Entrapped Nerve Hydrodissection – Carpal Tunnel Surgery Alternative
Am I a Candidate?Carpal tunnel syndrome (CTS) is the most common nerve compression problem of the upper limbs. It happens when the median nerve gets compressed in the wrist, commonly by swollen tendons and repetitive use. In addition, we frequently see it in patients with neck problems, also known as double crush syndrome.
Carpal tunnel syndrome affects about 1% of the general population and 5% of the working population and surgical treatment for carpal tunnel syndrome is the most frequent surgery of the hand and wrist. But do these patients really need surgery?
In our clinical experience, a new technique called nerve hydrodissection may be the better answer for some patients.
What Is Hydrodissection of the Nerve?
Although nerves are supposed to move freely through tissue, they can become entrapped and stick to surrounding tissues due to trauma, surgical scar tissues, inflammation, certain anatomical features, and conditions like pregnancy or obesity. This can lead to pain, numbness, and even paralysis, and may cause entrapment neuropathy – a common but frequently underdiagnosed source of pain.
Nerve hydrodissection is a minimally invasive, non-surgical medical procedure used to address nerve entrapment and nerve compression conditions (e.g.: carpal tunnel syndrome). It uses the injection of fluids to free up scar tissue or adhesions (two surfaces, usually separate, that are joined by scar tissues) that are trapping or compressing a peripheral nerve.
Using ultrasound guidance to accurately guide the needle to the target location, a specialist will inject a solution composed of anesthetic, saline, and, sometimes, dextrose in water in the target location. The solution will break apart – or “dissect” – nerves from the surrounding tissues, thus reducing pressure and irritation and improving symptoms, mobility, and quality of life.
How the Procedure Is Done
Rather than an open surgery, a doctor can perform this procedure using a needle under careful ultrasound imaging guidance. We inject small amounts of fluid around the nerve to “free up” the median nerve (which can become scarred and adhere to its surrounding tendons).
This allows the nerve to glide more easily and, many times, has the same effect as a surgical release where the numbness, tingling, and pain go away. We have also used Regenexx-SCP to perform this procedure, hoping autologous, regenerative solutions will also help the nerve repair.
And there you have it, nerve hydrodissection.
How Many Treatments Are Required?
Sometimes, just one treatment is required to achieve the desired results. However, often, patients require more than one treatment – usually three to six sessions – to see long-lasting improvements.
A 2020 study shows that patients experience considerable pain relief within 15 minutes of the first treatment, but an average of 3.8 sessions is required to tackle the root of the problem and ensure lasting relief from pain, tingling, and numbness.
The number of treatments required varies depending on factors like:
- The diagnosed condition
- The severity of the condition
- The patient’s physical health
- Individual tissue response
- Recovery progress
- The advice of the physician
Given these variables, a patient-tailored approach becomes key in determining the precise number of treatments needed.
Nerve Hydrodissection Recovery Time
One of the greatest advantages of choosing hydrodissection over invasive procedures is that this treatment does not involve risks or lengthy recovery times. Following the procedure, you are likely to experience a rapid decrease in pain levels, as well as improvements in mobility and quality of life.
Ache from the injection may last around two or three days, but there is no required downtime after this treatment, and you can return to your normal life the day after the procedure. Your doctor will provide you with all the information needed to look after the site of injection and prevent complications like infection or swelling.
Post-treatment instructions, such as minor activity modifications and lifestyle guidance (i.e. practicing nerve gliding exercises and maintaining healthy habits), can also help boost the effectiveness of the treatment.
Other Conditions That Can Be Treated with Hydrodissection
Besides CTS, hydrodissection can be effectively used in the treatment of several conditions that stem from the entrapment or compression of peripheral nerves.
These include:
- Thoracic outlet syndrome (TOS)/brachial plexus neuritis. TOS is a complex medical condition where blood vessels or nerves (95% of cases are neurogenic) between your collarbone and your first rib (this area is called the thoracic outlet) get compressed. This can result in pain in your shoulders and neck, and numbness in your fingers.
