Knee Bursitis
Bursitis is the inflammation of the bursa around the joints. Each year, 1 of every 10,000 individuals globally develops bursitis in the knee and elbow (1). Bursitis can occur in the shoulders, elbows, hips, knees, and feet.
But the knee joint is commonly affected by bursitis because it is a weight bearing joint and is used across a wide variety of daily activities, including walking and squatting.
One-third of individuals with knee bursitis develop septic bursitis, which must be treated immediately or can lead to significant long-term health consequences. Therefore, knee bursitis must be identified, diagnosed, and treated without delay.
What Is Knee Bursitis?
Bursae are small fluid-filled sacs that resemble pillow-like structures. The knee joint is protected by four main bursae: the prepatellar, suprapatellar, infrapatellar, and pes anserine bursa. There are also smaller bursae associated with tendons coming from the thigh and attaching to the tibia.
These bursae lie between the bony prominences of the joint and the soft tissue, like the muscles, tendons, ligaments in the knee. In this way, these bursae reduce friction between these structures as the knee moves, and also acts as a shock absorber to cushion and protect the joint.
However, because of their role, these thin-walled bursae are prone to inflammation as a result of repeated friction, trauma, and medical or autoimmune conditions. Any of these conditions can cause the synovial cells lining the bursae to produce fluid, causing swelling and inflammation, and leading to bursitis.
Types Of Bursitis In The Knee
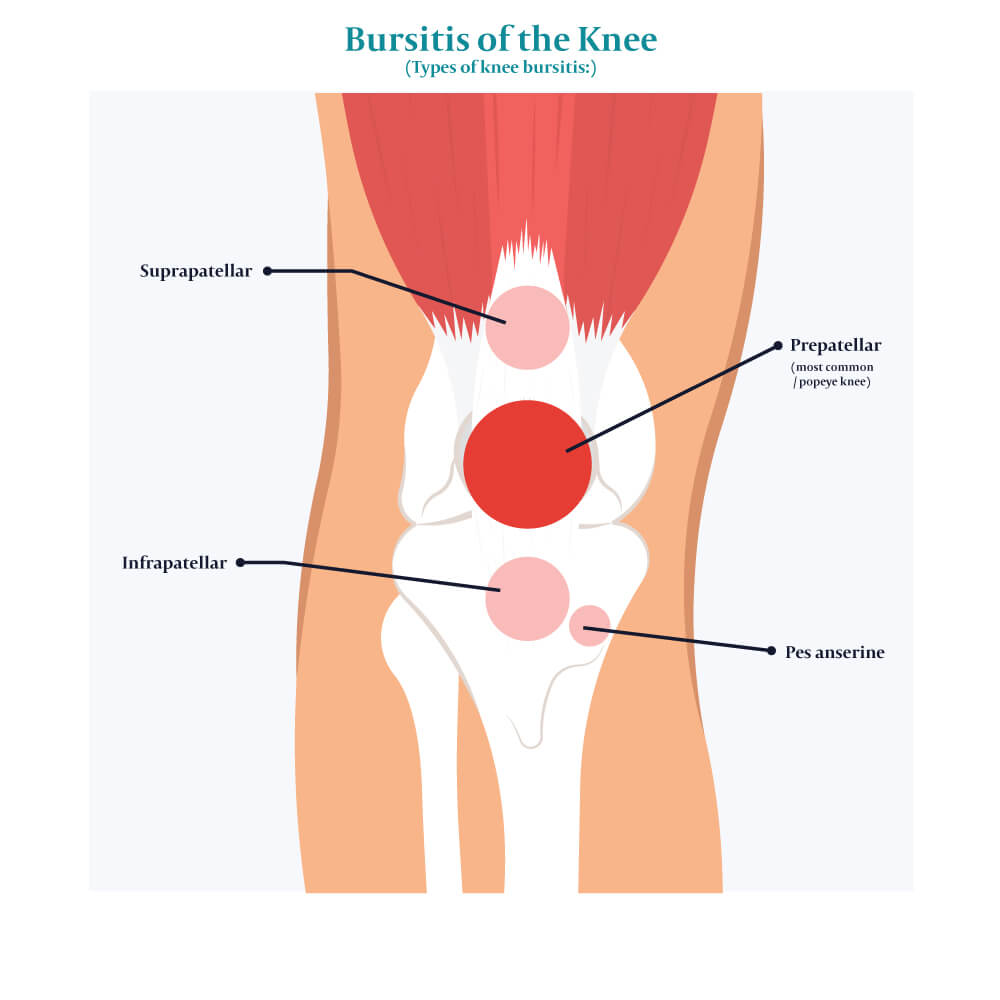
There are several types of knee bursitis, depending on which bursa is affected. The types of knee bursitis include and prepatellar bursitis, suprapatellar bursitis, infrapatellar bursitis, pes anserine bursitis. Bursitis can also develop in the hamstring area or lateral knee, known as semimembranosus bursitis and iliotibial bursitis, respectively.
