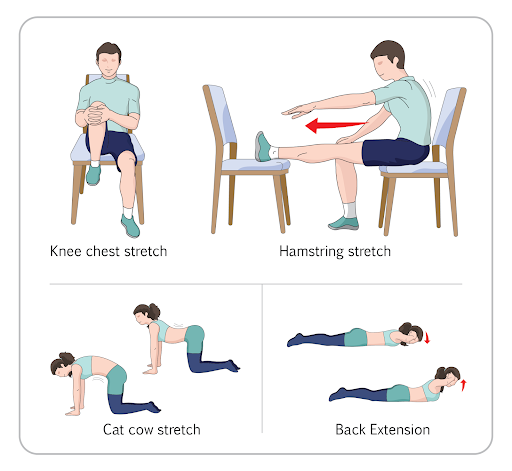
- Start by sitting on a chair.
- Place another chair in front of you for this stretch.
- Keep one leg on the floor, then put your other leg up onto the seat of the chair in front of you.
- Stretch the hamstring gradually.
- Hold the stretch for 30 seconds.
- Gradually increase this to a minute over time.
Practice this stretch twice a day initially and then every alternate day if there is no pain.
There are two forms of hamstring stretching. Active hamstring stretching and passive stretching. Active hamstring stretching is done against resistance and gravity without any assistance. For DDD, passive stretching is recommended because it is more supportive as the range of motion is achieved with assistance.
To complete a passive stretch, a physiotherapist will help you with the stretch or will teach you to use a tool like an exercise ball or band.
Whilst there are many different variations of hamstring stretches, avoid the ones that require you to stand as standing exercises can put more load on the spine.
3. Stationary Exercise Biking
Stationary exercise biking is considered to be gentle on the spine when compared to running or jogging. This exercise can reduce back pain in individuals with DDD as soon as eight weeks, with more compelling results seen by six months. Stationary biking is a low-impact exercise that can help relieve the symptoms of lumbar spinal stenosis.
The benefit of exercising on a stationary bike depends on the extent of your disease and the location of your DDD. To start with, you could do a 10-minute biking session two to three times per week. You can increase this time based on your symptoms and directions from your doctor or physiotherapist.
4. Cat-Cow Stretch
The cat-cow stretch is an exercise where the back oscillates between flexion and extension. Here are the steps for the cat-cow stretch:
For The Cow Pose
- Start on your hands and knees with your wrists under your shoulders.
- Visualize a straight line from your head to the tailbone.
- Inhale and curl your toes.
- Drop your belly, keeping the abdominal muscles close to the spine, and tilt the pelvis backward.
- Draw your navel inwards and try to look upwards gently.
For The Cat Pose
- Next, exhale and release your feet so the tops of your feet are flat against the floor.
- Drop your head and gaze towards your navel – this will round the back and keep your navel tucked in.
- Repeat the sequence, alternating gently from cow pose to cat pose.
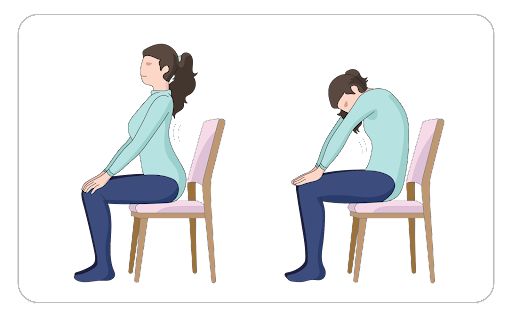
Do this for five to 10 breaths. If you cannot do this on the floor, you can also sit in a chair and do this stretch.
5. Back Extension
Back extension exercises are good for building lower back strength. They also activate the glutes and the hamstrings. One thing to remember, always do back extension exercises at the end of your routine so that your erector spinae muscles are not fatigued.
Here are the steps for the back extension exercises:
- Lie down on your stomach on a mat.
- Keep your legs straight behind you.
- Slide your shoulders downwards with your hands on the floor, behind your head or crossed in front of your chest. You can start with hands on the floor if you’re new to back extension exercises.
