Pes Anserine Bursitis
Causes, Symptoms, Treatment Options, & Other Resources
Knee pain located at the lower inside of the knee can be caused by Pes Anserine Bursitis, which is irritation of the tendons that run on the inside aspect of the knee. Commonly mistaken for arthritic pain, meniscal pain, and sometimes nerve pain from the low back! Don’t be misdiagnosed, and let’s dive in below to get a better understanding of Pes Anserine Bursitis.
What Is Pes Anserine Bursitis?
The Pes Anserine Bursa is a bursa that surrounds 3 tendons of the leg. A bursa is a thin, slippery, sac-like film that contains a small amount of fluid. A bursa is found between bones and soft tissues in and around joints. It cushions and protects joint structures and stops them from rubbing against each other. If a bursa becomes inflamed and irritated, it’s known as bursitis.
The Pes Anserine Bursa surrounds 3 tendons as they attach a few inches below the medial (inside) knee joint:
- Sartorius: Synergistic muscles that can help flex, abduct and rotate the femur. It can also flex and medially rotate the leg. Sitting cross-legged demonstrates all four actions of the Sartorius.
- Gracilis: The most superficial and medial of the muscles at the medial compartment of thigh. The muscle adducts, medially rotates (with hip flexion), laterally rotates, and flexes the hip as above, and also aids in flexion of the knee.
- Semitendinosus: The Semitendinosus muscle is one of three hamstring muscles that are located at the back of the thigh.
These three muscles work collectively to flex the knee and extend the hip. All 3 of the muscles that make up the Pes Anserine are unique in that they cross both the hip and knee, meaning they can move both joints (hip and knee).
Symptoms of This Condition
Burning Pain on Outside of Knee When Kneeling
There are many possible causes of burning pain on the outside of the knee while kneeling. One possibility is that you may have patellofemoral syndrome, which is a condition that results in pain around the kneecap. This pain can be aggravated by activities such as kneeling or squatting. Other potential causes of this type of pain include iliotibial band syndrome, runners knee, and meniscal tears. If you are experiencing burning pain on the outside of your knee while kneeling, it is important to see a doctor for evaluation. Some of these conditions can be treated with conservative measures such as rest, ice, and physical therapy…
Read More About Burning Pain on Outside of Knee When KneelingHamstring Pain Behind Knee
Hamstring pain behind the knee is a real problem, but many people are unaware of its severity. The hamstring muscle group spans the back of the thigh and consists of three muscles – Biceps Femoris, Semimembranosus, and Semitendinosus. Pain in the posterior aspect/backside of the knee has to do with one of three hamstring muscles. These can be roughly categorized as follows: Pain in the lower portion of the hamstring (semitendinosus and semimembranosus) is typically due to an injury sustained at their origin, or where they attach; this may be referred to as ‘insertional pain’. Pain located in the middle portion of the hamstring…
Read More About Hamstring Pain Behind KneeHamstring Pain when Sitting
The hamstring is composed of the three long muscles that are found on the back of the upper leg. These are semitendinosus, semimembranosus, and biceps femoris. All three muscles run down the length of the thigh before they join together to become one tendon that attaches itself to the backside of the lower leg bone, called the Fibula. When these tendons contract it pulls the lower leg downwards towards our feet. The muscle contracts concentrically as it shortens. And relaxes eccentrically as it lengthens. This contraction action is also known as knee flexion. When these muscles are weak or injured it can be difficult to stand on…
Read More About Hamstring Pain when SittingKnee Buckling
Knees can buckle, causing a sensation of one or both knees giving out that affects nearly 17% of adults. The knees are regarded to be one of the most essential (and biggest) joints in the human body because they play significant roles in basic activities such as walking and sitting. When our knees begin to feel unstable, weak, or begin giving out, it is easy to become stressed since we rely so heavily on them for movement. The knee can become stable from numerous types of injuries. The knee is kept stable by the following structures: Tendons attach the leg muscles…
Read More About Knee BucklingKnee Hurts When I Bend It and Straighten It