Prepatellar Bursitis
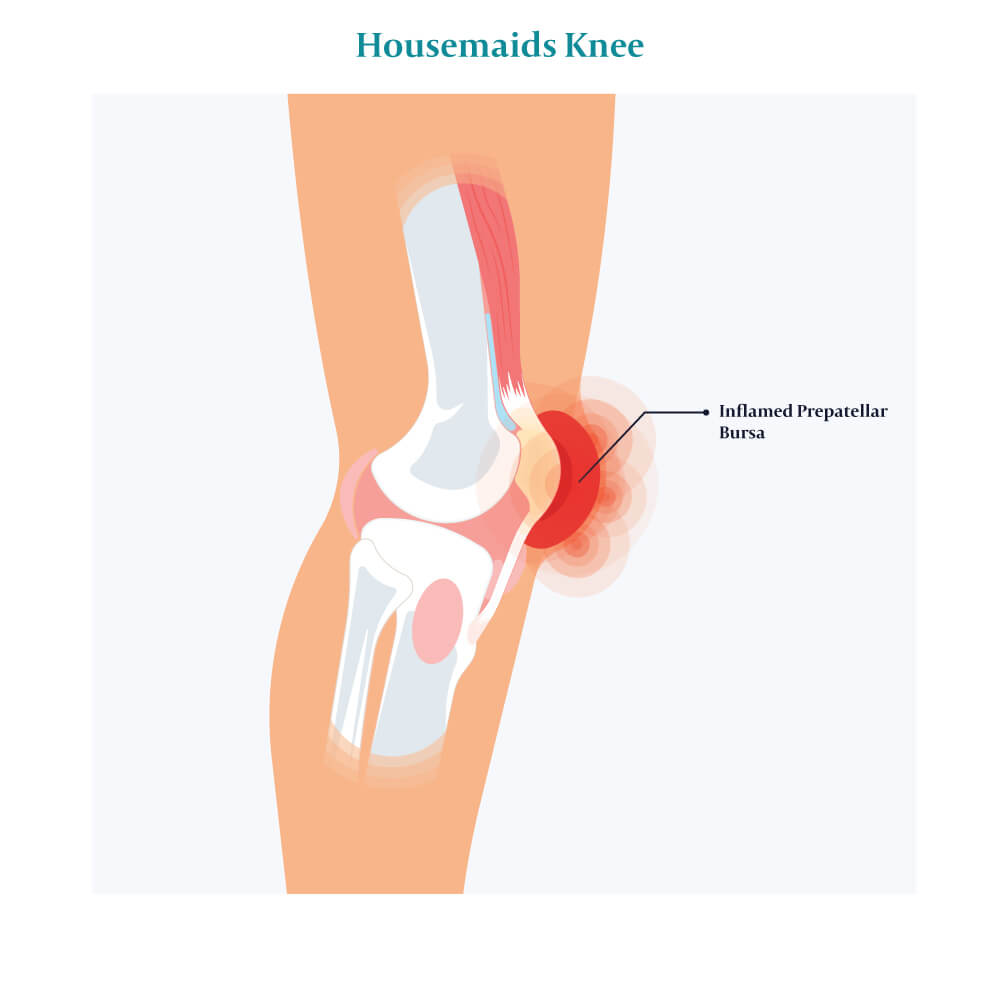
Prepatellar bursitis, commonly known as “Housemaid’s knee,” is the inflammation of the prepatellar bursae. The prepatellar bursa is located directly over the patella (the kneecap) and below the subcutaneous tissue.
