Knee Arthritis
Every day we evaluate patients who have been seen by an orthopedic surgeon and have been told they need a total joint replacement. These surgeries require long recoveries and risk major complications so naturally, patients are looking for an alternative to allow them to return to their active lives without the need for such invasive procedures! By 2030, total knee replacement surgeries are projected to grow 673% to 3.5 million procedures per year, with the number one indication for total knee replacements being arthritis in the knee.
So let’s jump into the topic of knee arthritis…..what is it.…and what can be done to treat it without replacing the knee?
What Is Knee Arthritis?
In the human body, a joint is simply where 2 ends of bone come together. At the ends of these bones, there is a thick substance called “Hyaline Cartilage” that lines the ends. Hyaline cartilage is extremely slippery which allows the two ends of the bone to slide on top of each other. Then there is a capsule that connects the two ends filled with “synovial fluid” that acts as a further lubricant to make it more slippery!
Arthritis in the knee is defined by loss of the hyaline cartilage plus other changes that happen to the bone such as additional bone being laid down (bone spurs/osteophytes). The cartilage layer is worn down to the point of exposing the underlying bone they cover, with the severity of wear to the cartilage = the stage of arthritis.
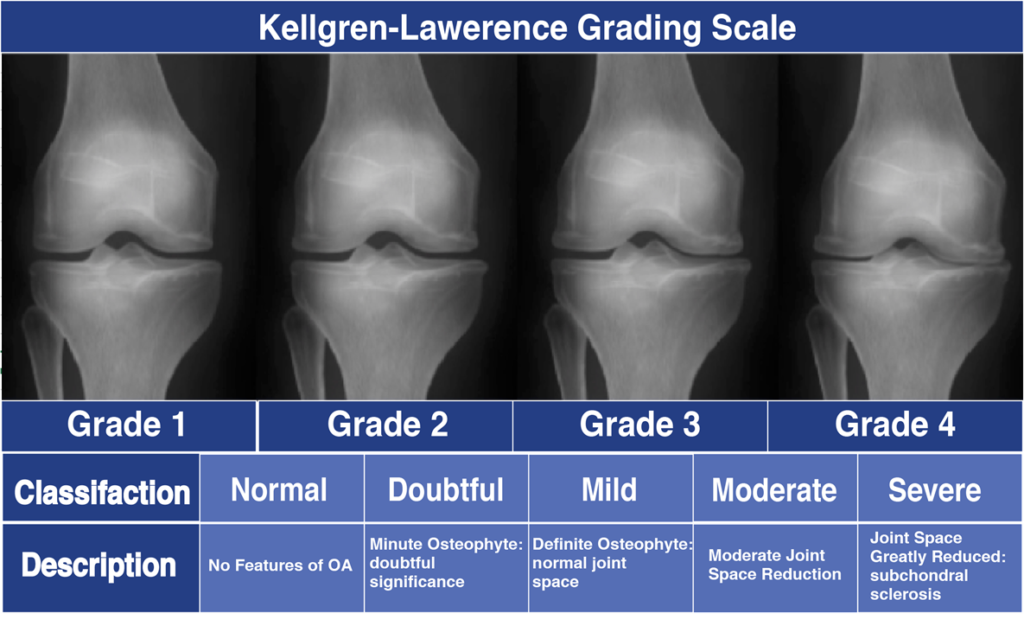
Historically the classification is based on an X-ray, which categorizes the cartilage loss by the joint space loss. X-rays cannot see cartilage but the space between the bones can give us an idea of the health of your cartilage.
Symptoms Related to Knee Arthritis
Anterior Lateral Knee Pain
The knee joint is one of the most complex joints of the human body. The femur, the tibia, patella, and fibula all contribute to this joint. They are held together by a myriad of strong ligaments that stabilize and support the joint. Anterior lateral knee pain is pain that occurs in the anterior and the anterior lateral region of the knee joint. A person may experience this pain front and center, in the outer aspect of the knee, or diffusely throughout the joint. The cause of the pain is some pathology in the anterior and lateral aspect of the knee.