Your knees bend countless times throughout the day. Running up the stairs, down the hall after kids, and getting into the car. You straighten the knee as you walk, descend stairs or get into and out of the car. Bending and straightening the knee are necessary for daily activities. Knee pain with bending or straightening may be a mild, transient irritation or may indicate a more significant problem. Learn more below and avoid further injury and dysfunction. Knee pain can vary significantly depending upon many factors including the actual source of the pain, the severity of the injury, general health, and level of activity…
Read More About Knee Hurts When I Bend It and Straighten ItKnee Pain
Knee pain can be caused by many factors. Overuse injuries, direct trauma to the knee and arthritis are the most common causes of knee pain. Damage to the knee structures may cause swelling, scar tissue formation (fibrosis), and loss of function of the joint. Pain is often accompanied by difficulty walking, weakness, and instability. When the knee is overused, the thigh and shin bones (femur and tibia), cartilage, or tendons may experience stress. This leads to pain and discomfort as well as stiffness in the knee. Overuse injuries are common among athletes who participate in sports that involve running, jumping…
Read More About Knee PainKnee Swelling
Swelling of the knee, also known as water on the knee, is a condition in which fluid collects around the knee joint. Swelling can occur for a variety of reasons and affect patients of any age. Some swelling can be treated with over-the-counter medicines, but persistent and continuous swelling might result in tissue damage, bone softening, and cartilage deterioration. Over-the-counter medicines will assist relieve pain for individuals with a history of osteoarthritis and swelling following physical activity, such as exercise or running. During and after activity, the patient may apply compression sleeves to reduce the inflammation. Ice is another method…
Read More About Knee SwellingPain Behind Knee
First off, this is where the hamstrings and calf muscles attach. They have tendons here that are inserted into the bone. So if there’s a problem in the muscle or the tendon, you’re going to feel it right here. This is also where deep muscles like the popliteus and plantaris live. So, if these have issues, you’re going to feel it in the back of the knee. In addition, the tibial nerve is back here. So if there’s an issue with a nerve in your back or a nerve locally, behind the knee, you’re going to feel it here. And the meniscus or the joint spacer lives back here. And the meniscus or the joint spacer lives back here. So a tear in the meniscus could cause pain…
Read More About Pain Behind KneeTight Hamstrings & Calves
The hamstrings are a group of muscles in the upper leg. They are located on the backside of the upper leg and are comprised of three muscles: biceps femoris, semitendinosus, and semimembranosus. The calf muscles are located on the backside of the lower leg and are comprised of two muscles: the gastrocnemius and soleus. Tight hamstring and calf muscles can be painful, limiting someone mobility. They also make lower extremity muscles more vulnerable to injuries. Tight hamstrings and calves can arise from different sources which include: medication, muscle and tendon injury, overuse, muscle imbalance, dehydration, poor posture, low back injury…
Read More About Tight Hamstrings & CalvesTightness in Knee
What could tightness in your knee mean? When fluid builds up inside the knee as a result of an injury, overuse, or medical problem, the knees become swollen and tight. Swelling might be mild, so you may not always notice it unless it is serious damage. You may feel this as stiffness in the knee since swelling may not be visible. Swelling restricts movement since there is less room in the knee. Fluid buildup can be caused by irritation, internal bleeding, and injuries to the knee. Arthritis, gout, tumors, and baker cysts are all causes of swelling. Pain and swelling are the responses of your body to damage. Together they can lead to stiffness in your knee…
Read More About Tightness in KneeOne of the hallmarks and distinguishing aspects of Pes Anserine Bursitis is that the knee pain is below the medial (inside) joint line. You can easily palpate the joint line of the knee and then 2 to 3 inches below the knee joint on the inside of the lower leg.
Pain And Tenderness Inside The Knee
Palpate the 2-3 inches below the joint line (see Figure 1), and if this area is very tender to even light touch, it is highly likely that you can have Pes Anserine Bursitis.
The Pes Tendons Get Irritated with Repetitive Motion / Knee Flexion
When inflamed, the pain increases with exercise or climbing stairs but if there is excessive inflammation, pain can be at rest with the knee flexed, such as in a sitting position.
