Thoracic spine surgery is a major surgery aimed at treating injuries in the thoracic spine. Because of the complex anatomy and close proximity to the heart and lungs, there are significant surgical risks and complications. Surgery on the thoracic spine can take hours and may require deflating the lung in order to gain access to the thoracic injury. Recovery can be lengthy depending upon the specific thoracic spine surgery performed.
Thoracic Spine Surgeries
There are several different types of thoracic spine surgery. The specific thoracic spine performed depends upon the underlying thoracic injury and a patient’s symptoms. For example, a thoracic disc herniation with no significant narrowing of the central canal may be a good candidate for posterior thoracic discectomy. Conversely, a patient who has sustained significant trauma to a thoracic disc may need a posterior thoracic fusion. The goal of thoracic spine surgery is to trim or cut out damaged tissues in the thoracic spine that is giving rise to a patient’s symptoms so as to restore the patient back to their clinical baseline.
Common Thoracic Spine Conditions That Result in Surgery

There are many different thoracic spine conditions that require surgery. The most common include:
- Degenerative Disc Disease: generalized wear and tear on the disc.
- Herniated Disc: Extrusion of the inner portion of the disc through the damaged sidewall into the spinal canal.
- Spinal Stenosis: narrowing of the spinal canal due to disc protrusion, disc herniation, facet joint overgrowth, and ligament thickening.
- Spondylolisthesis: slippage of one or more of the bones in the spine with injury to the disc, and facet joints and in many cases causes spinal canal stenosis.
- Osteoporosis: a bone disease characterized by decreased bone strength. Patients are a risk for fractures.
- Scoliosis: an abnormal sideways curve of the spine. The most common causes of scoliosis include congenital, neuromuscular, or degenerative conditions.
- Kyphosis: an abnormal forward curve in the spine.
- Compression Fractures: an injury of the vertebral body (boney building blocks in the spine) that makes them susceptible to collapse.
Annular Tear
To understand annular tears, let us first review the anatomy of the spine. The lumbar spine is comprised of 5 boney building blocks called vertebral bodies. Sandwiched between the vertebral bodies are the lumbar discs. Each disc is comprised of an outer fibrous ring, the annulus fibrosis that surrounds the inner gelatinous center, which is called the nucleus. The disc absorbs the forces of daily living. The annulus has multiple layers of collagen that provide important support. The annulus is similar to the sidewall of a tire which provides important stability for the tire. Through trauma or degeneration, the outer annular fibers can become injured and or weakened.
Read More About Annular TearBulging Disc In Thoracic Spine
A bulging disc in the thoracic spine is a serious medical condition that occurs when the outer layer of the disc weakens, causing it to bulge outward and put pressure on nerves and the spinal cord. The disc has two components, a soft center and a thick outer layer, and weakening or tears in the outer layer can lead to a bulge. Symptoms include pain, numbness, and weakness in the affected area. The thoracic spine is that portion of the spine that resides below the neck and above the low back. It is commonly referred to as the mid-back. A bulging…
Read More About Bulging Disc In Thoracic SpineDegenerative Scoliosis
Degenerative Scoliosis, also known as Adult-onset Scoliosis, is a medical condition that involves a side bending in the spine. The bending can be mild, moderate, or severe with side-bending to either the right or the left. The term degenerative means generalized wear and tear and is common as we get older. Degenerative scoliosis is the curvature of the spine that occurs as a result of degeneration of the discs, small joints, and building blocks. The Degenerative Scoliosis curve is often located in the low back and forms a ‘C” shape. There is a convex and a concave side. The convex side is the open side where it curves outward.
Read More About Degenerative ScoliosisFacet Joint Syndrome
Injury or inflammation of the cervical facet can led to neck, shoulder and headache pain – called “cervical facet syndrome.” Cervical facet syndrome largely involves a joint in the posterior aspect of the cervical spine. It functions to provide stability and guide motion. cervical facet joint injection for cervical facet syndrome Cervical facet pain is common in patients who have sustained a whiplash injury, trauma to the neck or undergone cervical fusion. Physical examination is typically significant for restriction in range of motion along with pain. Each joint has a distinct referral pattern illustrated below. The Centeno-Schultz Clinic are experts at diagnosing and treating cervical facet dysfunction. Injury to the joint is not commonly detected by conventional radiographic studies.