It is commonly inflamed in individuals with jobs that require frequent kneeling, like gardening, cleaning, carpentry, and roofing. That is why it is also referred to as housemaid’s knee. Prepatellar bursitis is the second most common bursitis of the human body following elbow bursitis.
Infrapatellar Bursitis
Infrapatellar bursitis is the inflammation of the infrapatellar bursa located just below the kneecap. It is also known as Clergyman’s knee since prolonged kneeling can lead to this type of bursitis. Infrapatellar bursitis can also occur due to trauma or frequent squatting.
There are two components of this bursa. The superficial and the deep component. Bursitis can occur in both the superficial component between the patella and the skin and the deep component which is between the patellar ligament and the tibia.
Pes Anserine Bursitis
The pes anserine region of the knee is the meeting point of three tendons, namely the gracilis, sartorius, and semitendinosus. The inflammation of the bursa between these three tendons is called pes anserine bursitis. Any repetitive motion that activates these tendons, like running, swimming, squatting, or climbing, can cause pes anserine bursitis.
Learn more about the pes anserine bursitis condition on this page.
Semimembranosus Bursitis
Semimembranosus bursitis, also known as a Baker’s cyst, is a type of bursitis where fluid accumulates near the tendon of the semimembranosus at the back of the knee. It occurs due to injury of the bursa caused by repetitive muscle contractions.
They are commonly found in the posterior capsule of the knee joint. The symptoms largely depend on the size of the cyst. This form of bursitis is usually found with other knee joint pathologies particularly meniscus tears.
Iliotibial Bursitis
Iliotibial bursitis, also known as iliotibial band (ITB) syndrome, is commonly seen in long-distance runners, cyclists, weightlifters, and skiers.
Repetitive friction of the iliotibial band, a sturdy band of tissue that originates from the glutes and tensor fascia lata, can lead to inflammation of the ITB bursa.It is characterized by pain on the outside of the knee that is worsened with movement. Any mechanical problem of the knee can also lead to ITB like uneven leg length and bow legs.
Symptoms Of Knee Bursitis
When the bursa becomes inflamed, fluid starts accumulating. Doctors call this “effusion”, which means the excessive accumulation of fluid. Most of the symptoms of knee bursitis are due to this slow-developing effusion. WIth that in mind, here is a list of all the symptoms you may experience with knee bursitis:
A Soft Lump In The Front Of The Knee
Effusion may begin as a small area of swelling that progressively increases in size. Swelling can be tender, and the area will often be warm or hot to touch. Studies show that if the skin over the affected bursa has a temperature that is 2.2⁰ higher than the contralateral knee, it is highly suggestive of an infected bursa.
Localized Knee Pain
Localized knee pain is quite common in knee bursitis. In traumatic conditions, the pain is more acute and severe.
However, with a slowly developing bursitis, the pain is often mild and gradually increases in intensity, especially if there is an infection. The pain also worsens with movement, such as when the muscles related to the affected bursa are active.
An important thing to keep in mind is that localized knee pain may not always be present in chronic bursitis.
This is because, in chronic conditions, the bursa has had time to accommodate the swelling and, in response, the walls of the bursa simply become thicker. There may also be an absence of pain in chronic bursitis due to this adaptation as well.