- Try to lift your upper back away from the mat while pressing your hips into the ground.
- Hold this stretch for 30 seconds.
You can do this exercise twice a week.
6. Knee-To-Chest Stretch
The knee-to-chest stretch is an exercise that can help improve the flexion of the lumbar spine. This exercise strengthens the glutes and the abdominal muscles. The main stretch involves a person lying down on a bed. Here are the steps:
Single Knee-To-Chest Stretch
- Start by lying down on your back.
- Keep one leg straight out, then bring up the other leg to your chest and wrap your arms around it.
- Hold for about 30 seconds.
- Repeat on the other side.
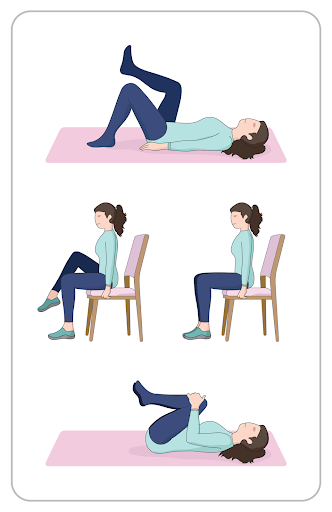
Variations of this stretch include the double knee chest stretch, where both knees are brought to the chest, the seated chest stretch which is done sitting up, and a partial sit-up stretch that is done with a person lying on the bed and bringing up their knee without using their arms.
7. Bird Dog Stretch
The bird dog stretch targets the core muscles while maintaining a neutral or normal spine curvature. Here are the steps for this stretch:
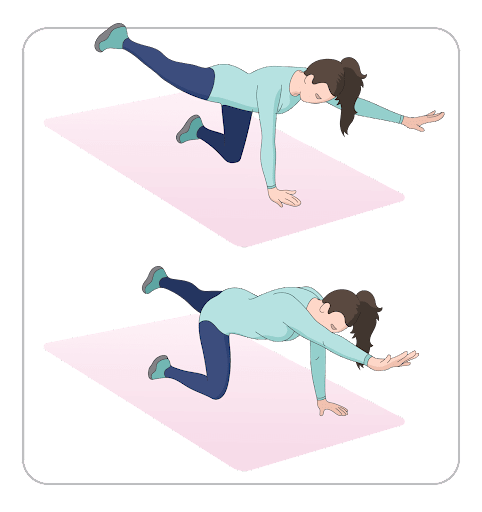
- Start on a mat on your hands and knees.
- Raise your right leg and left arm parallel to the ground.
- Tuck your chin inwards so that you are staring at the floor.
- Hold this for three breaths.
- Repeat with your left leg and right arm.
This exercise activates the erector spinae muscles of the lumbar spine. You can do this exercise two to three times in a single session.
8. Pelvic Tilting Exercise
Pelvic tilting exercises can help improve the range of motion of the lumbar spine and reduce lower back pain from DDD. The pelvic tilt exercises target the pelvic muscles like erector spinae, iliopsoas, and rectus femoris. Here are the steps:
- Lie on your back on the floor.
- Bend your knees and rest your feet on the floor.
- Activate your abdominal muscles and try to lift your pelvis so that it draws closer to your navel.
- Push your navel downwards and hold for 10 seconds
- Return to the starting position.
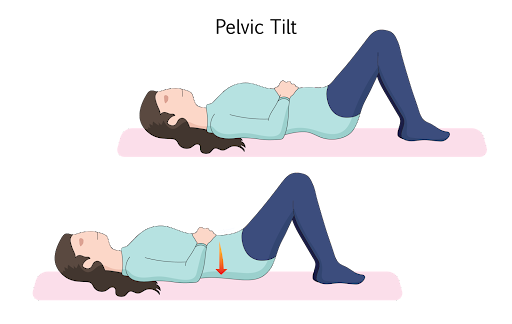
Repeat this two to three times. This exercise can also be done against a wall if you are uncomfortable on the floor.