Read More About Facet Joint SyndromeFailed Back Surgery Syndrome
Failed Back Surgery Syndrome also called failed back is a clinical condition in which patients who have undergone low back surgery continue to have pain and dysfunction. Said another way the surgery that was intended to reduce pain and increase function FAILED. That is right, the surgery failed. You had the surgery, struggled with the pain postoperatively, diligently participated in physical therapy and yet the pain and limitation are still there. Unfortunately, this occurs frequently. Estimates range from 20-40% of patients who undergo low back surgery will develop Failed Back Surgery Syndrome. Pain is the most common symptom of Failed Back Surgery Syndrome…
Read More About Failed Back Surgery SyndromeHerniated Thoracic Disc
A herniated thoracic disc is especially difficult because there are not as many treatments available as there are for disc herniations in other areas of the spine. To understand Thoracic Disc Herniations, though, we first need to cover thoracic spine anatomy and function. With disc herniation, the annulus fibrosus get small tears throughout the annulus. An annulus is a bunch of concentric fibers, so, as the fibers get damaged and cut, the pressure that is built up within the nucleus pushes the now weakened annulus outward, creating a bulge or herniation. The disc begins to weaken via mild degeneration/tearing of the annular fibers…
Read More About Herniated Thoracic DiscPinched Nerves in the Back
We talk a lot about leg pain stemming from a pinched or irritated nerve in the lower back. And, indeed, that’s what our physicians are traditionally taught in medical school—a pinched nerve in the lumbar spine typically presents as a symptom in the leg. However, what if you have some butt pain but no pain or other symptoms in the leg? Does this mean it couldn’t be a pinched nerve? Not so fast. Turns out a pinched low back nerve doesn’t always have to be accompanied by leg symptoms. Let’s start by taking a look at how the back is structured.
Read More About Pinched Nerves in the BackSpinal Instability
Spinal instability is a condition that occurs when the spinal column is not able to maintain its normal alignment and function under normal loads. It can be caused by various factors such as trauma, degenerative changes, infections, tumors, or congenital abnormalities. In a stable spine, the bones, discs, ligaments, and muscles work together to support and protect the spinal cord and nerve roots. However, in an unstable spine, the structures that support the spine may be damaged or weakened. This can lead to abnormal movement and excessive stress on the spinal cord and nerves. In most cases, bone and joint problems…
Read More About Spinal InstabilitySpinal Stenosis
Spinal stenosis is the narrowing of the central spinal canal and is a cause of significant pain and disability. Common causes of spinal stenosis include disc protrusion, facet overgrowth and ligamentum flavum thickening. Surgery is often chosen when conservative therapies fail despite the lack of convincing evidence that it is a superior treatment option. Are there alternatives to back surgery for spinal stenosis? Yes. Regenexx DDD utilizes precise platelet injections into the facets, muscles, and ligaments to treat the lumbar stenosis, treating all of the components of the issue, which is crucial. Spinal stenosis is often an age-related condition attributed…
Read More About Spinal StenosisSpondylolisthesis
Spondylolisthesis means that one vertebra is slipping forward or backwards on another. This causes the hole where the nerve exits (foramen) to get smaller (also called foraminal stenosis). It also causes more wear and tear on the facet joint which can lead to arthritis or what’s called “facet hypertrophy”. spondylolisthesis recovery The amount of slippage is graded 1-4, with grade 1 meaning that the one vertebra has slipped up to 25% on the other vertebra. Grade 2 means that one bone has slipped from 25-50% with higher grades indicating more slippage. The vast majority of patients are grade 1 to 2.
Read More About SpondylolisthesisThoracic Compression Fracture
A compression fracture is a type of bone fracture that typically occurs in the vertebrae of the spine. It occurs when one or more of the vertebrae become compressed or crushed due to excessive forces or pressure. The vertebrae are the bony building blocks that stack one upon another, forming the spine. Compression fractures most commonly occur in the vertebral body, which is the thick, rounded portion of each vertebra. The spine is composed of three sections: cervical, thoracic, and lumbar. The cervical spine is also referred to as the neck, whereas the lumbar is the low back. The thoracic spine is that section of the spine below the neck and above the low back. It is commonly referred to as the mid back. A majority of the compression fractures occur in the thoracic spine.