Read More About Anterior Lateral Knee PainBack of Knee Swollen
Back of knee swollen? Swelling in the back of the knee is not something that is talked about too often. It can be uncomfortable or sometimes painful with the movement of the knee or, even with rest. It often stems from an orthopedic-related issue or, perhaps some other medical condition. Let’s dive in…What’s Causes Swelling in the Back of Your Knee? The back of the knee contains a variety of anatomical structures that can be affected and result in pain, swelling, numbness, tingling, etc. Muscles and tendons behind the knee that could be the source of pain or pathology could be one or more of the following: Gastrocnemius, Soleus…
Read More About Back of Knee SwollenBack of Knee Tight
Stiffness in the back of the knee can be a sign that there is damage or inflammation in the joint, arthritis, or a baker cyst. This might be due to an injury, overuse, or medical condition. If you are experiencing stiffness in your back knee, it is important to see a doctor determine the cause and get treatment. Common causes of stiffness in the back of the knee include: tight muscles, tendons, and ligaments, Injury to the joint or surrounding tissue, overuse such as from running or biking for long periods. Stiffness at night can potentially indicate damage to the joint…
Read More About Back of Knee TightBurning Pain on Outside of Knee When Kneeling
There are many possible causes of burning pain on the outside of the knee while kneeling. One possibility is that you may have patellofemoral syndrome, which is a condition that results in pain around the kneecap. This pain can be aggravated by activities such as kneeling or squatting. Other potential causes of this type of pain include iliotibial band syndrome, runners knee, and meniscal tears. If you are experiencing burning pain on the outside of your knee while kneeling, it is important to see a doctor for evaluation. Some of these conditions can be treated with conservative measures such as rest, ice, and physical therapy…
Read More About Burning Pain on Outside of Knee When KneelingCan’t Straighten Knee
Your knee is capable of moving in a number of directions. The most common are flexion and extension. Flexion is when you bend your knee and the shin bone moves towards the buttock. Knee extension is when you straighten out your knee. The extension is the opposite of flexion. PT, trainers, and physicians alike measure the degree of knee flexion and extension. When lying flat on an examination table or hard surface your knee should be able to extend so that there is no angle between the thigh and shin bone. The inability to straighten the knee is also known as an extension lag and is a reason for concern.
Read More About Can’t Straighten KneeFibular Head Pain
The proximal fibula is the part of the bone that lives just below the knee joint on the outside. It’s attached to the leg bone (tibia) via strong ligaments and there is a small joint here. There are many things that attach here, so it’s a critical point where pain can occur. There is a small joint between the fibula and the tibia known as the proximal tibiofibular joint. This is a plane-type joint which allows some sliding of the fibula on the tibia. It has cartilage just like the knee joint, so it can get arthritis which means worn down cartilage and bone spurs.
Read More About Fibular Head PainKnee Buckling
Knees can buckle, causing a sensation of one or both knees giving out that affects nearly 17% of adults. The knees are regarded to be one of the most essential (and biggest) joints in the human body because they play significant roles in basic activities such as walking and sitting. When our knees begin to feel unstable, weak, or begin giving out, it is easy to become stressed since we rely so heavily on them for movement. The knee can become stable from numerous types of injuries. The knee is kept stable by the following structures: Tendons attach the leg muscles…
Read More About Knee BucklingKnee Hurts When I Bend It and Straighten It
Your knees bend countless times throughout the day. Running up the stairs, down the hall after kids, and getting into the car. You straighten the knee as you walk, descend stairs or get into and out of the car. Bending and straightening the knee are necessary for daily activities. Knee pain with bending or straightening may be a mild, transient irritation or may indicate a more significant problem. Learn more below and avoid further injury and dysfunction. Knee pain can vary significantly depending upon many factors including the actual source of the pain, the severity of the injury, general health, and level of activity…
Read More About Knee Hurts When I Bend It and Straighten ItKnee Locking & Catching
Knees have the ability to bend forward and back, as well as rotate slightly. When a knee is unable to execute these actions, it impairs mobility and the capacity to complete daily chores such as sitting, standing, squatting, or kneeling. A locked knee occurs when a knee cannot be bent or straightened so it gets stuck or feels locked in a certain position for an extended period of time. There are two forms of locked knees: one that is due to inability to move because of an actually physical or mechanical restriction and there is one that feels locked due to the pain involved in moving it. When a person has their knee joint effectively frozen into place and cannot move, this is known as a true locked knee….