Common causes of this condition include repetitive stress and sudden injuries to the neck (e.g. whiplash from a car accident). Hydrodissection can help re-establish space around compressed nerves in the lower neck and upper chest. - Radial nerve or posterior interosseous nerve (PIN) entrapment. This is a clinical condition resulting from the compression of the radial nerve or its branches (like the PIN), at the level of the elbow and wrist. The radial nerve supplies areas of the forearm, wrist, and hand, and, when it malfunctions, it can impact the sensory and motor functions of the arm.
Common causes include sustained forceful activities (e.g. gripping or pinching), direct trauma like fractures or dislocations, and repetitive actions that stress the nerve. In some cases, lesions such as tumors, cysts, and scar tissue can also occupy the space around the nerve, causing entrapment. - Pronator teres syndrome. This is a rare neuromuscular condition stemming from the entrapment of the median nerve near the elbow. It causes pain, numbness, and a tingling sensation in the forearm and hand. This syndrome occurs due to repetitive overuse of the forearm, heavy lifting, or direct trauma. Strain and compression of the median nerve can be eased by hydrodissection.
- Cubital tunnel syndrome. CTS stems from undue pressure on the ulnar nerve in the elbow region. It causes numbness or tingling in the ring and small fingers, pain in the forearm, and weakness in the hand.
CTS occurs due to repetitive or forceful bending of the elbow, prolonged flexion, fluid buildup, or pressure on the elbow due to certain habits or physical activities (e.g. lifting or throwing). Hydrodissection can help relieve inflammation and scar tissue in the cubital tunnel, which houses the ulnar nerve. - Meralgia paresthetica (lateral femoral cutaneous neuropathy). This is a nerve disorder characterized by numbness, tingling, or a burning sensation in the outer part of the thigh. This condition is usually due to compression or damage of the lateral femoral cutaneous nerve, which provides sensation to the skin surface of the thigh.
Most cases of meralgia paresthetica occur when the lateral femoral cutaneous nerve is compressed or squeezed as it exits the pelvis, a condition that can be relieved through hydrodissection. - Piriformis syndrome. This neuromuscular disorder occurs when the sciatic nerve is compressed by the piriformis muscle, leading to pain, numbness, and tingling along the path of the nerve, which connects the buttock to the lower leg.
It is associated with hypertrophy or spasms of the piriformis muscle, which occur due to trauma, overuse, or prolonged sitting. Hydrodissection can separate the muscle and the nerve and break down adhesions, leading to symptom relief and nerve decompression. - Fibular nerve/peroneal nerve entrapment syndrome. This condition occurs when the peroneal nerve in the leg gets compressed, leading to foot and ankle pain, numbness, and a condition known as foot drop.
Causes include habitual leg crossing, injuries like knee dislocation and fractures, compression due to a tight plaster cast, prolonged bed rest, or complications from surgical procedures that involve the knee or hip. Hydrodissection can be an effective treatment to free the nerve from surrounding structures like the fascia or muscles. - Tarsal tunnel syndrome. This neuropathic disorder is triggered by pressure on the posterior tibial nerve as it traverses through the tarsal tunnel, which is a narrow passage located just below the bony part on the inside of your ankle.
This syndrome results from injury, anatomical anomalies, systemic diseases, or repetitive stress, and causes numbness, tingling, burning sensations, and sharp, shooting pain in the ankle and foot. Hydrodissection can relieve symptoms by increasing the spaces within the tarsal tunnel, thus relieving the pressure on the posterior tibial nerve. - Morton’s neuroma/interdigital neuroma. This is a benign, non-cancerous thickening of the tissue around a nerve, usually in the third interspace between the toes. It is often caused by irritation or compression from wearing narrow, high-heeled shoes or participating in high-impact activities.
In simpler terms, it’s your body’s way of reacting to stress on the plantar digital nerve. Hydrodissection – coupled with activity and lifestyle modifications (e.g. choosing higher-quality shoes) – can relieve and decompress this nerve, which can help reduce the neuroma. - Scar neuropathy. This type of neuropathy is characterized by the dysfunction or damage of peripheral nerves, often resulting from a cutaneous scar, surgical intervention, or traumatic injury. By breaking down adhesions and scar tissues, hydrodissection can significantly reduce the symptoms of neuropathy and prevent permanent nerve damage.