Read More About Thoracic Compression FractureThoracic Cyst
Cysts are abnormal, closed sacs that contain fluid, gas or semi-fluid material. They can develop in various parts of the body. They can vary in size from very small to large and can be located within organs, tissues or bones. Cysts can be either benign (non-cancerous) or malignant (cancerous). Most cysts are benign. They occur due to a number of different reasons that include obstruction, infection, chronic inflammation, instability or cellular abnormalities. So, thoracic spine cysts are abnormal, closed sacs that occur in the spine below the neck and above the low back.
Read More About Thoracic CystThoracic Degenerative Disc Disease
Degenerative disc disease is a clinical condition that refers to the gradual deterioration of the discs located in the thoracic spine and the associated symptoms. Pain, weakness, muscle spasms, and restriction in range of motion are common. Degenerative disc disease can occur at each level of the spine: cervical, thoracic, and lumbar. Studies have demonstrated that degenerative disc disease in the thoracic spine most commonly occurs in the third to fourth decades (1) and occurs most frequently in the lower thoracic segments from T7-T12. Thoracic degenerative disc…
Read More About Thoracic Degenerative Disc DiseaseThoracic Outlet Syndrome
The thoracic outlet is an area around the collar bone where the nerves that come from your neck meet up with the blood vessels from your heart and together supply the entire upper extremity (shoulder and arm). These blood vessels (subclavian artery and vein) and nerves (brachial plexus) travel from the base of your neck to your armpit (axilla) and are considered the “thoracic outlet”. Now that you know what the thoracic outlet is, what is thoracic outlet syndrome? Simply listening to a patient’s history and completing a physical examination is all that is needed to diagnose TOS. But more involved imaging such as X-rays…
Read More About Thoracic Outlet SyndromeThoracic Spine Arthritis
Osteoarthritis is a common type of arthritis. It is a degenerative joint disease that principally affects the cartilage in your joints. Cartilage is the slippery connective tissue that covers the ends of bones that form joints, and it allows for smooth, effortless movement. Osteoarthritis involves the breakdown of the cartilage with subsequent pain, swelling, and reduced range of motion. The thoracic spine is that section of the spine that is below the neck and above the low back. It is often referred to as the “mid-back.” Thoracic spine arthritis involves the breakdown of the cartilage in joints within the thoracic spine.
Read More About Thoracic Spine ArthritisThoracic Spine Hemangioma
Hemangiomas are benign tumors composed of abnormal blood vessels. They can occur anywhere in the body but most commonly appear on the face, scalp or back. They can also occur in the vertebral bodies in the spine where they are referred to as vertebral hemangiomas. The vertebrae are the boney building blocks that stack one upon another that make up the spine.
Read More About Thoracic Spine HemangiomaThoracic Spondylosis
The thoracic spine, also known as the mid back, is that portion of the spine that is below the cervical spine (neck) and above the lumbar spine (low back). Thoracic spondylosis is a degenerative condition of the thoracic spine. The thoracic spine, also known as the mid back, is composed of many important different structures that work together to provide stability and movement. Thoracic spondylosis is a degenerative condition affecting the middle region of the spine, known as the thoracic spine. The major causes include: aging, genetics, poor posture, repetitive strain, and more. Symptoms can be mild, moderate, or severe…
Read More About Thoracic SpondylosisTorn Discs
The spinal discs are shock absorbers that live at each level between the vertebral bones (1). They have a tough outer annulus part and a soft inner gel part (nucleus pulposis). The outer covering can get damaged which can sometimes be seen on MRI and other times requires additional testing to identify. These tears are called: a torn disc, a disc tear, an annular tear, and when seen on MRI a “High-Intensity Zone” or HIZ. They can cause pain, mostly through ingrown nerves. There are torn disc findings that can be seen on MRI (HIZ) and these can be either asymptomatic (i.e. not painful) or…
Read More About Torn DiscsTypes Of Thoracic Spine Surgeries
There are several different types of thoracic spine surgeries. Which is best? It depends upon the type of thoracic injury, location, severity, and the patient’s symptoms. The 4 major thoracic spine surgeries include:
Posterior Thoracic Spinal Fusion
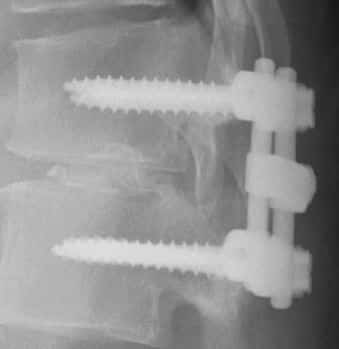
Thoracic spinal fusion is a specific type of surgery involving removing one or more thoracic discs with the insertion of bone grafts or disc spacers. The spine is then stabilized with screws and bolts. The term posterior refers to the surgical approach. Posterior means from the backside of the spine. A posterior thoracic spinal fusion is a major surgery
Risks unique to spinal fusions include:
- Permanently changes the biomechanics of the spine
- Implanted screws, bolts, and rods may crack or break requiring in many cases additional surgeries.