Read More About Knee Locking & CatchingKnee Making Crackling Sound
Crepitus is the medical term for this cracking or catching sensation. It can affect various regions of the body, but it is most common in the knee. It can happen due to air bubbles forming in bodily tissues (this is what happens most of the time), but it can also happen as a result of patellofemoral syndrome, damaged cartilage, osteoarthritis, or other conditions. Patients describe the sound of the popping with the following terms: popping, snapping, catching, clicking, crunching, cracking, crackling, creaking, grinding, grating, and Clunking. When Should You Be Concerned? When the crackling is accompanied by pain and/or the feeling of instability in the knee, that’s a good time to consult a physician. If the cracking is also associated….
Read More About Knee Making Crackling SoundKnee Pain
Knee pain can be caused by many factors. Overuse injuries, direct trauma to the knee and arthritis are the most common causes of knee pain. Damage to the knee structures may cause swelling, scar tissue formation (fibrosis), and loss of function of the joint. Pain is often accompanied by difficulty walking, weakness, and instability. When the knee is overused, the thigh and shin bones (femur and tibia), cartilage, or tendons may experience stress. This leads to pain and discomfort as well as stiffness in the knee. Overuse injuries are common among athletes who participate in sports that involve running, jumping…
Read More About Knee PainKnee Popping
Knee popping can be a sensation that something is moving around in the knee. There may also be an audible sound associated with the popping, which in medical terms is called crepitus. This can also cause what we call mechanical catching or locking, which may make the knee feel like it is stuck in an extended or flexed position, and you have to move it in certain ways to get out of that. This knee popping sensation or sound or could be a very simple issue or it could be a sign that more serious damage is going on in the knee, so determining what is causing it is very important. So, the knees may pop and get in a certain position….
Read More About Knee PoppingKnee Swelling
Swelling of the knee, also known as water on the knee, is a condition in which fluid collects around the knee joint. Swelling can occur for a variety of reasons and affect patients of any age. Some swelling can be treated with over-the-counter medicines, but persistent and continuous swelling might result in tissue damage, bone softening, and cartilage deterioration. Over-the-counter medicines will assist relieve pain for individuals with a history of osteoarthritis and swelling following physical activity, such as exercise or running. During and after activity, the patient may apply compression sleeves to reduce the inflammation. Ice is another method…
Read More About Knee SwellingKnee Twitching & Spasms
Knee twitching and or spasms are common occurrences that can be caused by a variety of factors. In most cases, it is not a cause for concern and does not require treatment. However, in some instances, knee twitching may be a sign of a more serious condition. Knee twitching is often accompanied by a feeling of pins and needles or tingling in the knee. It may also be accompanied by a burning sensation. The twitching usually occurs intermittently and lasts for a few seconds. There are a number of things that can cause knee twitching. Some of the most common…
Read More About Knee Twitching & SpasmsOutside Knee Pain
What causes outside knee pain? How do you treat it? Let us go over all of this and also review how one patient avoided a huge surgery. What is On the Outside of the Knee? You have a couple of key structures here (1). They include the: Lateral meniscus, Lateral joint compartment, Popliteus tendon, Iliotibial band, Lateral collateral ligament , and anterolateral ligament, and Fibula. The meniscus is a figure-8 shaped fibrous structure (shown here from above) that is a shock absorber for the knee joint. It has an outside part (lateral meniscus) that cushions the joint. The meniscus can become torn or degenerated. If you are young…
Read More About Outside Knee PainPain Behind Knee
First off, this is where the hamstrings and calf muscles attach. They have tendons here that are inserted into the bone. So if there’s a problem in the muscle or the tendon, you’re going to feel it right here. This is also where deep muscles like the popliteus and plantaris live. So, if these have issues, you’re going to feel it in the back of the knee. In addition, the tibial nerve is back here. So if there’s an issue with a nerve in your back or a nerve locally, behind the knee, you’re going to feel it here. And the meniscus or the joint spacer lives back here. And the meniscus or the joint spacer lives back here. So a tear in the meniscus could cause pain…
Read More About Pain Behind KneeReduced Range of Motion in Knees
A knee can feel stiff if there is some swelling in or around the joint or muscle tightness can caused restricted motion This can occur from a problem in the knee joint, such as inflammation, arthritis, or infection, or an injury. The distance and direction that a joint may move are referred to as its range of motion. Various joints in the human body have specific normal ranges set by doctors and therpists. One study, for example, found that a normal knee should be able to bend to between 133 and 153 degrees. A typical knee should also be able to extend fully straight. Limitation of motion occurs when a person range of motion in any limb is reduced below the normal range….
