Leg Feels Disconnected
Get Help With Leg Feels DisconnectedIt’s always fascinating to hear how patients describe what’s bothering them. When one patient with the instability of her SI joint said her “leg feels disconnected,” this one stuck with us. Why? What would cause your leg to feel disconnected? Because this is an acutely accurate description of what it feels like, we thought we’d dissect this description a bit today.
What Is the SI Joint?
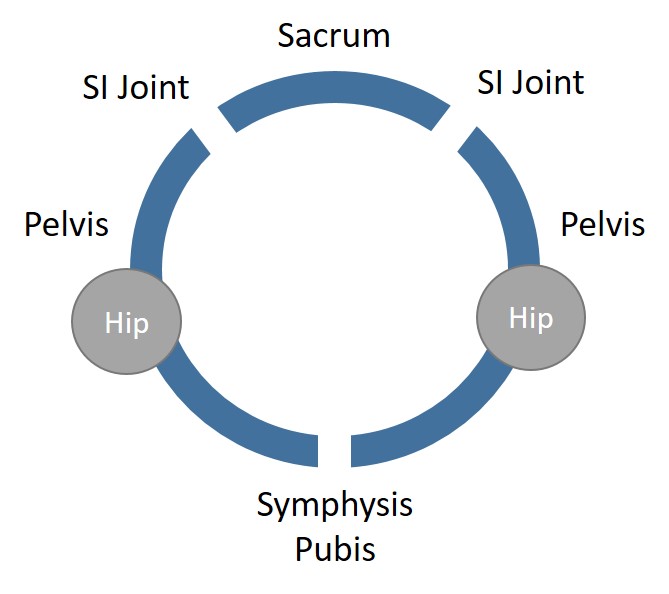
The sacroiliac (SI) joint is located where the sacrum (aka tail bone) and the back of the hip (at the largest part of the hip bone called the ilium) meet. There is a three-joint system located here known as the pelvic ring, and the SI joints (there are two of them as the image to the left shows) are part of this ring. The two SI joints live in the back of the pelvic ring while a single joint called the symphysis pubis lives at the front. The three joints work together to manage the forces that move up the leg and into the spine. Strong ligaments surround and support the joints.
What Can Make Your Leg Feel Disconnected
So what exactly causes the leg to feel disconnected? The hip joint is the connection point between the leg and the rest of the body. The femur in the leg and the acetabulum in the pelvis create the hip joint. So if the left SI joint, for example, in the back and the symphysis pubis joint in the front become unstable due to loose supporting ligaments, then the left leg, which is connected between the two joints, is likely to also feel a bit disconnected. Likewise, if the right SI joint were unstable, then the right leg might feel disconnected.
Degenerative Scoliosis
Degenerative Scoliosis, also known as Adult-onset Scoliosis, is a medical condition that involves a side bending in the spine. The bending can be mild, moderate, or severe with side-bending to either the right or the left. The term degenerative means generalized wear and tear and is common as we get older. Degenerative scoliosis is the curvature of the spine that occurs as a result of degeneration of the discs, small joints, and building blocks. The Degenerative Scoliosis curve is often located in the low back and forms a ‘C” shape. There is a convex and a concave side. The convex side is the open side where it curves outward.
Read More About Degenerative ScoliosisEhlers-Danlos Syndrome (EDS)
Disorders that affect and weaken the connective tissues such as tendons and ligaments. It is a hereditary disorder which means you are born with it. EDS has many different signs and symptoms which can vary significantly depending upon the type of EDS and its severity. It most commonly affects the skin, joints, and blood vessels. Joints are typically hypermobile with excessive joint range of motion because of a defect in collagen formation. In most cases Ehlers-Danlos syndrome is inherited. That is to say that you are born with it. The two main ways EDS is inherited are: autosomal dominant inheritance and autosomal recessive inheritance…
Read More About Ehlers-Danlos Syndrome (EDS)Failed Back Surgery Syndrome
Failed Back Surgery Syndrome also called failed back is a clinical condition in which patients who have undergone low back surgery continue to have pain and dysfunction. Said another way the surgery that was intended to reduce pain and increase function FAILED. That is right, the surgery failed. You had the surgery, struggled with the pain postoperatively, diligently participated in physical therapy and yet the pain and limitation are still there. Unfortunately, this occurs frequently. Estimates range from 20-40% of patients who undergo low back surgery will develop Failed Back Surgery Syndrome. Pain is the most common symptom of Failed Back Surgery Syndrome…
Read More About Failed Back Surgery SyndromePinched Nerves in the Back
We talk a lot about leg pain stemming from a pinched or irritated nerve in the lower back. And, indeed, that’s what our physicians are traditionally taught in medical school—a pinched nerve in the lumbar spine typically presents as a symptom in the leg. However, what if you have some butt pain but no pain or other symptoms in the leg? Does this mean it couldn’t be a pinched nerve? Not so fast. Turns out a pinched low back nerve doesn’t always have to be accompanied by leg symptoms. Let’s start by taking a look at how the back is structured.