- Risk of adjacent segment disease (ASD) (1). A breakdown of the discs and facet joints above and below the fusion as a result of the increased pressure. To learn more about adjacent segment disease please click on the video below.
Life After Posterior Thoracic Spinal Fusion Surgery
Life after posterior thoracic fusion surgery involves extensive rehabilitation and physical therapy to improve strength and spinal stability.
Associated Risks of Posterior Thoracic Spinal Fusion Surgery
Complications associated with posterior thoracic spinal surgery include spinal cord injury, nerve-root injury, dural injury, cerebrospinal fluid leak, pulmonary injury, infection, and failure to fuse (2)
Recovery Time After Posterior Thoracic Spinal Fusion Surgery
Recovery from surgery on the thoracic spine varies from patient to patient. It is dependent upon the number of levels fused, duration of the surgery, presence or absence of complications during the surgery, and one’s underlying medical condition. Recovery typically takes between three to six months.
Success Rates & Research Relating to Posterior Thoracic Spinal Fusion
Success rates vary depending on the number of levels fused, pre-existing medical conditions, and the skill and expertise of the surgical team. A recent study demonstrated an average success rate of only 61% (3)
Thoracic Laminectomy
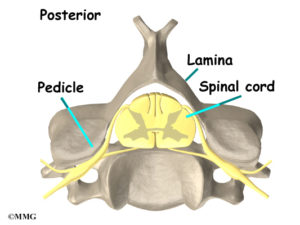
A thoracic laminectomy is a major surgery in which a part of the spinal bone is removed so as to reduce the pressure on the spinal cord and nerve roots. The lamina is the section of bone that is removed. It is located on the backside of the thoracic spine. The spinal canal can be severely narrowed as a result of disc bulge, disc herniation, ligament overgrowth, facet joint overgrowth, and tumors. Removing the lamina decreases the pressure and potential damage to the spinal cord and exiting nerves.
Life After Posterior Thoracic Laminectomy
Life after thoracic laminectomy involves extensive physical therapy to improve spinal stability and muscle strength. Removing the thoracic lamina in many cases provides a reduction in symptoms and pain and improved function.
Associated Risks of a Thoracic Laminectomy
Risks associated with thoracic laminectomy are similar to that of a posterior spinal fusion. Significant risks include infection, failure, escalation in pain, and injury to the spinal cord, nerve root, dural, and lung.
Recovery Time After a Thoracic Laminectomy
There are multiple factors that play a role in the recovery period. These include pre-existing medical conditions such as obesity, diabetes, lung disease, and poor exercise tolerance. Other important factors include the number of levels the laminectomy was performed on, surgical duration, and whether hardware such as screws and plates was utilized.
Success Rate & Research Relating to a Thoracic Laminectomy
Success rates vary depending upon the number of levels decompressed and the indication for surgery. One recent study demonstrated a success rate of only 53% (4).
Posterior Thoracic Discectomy
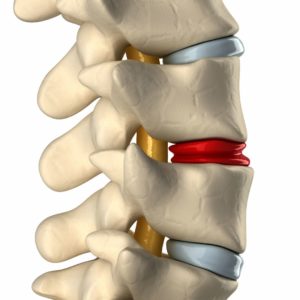
A discectomy is a surgery that involves the removal of the damaged part of the disc. It can be performed at all levels of the spine; cervical, thoracic, and lumbar. The goal of a posterior thoracic discectomy is to remove that portion of the disc that is damaged and causing pain. Thoracic discectomy is also performed to relieve the pressure exerted by the damaged disc on the nerves and the spinal cord. In theory, removing the damaged disc will improve pain and decrease pressure on spinal neural elements such as the spinal cord.