Read More About Reduced Range of Motion in KneesTightness in Knee
What could tightness in your knee mean? When fluid builds up inside the knee as a result of an injury, overuse, or medical problem, the knees become swollen and tight. Swelling might be mild, so you may not always notice it unless it is serious damage. You may feel this as stiffness in the knee since swelling may not be visible. Swelling restricts movement since there is less room in the knee. Fluid buildup can be caused by irritation, internal bleeding, and injuries to the knee. Arthritis, gout, tumors, and baker cysts are all causes of swelling. Pain and swelling are the responses of your body to damage. Together they can lead to stiffness in your knee…
Read More About Tightness in KneeWeak in Knees
Weakness in the knee can be a symptom of many different knee conditions. Some of the most common causes of weakness in the knee include ligament tears, meniscus tears, and arthritis. Another important but often overlooked cause of knee weakness is irritation or injury of the nerves in the low back. If you are experiencing any type of weakness in your knee for long durations of time (3 weeks), it is important to see a doctor to determine the cause. Some of the most common symptoms of knee weakness include difficulty standing up from a seated position, difficulty walking, climbing or descending stairs…
Read More About Weak in KneesDid you know that MRI or X-ray findings consistent with arthritis in knee are common in anyone over the age of 40 EVEN in individuals with zero knee pain or asymptomatic knees (1-3)? This means there are other causes of knee pain other than just arthritis. This highlights the importance of a detailed examination and getting a thorough history of the issues to help determine if the pain is from the knee arthritis OR the knee arthritis is asymptomatic, and the pain is coming from something other than the cartilage loss!
Common complaints about most knee conditions (including arthritis in knee) are:
Pain Increasing Gradually During Activities
If you have a loss of cartilage and underlying bone is exposed, additional stress on the knee leads to bone bruising, which can be seen on an MRI as “bone marrow edema.” Research has shown a high association with arthritis pain when paired with a bone bruise.
Swelling
Increased fluid in the knee is not a universal sign of arthritis as many things can cause fluid to build up in the knee and it’s important to investigate further to determine the source! Some examples are:
- Meniscus tears – Diagnostic ultrasound can identify meniscal tears as can MRIs. In the absence of other conditions these may be a cause of fuid buildup.
- Ligament injuries such as ACL or PCL tears – Fluid in the joint is not synovial fluid with ligament tears but bleeding in the joint which can also be seen in fractures.
- Arthritis – There are many different autoimmune diseases that increase joint fluid, as well as osteoarthritis in which cartilage loss causes thinning of the synovial fluid and it expands creating excessive fluid in the joint.
- Joint infections can cause excessive swelling.
For an accurate diagnosis of what kind of fluid is building up, aspirating the fluid and sending it to the lab for more detailed analysis is needed!
Crackling Sound
With knee arthritis, additional bone exists in the form of bone spurs. These can rub on other bones or
Crackling can happen in a 100% normal knee where some air or fluid release occurs or a ligament or tendon is snapping over a bony prominence.
One potential issue that can cause the crackling sound is lax ligaments surrounding the knee such as the medial (inside) or lateral (outside) ligaments.
Check out what a live diagnostic ultrasound of laxity in the MCL (Medial collateral ligament) looks like below. This laxity allows additional movement in the joint which can lead to “crackling or popping” sounds in the joint https://www.instagram.com/p/BetLa9QhpuD/?utm_source=ig_web_copy_link
Buckling And Locking
With knee arthritis, bone bruises or bone spurs can cause immediate and intense shots of pain which can inhibit all the muscles around the joint. This can manifest itself in the knee giving out or locking in place.
BUT ligament injuries such as an ACL tear can also cause incidences of buckling as the ligament is not functioning enough to support the knee.
Meniscus tears or loose bodies in the joints can get stuck between the bones and create locking issues as well!