9. Psoas Major Muscle Stretch
There are many exercises that can stretch the psoas major muscle. Some of these include the frog pose, side plank, and lunge stretches. Another stretch for the psoas major muscle is the glute bridge exercise. For this exercise, here are the steps:
- Lie down on the floor.
- Keep your hands flat against the ground.
- Raise your knees so your feet are flat on the floor.
- Lift the entire pelvis in the air and hold for 10 seconds.
- Return to the starting position and repeat.
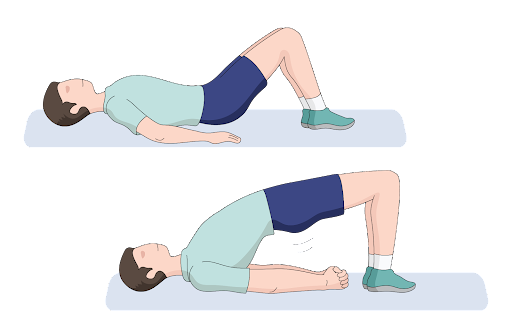
You can repeat this two to three times in a single session.
10. Lower Trunk Rotation Exercise
The lower trunk rotation exercise can help improve the flexibility, rotational movement, and range of motion of the lumbar spine. It can also help strengthen the pelvic and spinal muscles. These are the steps for the lower trunk rotation exercise:
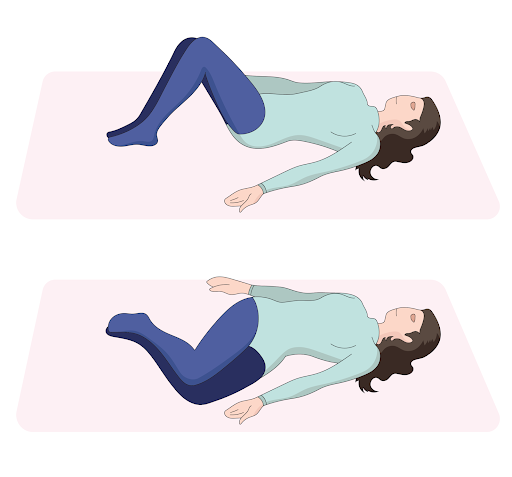
- Keep your back and feet flat against the floor.
- Bend your knees and bring them to one side.
- Hold for five seconds.
- Draw in your abdominal muscles and bring your knees to the other side.
- Hold for five seconds.
Try to do this exercise five times in a session.
Choose What’s Best For You
All of the exercises for DDD are designed to keep you active and your spine flexible and mobile. However, you do not have to do all these exercises. Your physio will direct you about the best exercises for you based on the extent of your degenerative disc disease. The best exercises for you will also depend on your current range of motion.
Precautions Before Doing The DDD Exercises
Disc degeneration exercises are helpful to improve blood flow and help you stay active. However, there are certain precautions you need to take before you do them. This includes:
- Start by consulting your spine specialist and physiotherapist about which exercises are good for you. The condition of your discs and spine will determine the best DDD exercises for you.
- When you begin DDD exercises, try to do them under the supervision of a physiotherapist. A physiotherapist will ensure you have the correct form and technique.
- Always warm up before you start any exercise. This will increase the blood flow to the muscles. Improved circulation will help supply more oxygen to the muscles thereby improving muscle contraction.
- Do the exercises within the prescribed range of motion. If you have any pain while doing them, stop immediately.
- Avoid putting any strain on the spine when lifting heavy weights, deadlifts, squats, or high-impact aerobic activity.
- Improve your posture so that even while you are exercising, you maintain a good posture.
- Change positions frequently. While you exercise, change up the movement every 10 minutes so that you are not overstraining one group of muscles or a particular part of the spine.
Additional Tips To Help Prevent Degenerative Disc Disease
You can prevent degenerative disc disease by taking a few preventive steps. This includes the following:
Smoking Cessation
There is strong evidence that suggests cigarette smoking leads to disc degenerative disease (4). This is a multifactorial process. Nicotine can reduce the proliferation rate and biosynthesis of cartilage in the disc cells by about 50%. Nicotine and several other compounds in cigarettes can also constrict the blood vessels which reduces the blood flow to the spine. This leads to a reduction of oxygen and nutrients to the spine. Cigarette smoking also leads to increased proteolytic or protein breakdown which weakens the spinal ligaments.