Associated Risks of a Thoracic Discectomy
Risks associated with thoracic discectomy include dural tears, nerve injury, spinal cord injury, vascular complication, infection, escalation in pain, continued degeneration of the affected disc, intercostal neuralgia, and failure.
Success Rate & Research Related to Thoracic Discectomy
The size of the thoracic disc herniation and the presence of any calcification are both predictors of poor outcomes (5). Success rates vary significantly based upon the indication for the thoracic discectomy, levels performed, presence or absence of fusion, and pre-existing medical conditions.
What To Expect
Surgery on the thoracic spine is major surgery. There are several different types which include thoracic fusion, thoracic laminectomy, and thoracic discectomy. There are significant and potentially permanent complications that are life-changing. The rehabilitation and recovery are long with no assurance one will return to baseline. The is no guarantee that the pain and dysfunction will improve and success rates on average are slightly greater 50%.
When Should You Consider Surgical Treatment
Thoracic spine surgery is major surgery with significant potentially permanent complications with no assurance that the pain and dysfunction will improve.
An accurate diagnosis is essential. It will confirm that the pain is actually arising from the thoracic spine. There are many sources of thoracic pain that are overlooked and not evaluated. These include ligaments, facet joints, and costovertebral joints. To learn more about the causes of thoracic pain please click here.
All conservative therapies must be undertaken and exhausted. Traditional pain injections can be helpful in identifying the source of pain. Most importantly thoracic spine surgery should be the treatment of last resort given it invasive nature, long rehabilitation time, need for narcotics, and significant and potentially permanent complications.
Thoracic spine surgery may be required when there is an abrupt onset of bowel and bladder incontinence, lower extremity weakness, and numbness.
Who Is A Candidate For Surgery?
Surgery on the thoracic spine may be the appropriate treatment if:
- Pain is chronic and intolerable
- Nonsurgical treatments have not worked
- Loss of bowel and bladder function.
Can You Treat Thoracic Spine Conditions Without Surgery?
The Centeno Schultz Clinic are experts in the evaluation and treatment of thoracic pain. All physicians are board-certified and fellowship-trained. We view the spine as a functional unit that involves many moving parts that work together. The spine’s stability is critical and is evaluated by examining the integrity of supporting ligaments.
All injections are performed under x-ray or ultrasound guidance. This is to ensure the accurate placement of the needle and injected medicine. It is also used to avoid injury to the lung with the subsequent collapse.
PRP and bone marrow concentrate are utilized to facilitate healing and restore stability. The injections require extensive experience and training due to the complexity of the anatomy. Thoracic injections can not be performed by your PCP or local orthopedic surgeon.
Get The Best Treatment Plan For Your Thoracic Spine Condition
Thoracic spine surgery is a major surgery that requires extensive rehabilitation and is associated with significant and potentially permanent complications. Thoracic spine surgery is no guarantee that the pain will improve and may in fact get worse.
An accurate diagnosis is paramount. One must insist upon an evaluation that identifies the cause of thoracic pain. Then and only then can an appropriate treatment plan be designed. Diagnostic injections with local anesthetics can confirm the source of pain. All conservative treatment should be undertaken. PRP and stem cells can aid in the healing of damaged structures as opposed to high-dose steroids which have significant side effects and can potentially damage discs, facet joints, tendons, and ligaments. To learn about the adverse side effects of steroids click here.
Narcotics mask the pain without treating the underlying condition. Narcotics are associated with addiction.
Are you unsure about getting surgery for your thoracic pain? Schedule an appointment with the experts in thoracic pain at the Centeno-Schultz Clinic. In-office and online evaluations are available where we will review your history, symptoms, treatment to date, and radiographic studies. PRP and bone marrow concentrate treatments are viable alternatives to thoracic spine surgery without the extensive rehabilitation and risks associated with surgery.
Are you unsure about getting surgery for your thoracic spine condition? To schedule please contact Jen at 720-287-7196 or [email protected] or Vanessa at [email protected]. It is time to stop suffering and start living life to its fullest.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate and PRP for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI).
More Resources

The Spine Owner’s Manual: How to Avoid Back Pain & Life-Altering Surgery
This e-book from Dr. Chris Centeno focuses on the spine and how it functions within the human musculoskeletal system and the body as a whole. Everything in our bodies works together like a well-tuned symphony to support our well-being, and a strong spine (including all of its component parts, such as spinal nerves, ligaments, muscles, etc.) is critical to complete health.