Limited Range Of Motion
Bone spurs grow all around the joint with arthritis which can impede the joint from a full range of motion.
So, as you can see, there are a lot of overlap symptoms between knee arthritis and other conditions in the knee, which highlights the importance of a highly trained medical provider investing the time to discuss your issues, examine your knee, and ordering an appropriate test to best determine the cause of your unique knee pain. All too often a patient goes to a doctor and in 5 mins the doctor tells the patient what is wrong without ever talking to the patient or examining them – just going off an MRI or x-ray.
Common Causes of Knee Arthritis
Developing arthritis in knee or any other joint in your body is, unfortunately, inevitable. If you live long enough, one of your joints will likely break down and develop arthritis. Some individuals develop arthritis sooner than others. There are many risk factors that determine whether this happens to you! Some you can control while others are predetermined. Let’s dig in….
Heredity
You cannot control what genes you are born with and some genes place you at risk for developing arthritis prematurely.
Aging
Risk for multiple types of arthritis increase with age. Those include:
- Osteoarthritis
- Rheumatoid Arthritis
- Gout
Obesity
The relationship between excess weight and OA is well established. In fact, obesity appears to be the top modifiable factor that influences OA risk, with one study reporting that individuals whose body mass index (BMI) was higher than 30 kg/m2 had a nearly 7-fold increased risk of developing knee OA. (5)
Repetitive Stress Injuries
Small repetitive traumas over time increase the cumulative damage in the knee and eventually accumulate irreversible damage. Have you ever seen the knees of NFL players, especially a lineman after years of weighing >300lbs and repetitive stress (6)?
Past Surgeries
Especially ACL reconstruction and meniscectomy, develop post-traumatic knee arthritis as a complication of both the trauma that resulted in the injury as well as trauma from the surgery.
New research shows ACL reconstruction surgery itself leads to a greater risk of developing knee arthritis! To read more go here: https://regenexx.com/blog/acl-reconstruction-surgery-is-a-second-hit-to-the-cartilage-time-to-rethink-orthopedics/#gref
Common Treatments for Knee Arthritis
Knee arthritis treatment, like most other orthopedic treatment, ranges from the least invasive to the most invasive treatments. They begin with something as simple such as medications and physical therapy to the most invasive such as total knee replacements….and many treatments in between.
Medication
- Supplementation https://centenoschultz.com/controlling-knee-arthritis-pain-with-a-proper-omega-6-to-omega-3-ratio/
Therapies / Modalities
Physical Therapy
One of the main treatments to prevent arthritis with the goal to correct the underlying bio-mechanics by strengthening the knee and the muscles up and down the kinetic chain. Physical therapy has been proven a useful toll with the right therapist to help both pain and function!
Simple Injections
If physical therapy is not helping, most physicians or orthopedic physicians resort to knee injections.
Cortico-Steroid Injections
Steroids have been a mainstay in the treatment of arthritic conditions. But there are downsides and risks to these injections:
- Systemic effects such as increasing cortisol and elevating blood sugars
- Risk of creating avascular necrosis
- Risk of degenerating the joint more and advancing arthritis (which is the wrong direction if already have arthritis!)
Hyaluronic Acid (HA) Injection
This substance is naturally found in the synovium and synovial fluid so injection provide nutrition to the joint and lubrication and can give lasting improvement 6 to 12 months.
Other Alternative Therapies
Alternative therapies include acupuncture, dry needling, cupping, Graston, and blood flow restriction therapy.
Surgical Procedures
There are multiple surgical procedures that are performed for arthritis in the knee.
Knee arthroscopic procedure “clean out”
Surgeons take you to the surgical suite, place a camera inside the knee and shave down loose bits of cartilage floating around as well as trim meniscus. BUT long term evidence and research have proven that this method does more harm than good (7).
Supported by landmark articles by Mousley et al. and Kirkley et al., it may seem that the role of arthroscopic surgery in the degenerative knee is no longer justified. They found no difference in outcomes in Mousley ‘s single-blinded randomized controlled trial in 2002 comparing arthroscopic surgery versus sham surgery and again no difference in outcomes in Kirkley’s randomized controlled trial in 2008 comparing arthroscopic surgery versus optimized medical and physical therapy. This makes total sense given the fact they are shaving away the cartilage you have left that we know won’t grow back…….who thought that was a good idea, to begin with?!