Quitting smoking can mitigate DDD to some extent. However, evidence shows that smoking cessation with cell-based treatment significantly improves disc health (5).
Weight Management
Data from population studies indicates a strong correlation between obesity and overweight body status with DDD (6). This is particularly in the case of the lumbar spine.
Increased compressive loading of the spine due to excessive weight and reduced blood flow due to the presence of plaques in the blood vessels are two causes of DDD in overweight individuals.
Therefore, it’s important to maintain a healthy weight. Body mass indices (BMI) vary according to height and ethnicity. Ask your doctor what the appropriate BMI range is for you.
Ergonomics In The Workplace
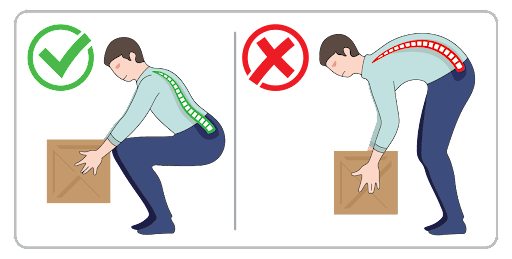
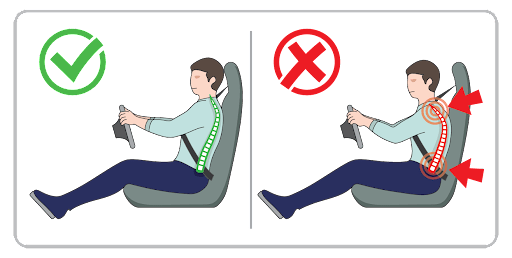
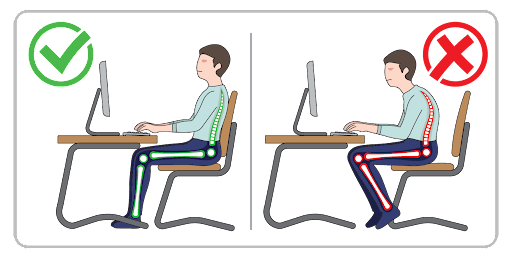
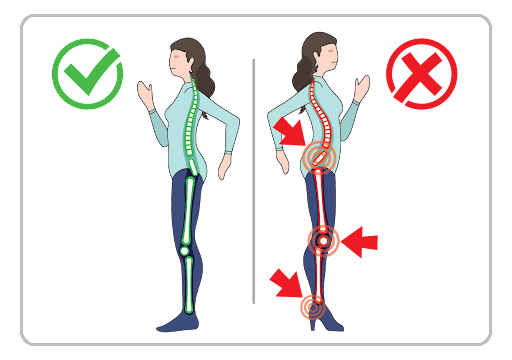
Your job may be contributing to DDD. At work, it’s important to have an ergonomic workspace. Some ways to practice ergonomics at work are:
- Use a swivel chair or an ergonomic chair if you have to sit for long periods.
- Take frequent breaks so that your muscles don’t get fatigued maintaining the spine in just one position. Muscles have to actively work to keep your back erect in a seated position. Sitting for hours in the same position will tire your muscles.
- Ensure your computer is at eye level.
- If you drive for long periods, try to place your knees and hips at the same level. This is the ideal position recommended by OSHA (Occupational Safety and Health Administration).
- Sit at an optimal distance of 10 inches from the steering wheel to ensure you’re not hunched over the wheel.
- If you have to do physical work, then take sitting breaks now and then.
- When lifting heavy items, always bend from your knees in a squat.
- You can only lift a maximum load of 25 kgs if the object’s height is at waist level. For objects at shoulder height, you can only lift a maximum of five kgs.
- If you have to rotate at work, then pivot with your feet. Don’t twist at your waist.
- Wear appropriate footwear. High-heeled shoes cause the spine to lean forward and put undue pressure on the knees and spine.