Using the Regenexx SANS approach, The Spine Owner’s Manual provides a series of tests and clearly defined exercises that you can do on your own to measure and monitor your own spinal health. These musculoskeletal tests will allow you to monitor where your own body might be struggling to maintain proper stability, articulation, symmetry, and neuromuscular function.
Related Articles
-
Understanding the Thoracic and Lumbar Spines
The thoracic spine and lumbar spine make up a vital nexus of stability and mobility in the human body. In this exploration, we delve into the biomechanics and complexities that define these regions, unraveling their significance in posture, movement, and overall well-being. Understanding the thoracic and lumbar spine not only illustrates the mechanics of our…
-
Effective Thoracic Herniated Disc Treatment Exercises You Can Do
A thoracic herniated disc occurs when the soft center of a spinal disc in the thoracic area of the spinal region ruptures. This condition can lead to symptoms such as pain, numbness, and weakness in the chest, back, and potentially radiating down the arms, legs or abdomen. Effective thoracic herniated disc treatment often involves a…
-
The L5 Vertebra: Everything You Need to Know
The spine, consisting of 33 individual bones called vertebrae, is divided into five major regions: cervical (neck), thoracic (upper back), lumbar (lower back), sacral (pelvic region), and coccygeal (tailbone). These vertebrae are separated by intervertebral discs, which act as cushions and allow for flexibility in movement. The lumbar spine, also known as the lower back,…
-
Understanding the Role Of The Thoracic Spine Muscles
The thoracic spine plays a critical role in the stability and mobility of the upper body. Comprised of twelve vertebrae and an intricate network of muscles and ligaments, it serves as a central pillar supporting the structure and movement of the body. Understanding the role and function of thoracic spine muscles is pivotal for anyone…
-
Exploring the Lumbosacral Joint: What Should You Be Wary Of?
The L5 S1 joint, or the lumbosacral joint, is a critical joint. It lies between the lumbar segment of the spine and the auricular processes of the sacrum. The L5-S1 joint plays a vital role in transmitting the weight of the body via the sacrum and ilium downwards. The weight is distributed to the femur…
References
1.Saavedra-Pozo FM, Deusdara RA, Benzel EC. Adjacent segment disease perspective and review of the literature. Ochsner J. 2014 Spring;14(1):78-83. PMID: 24688337; PMCID: PMC3963057.
2.He B, Yan L, Xu Z, Guo H, Liu T, Hao D. Treatment strategies for the surgical complications of thoracic spinal stenosis: a retrospective analysis of two hundred and eighty-three cases. Int Orthop. 2014 Jan;38(1):117-22. doi: 10.1007/s00264-013-2103-2. Epub 2013 Sep 22. PMID: 24057658; PMCID: PMC3890145.
3.Yamasaki R, Okuda S, Maeno T, Haku T, Iwasaki M, Oda T. Surgical outcomes of posterior thoracic interbody fusion for thoracic disc herniations. Eur Spine J. 2013 Nov;22(11):2496-503. doi: 10.1007/s00586-013-2877-3. Epub 2013 Jun 26. PMID: 23801016; PMCID: PMC3886499.
4.Li X, An B, Gao H, Zhou C, Zhao X, Ma H, Wang B, Yang H, Zhou H, Guo X, Zhu H, Qian J. Surgical results and prognostic factors following percutaneous full endoscopic posterior decompression for thoracic myelopathy caused by ossification of the ligamentum flavum. Sci Rep. 2020 Jan 28;10(1):1305. doi: 10.1038/s41598-020-58198-x. PMID: 31992790; PMCID: PMC6987090.
5. Court C, Mansour E, Bouthors C. Thoracic disc herniation: Surgical treatment. Orthop Traumatol Surg Res. 2018 Feb;104(1S):S31-S40. doi: 10.1016/j.otsr.2017.04.022. Epub 2017 Dec 7. PMID: 29225115.
Am I a Candidate?
To answer this question, fill out the candidate form below to request a new patient evaluation, and a patient advocate will reach out to you to determine your next steps. Your one-hour, in-office or telemedicine evaluation will be with one of the world’s experts in the field of Interventional Orthopedics.