Total Joint Replacement
To learn more about TKR (Total Knee Replacement) go here:
https://regenexx.com/blog/is-this-the-truth-about-knee-replacement-surgery/#gref
Using Support / Brace
Bracing can help support the joint when ligaments around and in the joint aren’t up to the task and offload the arthritis region of the joint assuming only one of the 3 compartments showing arthritic changes.
Cupping Therapy
Cupping therapy is an ancient method of treatment that has been used in the treatment of a broad range of conditions. This therapy has its roots in various traditional medicine systems, including traditional Chinese medicine (TCM) and Middle Eastern folk medicine. This therapeutic technique involves creating a vacuum or negative pressure inside specialized cups, typically made of glass, bamboo, or silicone. The negative pressure can be achieved through different methods, such as the application of heat using flames, electrical suction devices, or manual suction.
Read More About Cupping TherapyKnee Arthroscopy Surgery
Knee arthroscopy surgery is a very common procedure performed by orthopedic surgeons in an attempt to treat knee pain. Knee arthroscopic surgery is typically performed in an outpatient surgical facility where a small camera is inserted into the knee joint, which allows the surgeon an inside view of one’s knee to operate. It is used both to diagnose and treat a wide variety of knee problems. Utilizing arthroscopic surgery the surgeon can trim any damaged ligaments which are called knee ligament surgery. Alternatively, if ‘damaged’ meniscus is detected, it also is trimmed and or removed, which is called meniscus knee surgery.
Read More About Knee Arthroscopy SurgeryKnee Replacement
Your knee pain initially was intermittent and mild. Unfortunately, It is now constant and debilitating. Your doctor recommends knee replacement surgery. What is the knee composed of? What are the most common knee injuries? What is knee replacement surgery? What are the different types of knee replacements? What is knee replacement surgery success? What are the 12 most common complications associated with knee replacement surgery? What regenerative treatment options exist? How to avoid knee replacement? Let’s dig in.
Read More About Knee ReplacementNSAIDs
The other day I was evaluating a patient and reviewing the treatment options for their spine condition. After discussing prior treatments, we got to the topic of medications taken for pain relief. She explained that she mainly utilized anti-inflammatory (NSAID) medications and then she told me to hold much she takes and has been for many years…..she takes close to 2 grams (2000 milligrams) on a daily basis which equated to about 9-10 capsules of medication per day. I was shocked, considering she was pre-diabetic and with high blood pressure plus the kicker of it is that her PCP (primary care physician) is ok with this…
Read More About NSAIDsPRP for Osteoarthritis
To discuss PRP for Osteoarthritis we need to define Osteoarthritis. Arthritis is a general term for painful conditions that involve one or more body joints such as the knee and hip. Most types of arthritis involve pain, swelling, and stiffness. There are more than 100 types of arthritis. Osteoarthritis is the most common form of arthritis affecting more than 30 million adults in the united states (1). It involves the breakdown of the protective cartilage. In 2013 osteoarthritis was the second most expensive condition treated in US hospitals accounting for more than $165 billion in hospital costs (2). Other types of arthritis include rheumatoid arthritis, juvenile arthritis, and gout.
Read More About PRP for OsteoarthritisPRP Injections
PRP is short for platelet-rich plasma, and it is autologous blood with concentrations of platelets above baseline values. The potential benefit of platelet-rich plasma has received considerable interest due to the appeal of a simple, safe, and minimally invasive method of applying growth factors. PRP treatments are a form of regenerative medicine that utilizes the blood healing factors to help the body repair itself by means of injecting PRP into the damaged tissue. In regenerative orthopedics, it is typically used for the treatment of muscle strains, tears, ligament and tendon tears, minor arthritis, and joint instability. There have been more than 30 randomized controlled trials of PRP…
Read More About PRP InjectionsPRP Knee Injections
PRP stands for Platelet-Rich Plasma. Platelets are blood cells that prevent bleeding. They contain important growth factors that aid in healing. Plasma is the light yellow liquid portion of our blood. So PRP is simply a concentration of a patient’s own platelets that are suspended in plasma and are used to accelerate healing. PRP is NOT stem cell therapy. Regrettably, blood contains few circulating stem cells. Rich sources of stem cells are bone marrow and fat. PRP is rich in growth factors. There are many different types of growth factors with different properties. VEGF is a very important one as it can increase the blood flow to an area.