How Centeno-Schultz Uses Hydrodissection for Carpal Tunnel
Given the unparalleled level of safety, lack of downtime, and excellent clinical outcomes, hydrodissection is quickly becoming an appealing alternative to nerve decompression surgery for millions of people struggling with CTS.
Nonetheless, not all hydrodissection therapies are equal: superior treatments, like the ones offered at Centeno-Schultz, will use imaging guidance for accuracy and injectable solutions entirely tailored to the patient’s needs and goals.
The visuals below offer a deeper dive into how the hydrodissection for CTS is performed at Centeno-Schultz.
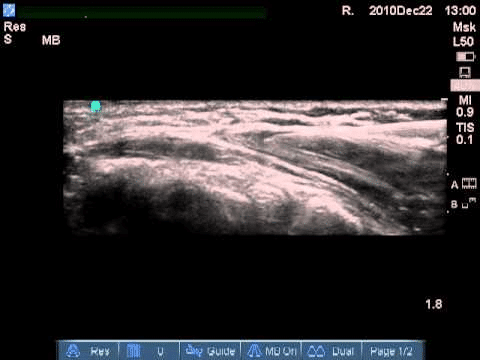
The video above shows a side section of the ulnar nerve at the elbow. The needle comes off from the right (light-colored line moving in and out of the frame) and comes up to the nerve. The dark material is fluid being injected around the nerve.
The video below shows an ultrasound cross-section of the wrist. The median nerve is the big oval structure in the middle.
The needle can be seen injecting fluid around the nerve, which is the dark material that seems to grow around the oval.
Again, since we did this through a needle without cutting or damaging important ligaments in the wrists, recovery time is much shorter than for surgery.
Patient Outcomes from the Procedure
No two cases of CTS will have the exact characteristics – nor will they have the same impact on life or prognosis. That is why it is important to find a line of treatment that is designed entirely around your clinical picture.
In the example below, you’ll see how the team at Centeno-Schultz uses a patient-centered approach to address the unique challenges of each person affected by nerve disorders.
Patient Case Report
KM is a 36-year-old woman who had arm pain for two years and who had an EMG/nerve conduction study, brain MRI and cervical MRI, all to figure out why her arm hurt. She also tried extensive physical therapy, which didn’t help.
The patient started on a fibromyalgia treatment program and was eventually referred for a diagnostic ultrasound to differentiate between tendon and nerve dysfunction in the arm.
Diagnostic ultrasound showed normal tendons, but revealed swelling of the ulnar nerve proximal to the flexor heads at the cubital tunnel and slight swelling of the ulnar nerve at the wrist (she felt this area most at work when the wrist was resting on her drafting table).
She underwent a diagnostic numbing injection of the ulnar nerve under ultrasound guidance, with decreased pain at the elbow and wrist.
At the same appointment, nerve hydrodissection made more room for her nerve through the cubital tunnel and around the wrist flexor heads by dissecting the tissue from around her nerve (also called hydro neurolysis).
She reported 100% relief from her pain. In this case, the ulnar nerve at the elbow was treated (not carpal tunnel at the wrist). This patient’s only other option would have been a risky surgery where the ulnar nerve would be moved to a different location (ulnar transposition).
Get Fast and Effective Relief from Carpal Tunnel Syndrome
Carpal tunnel syndrome can have a profound, debilitating impact on your life as a whole. But undergoing invasive procedures and extensive surgeries is no longer the only way out of pain and disability.
The hydrodissection treatments offered at Centeno-Schultz can help you regain your hand function, relieve symptoms, and lay the foundations for optimal neurological health.
Want to know more about the procedure to treat the condition you have? Read this article and learn about this non-invasive procedure.

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreAm I a Candidate?
To answer this question, fill out the candidate form below to request a new patient evaluation, and a patient advocate will reach out to you to determine your next steps. Your one-hour, in-office or telemedicine evaluation will be with one of the world’s experts in the field of Interventional Orthopedics.