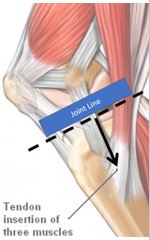
Common Causes of Pes Anserine Bursitis
Tendons of the Pes Anserine act on both the hip and knee, so repetitive motion and overuse of both the hip and knee can lead to excessive stress on the tendons.
Overuse Seen in Multiple Movements
We see a lot of athletes, but they are not the only ones that do repetitive activities. Repetitive activities, like squatting, stair climbing, and other work or household activities can be the cause of overuse of a joint.
Osteoarthritis
Numerous studies have shown the strong association of Pes Anserine Bursitis in Osteoarthritis patients.
Incorrect Physical Training Techniques
This can include things such as a lack of stretching, big distance jumps in training or too much uphill running.
Tight Hamstring Muscles
Tight hamstrings are a common cause of Pes Anserine Bursitis.
Obesity
Examination and Diagnosis
Getting the correct diagnosis is key! Getting to the right diagnosis takes time to discuss your pain. We typically begin with determining the “OLD CARTS” which is a cheat code for recalling the history of your pain, and it stands for Onset, Location, Duration, Characterization, Aggravating, Relieving, Treatments and Severity. This information quickly gives insight into a possible diagnosis.
Next comes the examination part, inspecting for any abnormal alignment (valgus or varus), palpating all structures around the knee, and putting the knee through stress maneuvers to see if anything recreates the pain.
Lastly during evaluation any sports medicine or musculoskeletal doctor (PM&R, orthopedic surgeon) when evaluating any knee conditions has to use diagnostic ultrasound during their evaluation and examination. This can easily help differentiate say a meniscus tear versus Pes Anserine Bursitis (see Figure 2, below). Diagnostic ultrasounds are now a standard of care for most orthopedic problems, helps coming up with a concrete diagnosis during your visit so we can move forward talking about how best to treat the problem to get you back to doing what you love to do, without pain.
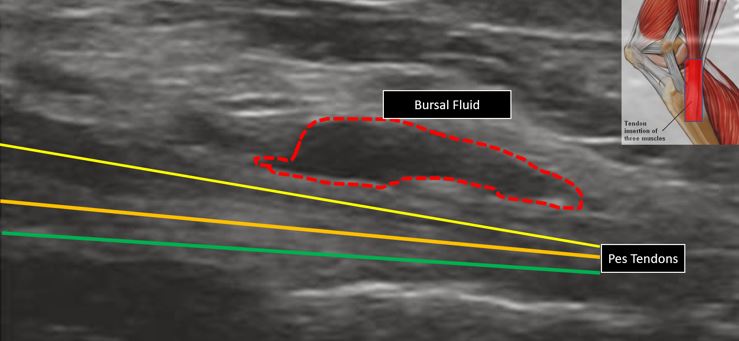
Once we have a solid diagnosis of Pes Anserine Bursitis, we can move on to discussing the more important issues – like how to treat it! Bursitis = inflammation of the bursa which can come from overuse / repetitive trauma or from the Pes tendons becoming damaged and swollen. Treatments start with conservative care and then increase invasiveness.
- Rest it for a few weeks to allow the body to take care of it.
- Ice Packs or Heat packs can help calm down the inflammation.
- Anti-inflammatory Medication both over the counter or supplementations – to learn more about best options read a previous blog about NSAIDs:
- Physical Therapy can help increase the strength of the Pes tendons and use modalities to help flush the inflammation out.
- Anesthetic and Steroid Injections can help temporarily and as well confirm the diagnosis if all the pain goes away but any injection should be done under ultrasound guidance to avoid the nerves / vessels of the area and to NOT get in the tendon …. Potentially for tendon rupture if that happens!
- Surgery is rarely needed for Pes Anserine Bursitis but many more invasive procedures can be done such as Radio Frequency Ablation (RFA) to the local nerves to dull the pain (1).