Read More About PRP Knee InjectionsAlternative Treatments To Surgery For Knee Arthritis
All of the physicians at Centeno Schultz Clinic have been researching and continue to search for better alternatives to total joint replacement to give our patients a less invasive alternative that accomplishes the goal of getting patients back doing what they want to do with little downtime, less risk of complications and that last as long a replacement!
Research has shown that using your own Bone Marrow Concentrate (which contains stem cells) can be just as effective with less risk when directly compared to total joint replacement.
RESULTS:
- Anesthesia related to the TKA side was longer than for the cell therapy group. Medical and surgical complications were more frequent after TKA.
- A higher number of thrombophlebitis was observed on the side with TKA (15%) versus none on the side with cell therapy (0%).
- At follow-up (average of 12 years, range 8 to 16 years), six (out of 30) TKA knees needed subsequent surgery versus only one with cell therapy.
- The Knee Score had improved and remained similar in the TKA and cell therapy groups (respectively 80.3 points ± 11 versus 78.3 ± 23);
- 21 patients preferred the knee with cell therapy and 9 preferred the knee with TKA.
- Knees with cell therapy had improvement on cartilage and bone marrow lesions observed at the site of bone marrow subchondral injection.
Examining And Diagnosing Knee Arthritis
If you made it this far, congrats! We have been treating knee arthritis with advanced regenerative interventional orthopedic technology since the early 2000s. We were the first physicians in the country to use the patient’s own Bone Marrow Concentrate containing stem cells to treat various orthopedic conditions. With decades of experience to lean on, we know how to get our patients the best outcomes possible: it’s all about the details! With our examinations, we take 60 mins of physician-patient face-to-face time to get a detailed history of the knee pain, a thorough examination of how your knee uniquely works, and utilize diagnostic ultrasound to evaluate the soft tissue surrounding the joint. We also take a very thorough look at your imaging, not just read the report.
Based on all of the above we come up with a comprehensive evaluation, and along with all our data and current research, we determine a Candidacy Rating of Good, Fair, or Poor. Candidacy is our expert opinion on the likelihood of success, and which therapy will yield the best long-term outcome to accomplish your goal. Many times after a full examination we do not recommend any of our treatments and recommend a surgical consultation. We will be honest with you in our evaluation once we have all the evidence!
What You Can Do To Prevent Knee Arthritis
There are always things you can do to be proactive in preventing knee arthritis or stopping or slowing the progression of OA!
- Regular exercise routine – Keeping a sedentary life is the worst thing you can do. Try your best to continue to move and live by the motto: “motion is lotion” because once you stop moving then things can break down more rapidly.
- Nutrition – Watching what you eat and making good nutrition decisions on what you put into your body can play a huge role in in your whole body inflammation. This type of inflammation can affect every aspect of your life from sleep habits, bowel health, joint health and mood. Check out Dr. Pitts’ blog on nutrition https://centenoschultz.com/dr-pitts-top-7-best-and-worst-foods-for-good-health/ or read his nutrition book https://regenexx.com/resources/ebooks-and-reports/nutrition-2-0/#gref
Get Yourself Checked To Get A Better Diagnosis
If you are considering an alternative to knee replacement and would like to get a detailed evaluation, contact our office! We do both in-patient examinations and telehealth consultation to help give you an accurate diagnosis and a candidacy rating on how effective, or whether it’s even indicated, a Regenexx Procedure for knees would likely be for you!
Doctors That Assist With Knee Osteoarthritis

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics. He is board-certified in physical medicine and rehabilitation with a subspecialty of pain medicine through The American Board of Physical Medicine and Rehabilitation. Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who…
Read more
John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreAdditional Resources on Knee Arthritis
Free Download: The Knee Owner’s Manual

This e-book by Dr. Chris Centeno examines the knee and its role in the human musculoskeletal system and the body as a whole. The Knee Owner’s Manual provides a series of tests and clearly defined exercises that you can perform on your own to assess and monitor your own knee health. It will allow you to look for trouble spots where your own body may be having difficulty with stability, articulation, symmetry, and neuromuscular function. You’ll be able to see how these deficits in other regions of the body relate to the knee.