Healthy Diet
Diet plays an important role in spine health. There are various theories about this. The first suggests that vitamin D supplementation can improve DDD. Studies have shown that individuals with Modic changes (a MRI finding that indicates DDD) have lower vitamin D levels (7). Secondly, foods rich in antioxidants that reduce inflammation can improve DDD.
A diet rich in fortified cereals, oily fish like salmon and sardines, eggs, and exposure to natural sunlight can increase vitamin D levels. Antioxidant-rich foods including dark chocolate, fruits, sprouts, nuts, and vegetables can also help DDD by reducing inflammation. A diet low in fats can also help you maintain a healthy weight which will ease the pressure on the spine.
When Is Medical Intervention Needed?
These exercises may not be enough in cases where the DDD is advanced or is progressing rapidly. In some cases, exercise may not relieve your symptoms. Instead, some individuals may see an escalation of symptoms. If this happens, consult your spine specialist. Here are some signs and symptoms that require immediate medical attention:
- Severe back pain
- Tingling and numbness along the extremities
- Weakness in extremities
- Paralysis
- Bowel or bladder dysfunction
- One-sided sensory changes
- Radiating pain below the knee
- Unstable gait
- Sudden fever
Your doctor will address these signs and symptoms with immediate treatment, either surgically or with biological treatments. Biological treatments are protein-based therapies where biological factors are administered via an intradiscal injection. The factors are either given alone, with cells or tissue scaffolds, or with gene therapy.
Biological factors increase the synthesis of the matrix, delay degeneration, and can stop inflammation. At Centeno-Schultz, we are at the forefront of regenerative medicine. Our doctors highly recommend biological therapy for many of our patients.
Staying Active Can Make A Difference
It is important to stay active, even if you experience pain with degenerative disc disease. You don’t have to do all the exercises we listed, rather just do what is comfortable for you. Your physiotherapist and spine specialist can create a rehab program for you so you have a tailored exercise regime to help improve the range of motion of your spine. This may be just one aspect of your treatment for DDD, but it will go a long way to helping reduce its progression.
Do you want to know more about how to strengthen your spine using a safe approach? Talk to us and we will help you!
References
- Boden SD, McCowin PR, Davis DO, Dina TS, Mark AS, Wiesel S. Abnormal magnetic-resonance scans of the cervical spine in asymptomatic subjects. A prospective investigation. J Bone Joint Surg Am. 1990 Sep;72(8):1178-84.
- Lewis JS, Hewitt JS, Billington L, et al.: A randomized clinical trial comparing two physiotherapy interventions for chronic low back pain. Spine, 2005, 30: 711–721
- Sculco AD, Paup DC, Bo Fernhall, Sculco MJ. Effects of aerobic exercise on low back pain patients in treatment. Spine J. 2001;1(2):95–101. doi: 10.1016/S1529-9430(01)00026-2.
- Fogelholm RR, Alho AV. Smoking and intervertebral disc degeneration. Med Hypotheses. 2001;56(4):537-539. doi:10.1054/mehy.2000.1253
- Musich S, Faruzzi SD, Lu C, McDonald T, Hirschland D, Edington DW (2003) Pattern of medical charges after quitting smoking among those with and without arthritis, allergies, or back pain. American Journal of Health Promotion 18: 133–142.
- Sheng B, Feng C, Zhang D, Spitler H, Shi L. Associations between Obesity and Spinal Diseases: A Medical Expenditure Panel Study Analysis. Int J Environ Res Public Health. 2017 Feb 13;14(2):183. doi: 10.3390/ijerph14020183. PMID: 28208824; PMCID: PMC5334737.
- Seyithanoglu H, Aydin T, Taşpınar O, Camli A, Kiziltan H, Eris AH, Hocaoglu IT, Ozder A, Denizli E, Kepekci M, Keskin Y, Mutluer AS. Association between nutritional status and Modic classification in degenerative disc disease. J Phys Ther Sci. 2016 Apr;28(4):1250-4. doi: 10.1589/jpts.28.1250. Epub 2016 Apr 28. PMID: 27190462; PMCID: PMC4868222.