Regenexx: A Revolutionary Treatment Method
Over the last 20 years, research has gone beyond corticosteroids for orthopedic injuries. The development of Platelet-Rich Plasma has successfully been able to help most orthopedic conditions as well as reduce the surgical conversion rates of common tendon issues like Pes Anserine Bursitis! Being the HQ of Regenexx, we continue to research how to maximize the concentration and tailor-make our PRP treatments to specific orthopedic conditions, thus maximizing our clinical results.
“Patient outcomes are the #1 priority at Regenexx. Our lab processing of blood platelet mixtures is far more labor intensive than the automated centrifuge used by others, but we are able to create customized solutions for our patients, with platelet mixtures that are purer and more concentrated.”
Dr. Chris Centeno
Over the last 15+ years, Regenexx has pioneered orthobiologics with maximization of outcomes using the most up-to-date precise ultrasound-guided imaging to ensure we treat the right area! We have termed this as “Interventional Orthopedics” To learn more about these advanced image-guided treatment options.
Is Pes Anserine Bursitis Preventable?
Seeing a physical therapist can set you up with a home exercise program to strengthen and stretch the muscles around your knees, upper legs, and abdomen to help prevent the onset or recurrence of Pes Anserine Bursitis. Working on mobility, stability, and strength of the kinetic chain can help prevent not only Pes Anserine Bursitis but also reduce the risk of multiple other injuries in your lower extremities.
Here’s a Simple Checklist:
- Learn correct knee positioning when participating in athletic activities.
- Follow a consistent flexibility and strength exercise program, especially for the leg and hip muscles, to maintain good physical conditioning.
- Practice balance and agility exercises and drills.
- Always warm up before starting a sport or heavy physical activity.
- Avoid sudden increases in running mileage or uphill running, gradually build loads over time.
- Wear shoes that are in good condition and fit well.
- Maintain a healthy weight and eliminate high sugar foods and processed foods.
- Treat and manage Diabetes, as managing your glycemic control helps prevent musculoskeletal injuries.
- Wear orthotics to reduce flat feet and valgus (knock-knee) positioning of the lower extremities.
- Wear a knee brace to support the knee and reduce strain on the inside of the joint when doing high stress activities.
Recovery Period
For tendons (like in Pes Anserine Bursitis) the soreness can last longer and the effects could take up to 3-4 months to be fully appreciated. For ligaments, there may be a “honeymoon” period of 1-2 weeks where loose ligaments are swollen and as such, provide better stability during that time, but then the initial swelling goes away and the pain and instability come back (2). The full effects, like in tendons, can take a few months to be seen.
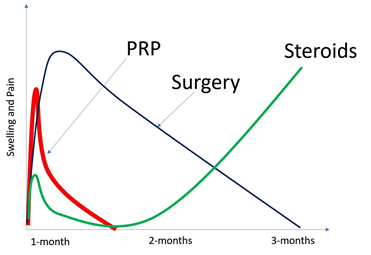
BUT Not All PRP Is Created Equal.
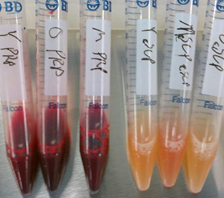
There are two main types of PRP: red and amber. Red PRP has red and white blood cells, so in my experience, it causes more of a flare-up for longer. Amber PRP has few red or white blood cells, so it causes less of a flare-up and if that happens, the flare-up doesn’t last as long.
Also, realize that the degree of post-PRP injection flare-up can be due to your body’s own level of systemic inflammation and where the PRP was injected, or how aggressively the procedure disrupted the tissues.
Successful Treatment Is Possible for Pes Anserine Bursitis
At Centeno Schultz Clinic, we have dedicated our practice to delivering the highest quality orthopedic care possible. We have a three-prong approach:
- Spending an hour with patients during initial evaluations to ensure we have the most accurate diagnosis and discussing all options with patients to develop a comprehensive treatment plan (which may or may not include biologics).
- Continuing research in biologic therapy such as PRP and Bone Marrow Concentrate (containing stem cells) utilizing our Flexible Lab Platform to maximize platelet-based therapies and beyond.
- Continuing to innovate injection techniques to ensure precision guidance of biologics to target areas. All physicians at CSC are trained in both xray based and ultrasound image guidance to ensure the best possible treatment for your knee condition.