The Knee Owner’s Manual also discusses how Regenexx is pioneering the development of interventional orthopedics, a new branch of medicine that employs regenerative biologic therapies such as adult bone marrow concentrate and platelet-rich plasma to help repair and strengthen damaged tissues in other areas of the body.
This is contrasted with invasive knee surgeries, which often remove important tissues or replace the entire knee itself when it becomes damaged. With hyperlinks to more detailed information, related studies, and commentary, this book condenses a vast amount of data, images, and resources into an enjoyable and informative read. This is the first edition of The Knee Owner’s Manual, a companion book to Orthopedics 2.0.
-
7 Most Common Symptoms of a Loose Knee Replacement
Walking became impossible. Each step was associated with severe pain. Knee replacement seemed like a good solution. Unfortunately, months after the surgery problems exist. Your doctor thinks you have a loose knee replacement. What is a knee replacement? What causes a knee replacement to become loose? What are the 7 most common symptoms of a…
-
14 Disadvantages of Knee Replacement Surgery
Every step is a reminder of your knee pain. Physical therapy and steroid injections did not help. Your doctor is referring you for surgery. What is knee replacement surgery? What are the disadvantages of knee replacement surgery? What is the success rate of knee replacement surgery? What are the alternatives to knee replacement surgery? Let’s…
-
Matt Chan’s Journey with CrossFit Injuries and Regenexx Treatments
Matt Chan, a Denver Firefighter, and National CrossFit Champion undergoes treatment at the Centeno-Schultz Clinic. Dr. Schultz discusses how athletes and others can successfully use stem cells to treat knee and back injuries.
References:
- Beattie KA, Boulos P, Pui M, O’Neill J, Inglis D, Webber CE, Adachi JD. Abnormalities identified in the knees of asymptomatic volunteers using peripheral magnetic resonance imaging. Osteoarthritis Cartilage. 2005 Mar;13(3):181-6. doi: 10.1016/j.joca.2004.11.001. PMID: 15727883.
- Pappas GP, Vogelsong MA, Staroswiecki E, Gold GE, Safran MR. Magnetic Resonance Imaging of Asymptomatic Knees in Collegiate Basketball Players: The Effect of One Season of Play. Clin J Sport Med. 2016;26(6):483-489. doi:10.1097/JSM.0000000000000283
- Guymer E, Baranyay F, Wluka AE, Hanna F, Bell RJ, Davis SR, Wang Y, Cicuttini FM. A study of the prevalence and associations of subchondral bone marrow lesions in the knees of healthy, middle-aged women. Osteoarthritis Cartilage. 2007 Dec;15(12):1437-42. doi: 10.1016/j.joca.2007.04.010. Epub 2007 Jun 7. PMID: 17560134.
- Culvenor AG, Øiestad BE, Hart HF, Stefanik JJ, Guermazi A, Crossley KM. Prevalence of knee osteoarthritis features on magnetic resonance imaging in asymptomatic uninjured adults: a systematic review and meta-analysis. Br J Sports Med. 2019;53(20):1268-1278. doi:10.1136/bjsports-2018-099257.
- King LK, March L, Anandacoomarasamy A. Obesity & osteoarthritis. Indian J Med Res. 2013; 138(2): 185–193.
- Davies MAM, Kerr ZY, DeFreese JD, Arden NK, Marshall SW, Guskiewicz KM, Padua DA, Pietrosimone B. Prevalence of and Risk Factors for Total Hip and Knee Replacement in Retired National Football League Athletes. Am J Sports Med. 2019 Oct;47(12):2863-2870. doi: 10.1177/0363546519870804. Epub 2019 Sep 9. PMID: 31498654.
- Law GW, Lee JK, Soong J, Lim JWS, Zhang KT, Tan AHC. Arthroscopic debridement of the degenerative knee – Is there still a role?. Asia Pac J Sports Med Arthrosc Rehabil Technol. 2018;15:23-28. Published 2018 Dec 8. doi:10.1016/j.asmart.2018.11.003