Read More About Pinched Nerves in the BackSciatica
Disc herniation, disc protrusion, overgrowth of the facet joint, and thickening of the ligaments can result in nerve root compression or irritation, causing symptoms of sciatic compression. Some causes of sciatic compression can be interrelated with the following conditions: Degenerative disc disease, Spinal stenosis, damage or injuries to the discs, spondylolisthesis, piriformis syndrome, osteoarthritis. The symptoms of sciatica include pain in the lower back, buttock, and down your leg, numbness and weakness in low back, buttock, leg, and/or feet, pain increase with movement, “Pins and needles” feeling in your legs, toes, or feet., loss of bowel control, and incontinence. Sciatica can be treated…
Read More About SciaticaSpondylolisthesis
Spondylolisthesis means that one vertebra is slipping forward or backwards on another. This causes the hole where the nerve exits (foramen) to get smaller (also called foraminal stenosis). It also causes more wear and tear on the facet joint which can lead to arthritis or what’s called “facet hypertrophy”. spondylolisthesis recovery The amount of slippage is graded 1-4, with grade 1 meaning that the one vertebra has slipped up to 25% on the other vertebra. Grade 2 means that one bone has slipped from 25-50% with higher grades indicating more slippage. The vast majority of patients are grade 1 to 2.
Read More About SpondylolisthesisThoracic Degenerative Disc Disease
Degenerative disc disease is a clinical condition that refers to the gradual deterioration of the discs located in the thoracic spine and the associated symptoms. Pain, weakness, muscle spasms, and restriction in range of motion are common. Degenerative disc disease can occur at each level of the spine: cervical, thoracic, and lumbar. Studies have demonstrated that degenerative disc disease in the thoracic spine most commonly occurs in the third to fourth decades (1) and occurs most frequently in the lower thoracic segments from T7-T12. Thoracic degenerative disc…
Read More About Thoracic Degenerative Disc DiseaseThoracic Spondylosis
The thoracic spine, also known as the mid back, is that portion of the spine that is below the cervical spine (neck) and above the lumbar spine (low back). Thoracic spondylosis is a degenerative condition of the thoracic spine. The thoracic spine, also known as the mid back, is composed of many important different structures that work together to provide stability and movement. Thoracic spondylosis is a degenerative condition affecting the middle region of the spine, known as the thoracic spine. The major causes include: aging, genetics, poor posture, repetitive strain, and more. Symptoms can be mild, moderate, or severe…
Read More About Thoracic SpondylosisHow This Patient’s “Disconnected” Leg Was Fixed
Despite “leg feels disconnected” sensation, we were able to successfully treat this patient’s “disconnected” leg feeling by addressing the SI joint. We did this by injecting growth factors derived from her platelets as well as a proliferant. This helped the ligaments tighten up. For the patient, she had been wearing a stabilizing SI belt all the time. After her treatment, she no longer had to wear the belt to perform normal activities. She is a skier and reported that this is the only time she now feels the need to wear her SI belt.
What About Steroids for a Painful SI Joint?
We say just don’t do it! While you may enjoy some temporary relief with an SI joint steroid injection, it’s only addressing the symptom, not the real problem, which is the instability due to the loose ligaments. Not to mention, the introduction of steroids is only creating more problems that you will no doubt have to deal with down the road. We’ve created a page for SI Joint Syndrome you can read.
Treating the Symphysis Pubis Is Also Important
Treating the symphysis pubis joint at the front of the pelvic ring is just as important as treating the SI joint, yet many physicians who offer prolotherapy (or ligament injections) don’t know to treat that area. This particular patient did not want to treat her symphysis pubis instability a few years ago when we treated her SI joint, but as running is the next challenge she’d like to conquer, she is now ready to take that step to try to get even better control of her pelvic-ring instability.
Every good doctor knows that if you let the patient talk and just listen, he or she will tell you exactly what’s wrong. Sometimes, such as in the case of this disconnected leg, what’s wrong is much more accurate than the patient even realizes!