If you have been dealing with Pes Anserine Bursitis or an orthopedic condition and would like an in-depth evaluation with a comprehensive treatment plan, sign up for an evaluation today!
Deep Dive Into Your Treatment Options
NSAIDs
The other day I was evaluating a patient and reviewing the treatment options for their spine condition. After discussing prior treatments, we got to the topic of medications taken for pain relief. She explained that she mainly utilized anti-inflammatory (NSAID) medications and then she told me to hold much she takes and has been for many years…..she takes close to 2 grams (2000 milligrams) on a daily basis which equated to about 9-10 capsules of medication per day. I was shocked, considering she was pre-diabetic and with high blood pressure plus the kicker of it is that her PCP (primary care physician) is ok with this…
Read More About NSAIDsPRP Knee Injections
PRP stands for Platelet-Rich Plasma. Platelets are blood cells that prevent bleeding. They contain important growth factors that aid in healing. Plasma is the light yellow liquid portion of our blood. So PRP is simply a concentration of a patient’s own platelets that are suspended in plasma and are used to accelerate healing. PRP is NOT stem cell therapy. Regrettably, blood contains few circulating stem cells. Rich sources of stem cells are bone marrow and fat. PRP is rich in growth factors. There are many different types of growth factors with different properties. VEGF is a very important one as it can increase the blood flow to an area.
Read More About PRP Knee InjectionsOur Doctors That Can Assist With Pes Anserine Bursitis

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics. He is board-certified in physical medicine and rehabilitation with a subspecialty of pain medicine through The American Board of Physical Medicine and Rehabilitation. Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who…
Read more
John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreOther Resources for Pes Anserine Bursitis
Free Download: The Knee Owner’s Manual

This e-book by Dr. Chris Centeno examines the knee and its role in the human musculoskeletal system and the body as a whole. The Knee Owner’s Manual provides a series of tests and clearly defined exercises that you can perform on your own to assess and monitor your own knee health. It will allow you to look for trouble spots where your own body may be having difficulty with stability, articulation, symmetry, and neuromuscular function. You’ll be able to see how these deficits in other regions of the body relate to the knee.
The Knee Owner’s Manual also discusses how Regenexx is pioneering the development of interventional orthopedics, a new branch of medicine that employs regenerative biologic therapies such as adult bone marrow concentrate and platelet-rich plasma to help repair and strengthen damaged tissues in other areas of the body.
This is contrasted with invasive knee surgeries, which often remove important tissues or replace the entire knee itself when it becomes damaged. With hyperlinks to more detailed information, related studies, and commentary, this book condenses a vast amount of data, images, and resources into an enjoyable and informative read. This is the first edition of The Knee Owner’s Manual, a companion book to Orthopedics 2.0.
-
Knee Pain Location Chart: Know What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
Learn About Your Knee Pain Symptoms To Get The Best Treatments
Knee pain affects about 25% of the population (1). The knee joint involves three bones, namely the patella, the femur, and the tibia. Knee pain can be a sign of damage to the ligaments, bones, bursae, or muscle tendons because there are so many structures within the knee joint. In this post, we’ll discuss the…
-
What is a Cervical Disc?
There are 23 discs in the spine: 6 in the cervical region (neck), 12 in the thoracic region (middle back), and 5 in the lumbar region (lower back). The disc’s function is to provide flexibility and stability to the spine. The disc absorbs approximately 70% of the forces placed on the spine in multiple movements…
References
- Conger A, McCormick ZL, Henrie AM. Pes Anserine Tendon Injury Resulting from Cooled Radiofrequency Ablation of the Inferior Medial Genicular Nerve. PM R. 2019 Nov;11(11):1244-1247. doi: 10.1002/pmrj.12155. Epub 2019 May 24. PMID: 30859692.
- Xu Q, Chen J, Cheng L. Comparison of platelet rich plasma and corticosteroids in the management of lateral epicondylitis: A meta-analysis of randomized controlled trials. Int J Surg. 2019 Jul;67:37-46. doi:10.1016/j.ijsu.2019.05.003