The Centeno Schultz Clinic is committed to the highest standard of care with comprehensive evaluations performed by fellowship-trained physicians. We utilize a SANS approach to evaluate our patients, which is what has helped us identify the peripheral neuropathy.
Today I saw a patient in clinic who literally breaks my heart. Here is the tale of institution medicine gone bad.
Patient’s Leg Pain and Numbness Diagnosed as Peripheral Neuropathy?
RP is an 83-year-old Kaiser patient from San Diego with a three-year history of leg numbness and pain that was greater on the right than on the left. The onset of his leg symptoms was not associated with any trauma. RP’s numbness and pain involves the anterior thighs, knees, calves, and feet, and virtually any activity aggravates these leg symptoms. Even walking is difficult and requires the use of a cane, and the patient’s feet feel like “blocks of wood.” Interesting enough, he denied any low-back pain or stiffness.
Treatment to date had been limited to conservative care: physical therapy, massage, heat, and ice. He underwent a single epidural steroid injection with very limited benefit. Like many similar patients, RP has been directed from one clinic to the next and ultimately was informed that his leg numbness and weakness was due to peripheral neuropathy. Peripheral neuropathy is a condition that occurs when there is some type of irritation, injury, or disease affecting the peripheral nerves (the nerves that carry signals to and from the central nervous system). Lyrica was prescribed for RP.
A Review of RP’s Lumbar MRI
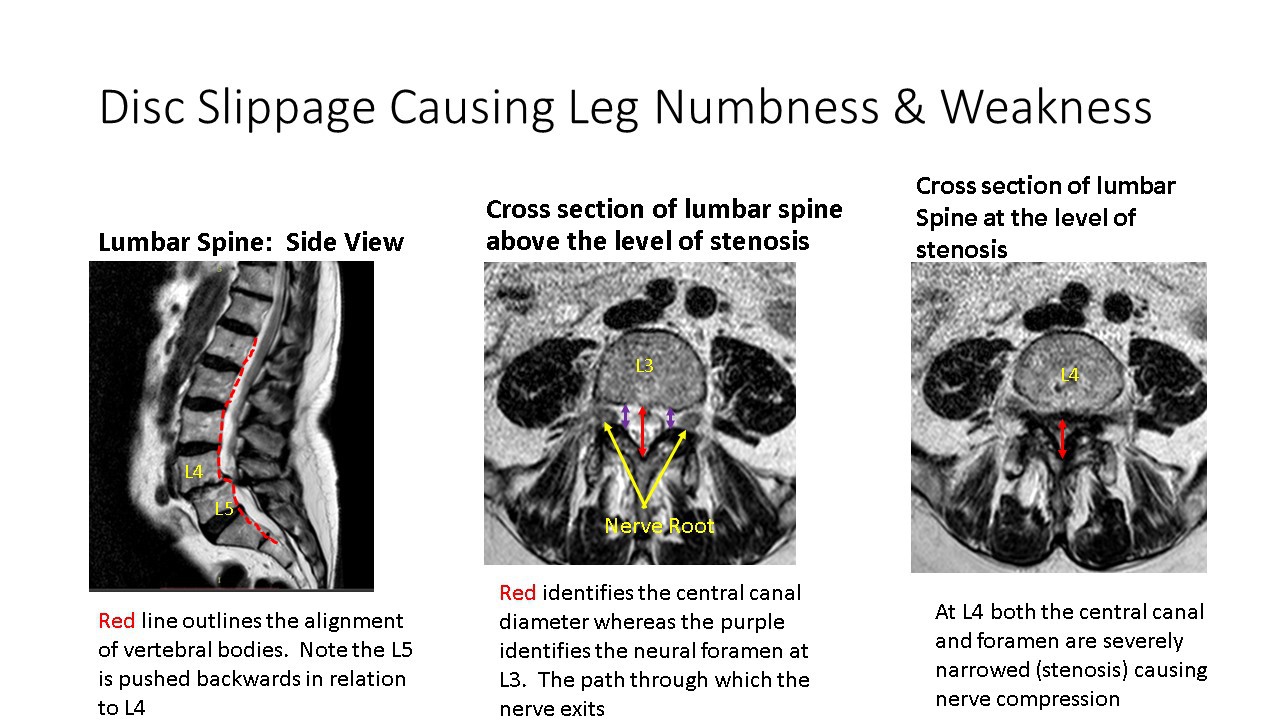
Above is RP’s lumbar MRI. The image on the left is the side view of RP’s spine. Note the red line along the posterior aspect of the vertebral bodies. There is significant misalignment. The L5 vertebral body is pushed backward in relation to L4.
The image in the middle is a cross-section view at L3/4 disc level, which is relatively normal.
The image on the right is a cross-section view at L4/5, which is significant for narrowing of the central canal and foramen, where the nerves exit. The L4/5 disc is darker in color and shorter in comparison to the other discs.
On the middle slide, note the white spinal fluid that surrounds the spinal cord. A red line with arrows on both sides spans the diameter of the central spinal canal. Also note the yellow arrows that point to the exiting nerve roots. The exiting nerves must go through the foramen identified by the purple lines with arrows. These are the same nerves that provide strength and sensation to your legs and feet.
Note slide to the far right. The spinal canal and fluid is severely reduced in size consistent with central canal stenosis. The existing nerve roots are not visible as they are severely compressed due to misalignment of vertebral bodies, disc protrusion, and overgrowth of facets. This is referred to as severe foraminal stenosis. The foramen is the doorway through which the exiting nerve root leaves the spinal column.
RP’s Leg Pain and Numbness NOT Due to Peripheral Neuropathy
RP’s leg numbness and weakness was NOT due to peripheral neuropathy but rather the severe central and foraminal stenosis at L4/5 due to misalignment of the vertebral bodies.
RP underwent platelet-rich plasma (PRP) epidural facets and ligament injections at the Centeno-Schultz Clinic. The goal was create stability in the spine and improvement in nerve function, which hopefully will translate to improved feeling and strength in his legs and feet.
A very sad part of this story is that when compared to the 2010 lumbar X-ray, there had been significant progression in the disc slippage and stenosis. That’s right! Eight years had lapsed, and nobody recognized or addressed the lumbar injury, which has progressed.
Bottom line? If you have ongoing pain or dysfunction that has not responded to treatment to date or you have been given a diagnosis such as fibromyalgia or “peripheral neuropathy,” you may wish to consider a second option at the clinic where stem cells were invented: Centeno-Schultz Clinic