Limited Motion
The presence of a painful lump can limit the movement in the knee joint and surrounding joints. Depending on which bursae are affected, movement in certain planes can be very painful or stiff. In some cases, this discomfort prevents people from going about their daily activities. People may also feel as if the muscles have less strength since the joint can feel stiff and tight.
Common Causes Of Bursitis In The Knee
There are many causes of bursitis in the knee. Occupational stressors, autoimmune conditions, infections, and trauma are some of the more common causes of knee bursitis. Let us look at the causes of knee bursitis in detail.
Knee Bursitis Due To A Direct Blow To The Knee
- Trauma: A sharp blow to the kneecap can cause prepatellar bursitis by rupturing the ligaments leading to an inflammatory response. The bursae get filled with fluid as the ligaments and muscles are subject to infiltration with white blood cells and other inflammatory chemicals.
- Sports: Many athletes in sports like rugby, soccer, hockey, and other contact sports sustain direct hits to their knee joint, which can lead to acute knee bursitis. Here a direct it to the bursa injures them and causes them to produce more fluid. This fluid is rich in repair cells.
- Puncture wounds: An accident where the skin over the kneecap is broken from a direct blow to the knee can also lead to knee bursitis. This injury can introduce bacteria, viruses and fungi into the sterile bursae leading to septic bursitis.
Knee Bursitis Due To Repeated Irritation
- Occupational stressors: Constant irritation due to the friction of repetitive motion in certain occupations can lead to knee bursitis. Gardeners, installers, carpet layers, plumbers, and roofers frequently kneel or squat to do their job, and this friction can cause knee bursitis.
- Sports: Certain sports that require repetitive movements of the knee, such as flexion or extension, can cause knee bursitis. The repeated actions tend to wear down the ligaments and inflame them. If not allowed to recover, fluid accumulates in response to this inflammation leading to bursitis. This includes cycling, skiing, weightlifting, and hockey.
Knee Bursitis Due To An Infection In The Bursa
The bursa is a sterile sac and any cut or wound on the skin overlying the bursa can introduce bacteria, leading to an infection. A third of all knee bursitis is caused by bacteria. Infection of the bursae can result from a puncture wound, a fall, or even a systemic infection.
Other Causes Of Knee Bursitis
- Autoimmune conditions: Autoimmune conditions like rheumatoid arthritis, Sjogren’s disease, gout, and SLE( Systemic lupus erythematosus) can cause knee bursitis.
In these autoimmune conditions, the body’s antibodies no longer recognise the body’s cells, so they attack the joints, which can affect the bursae and cause inflammation and pain. - Age-related changes: Osteoarthritis due to wear and tear of the joint over time can also lead to inflammation in the bursae of the knee. Individuals with osteoarthritis have a higher risk of knee bursitis due to the constant presence of inflammatory cells.
The inflammation wears down the joint and constantly attacks the ligaments and bursae making them more susceptible to bursitis. - Immunocompromised conditions: People with diabetes mellitus, HIV, cancer, and chronic alcoholics, may have poor immunity. These individuals are therefore easily susceptible to infections and are at a higher risk of septic bursitis.
Common Treatments For Bursitis In The Knee
Most cases of bursitis will heal on their own through natural and supportive care. In individuals with pain, the intensity of the pain determines the pain medications. In addition to pain relief, physical therapy can restore the functionality of the joint over a period. Patient education is also important to prevent any exacerbation and recurrence of the injury.
Knee Arthroscopy Surgery
Knee arthroscopy surgery is a very common procedure performed by orthopedic surgeons in an attempt to treat knee pain. Knee arthroscopic surgery is typically performed in an outpatient surgical facility where a small camera is inserted into the knee joint, which allows the surgeon an inside view of one’s knee to operate. It is used both to diagnose and treat a wide variety of knee problems. Utilizing arthroscopic surgery the surgeon can trim any damaged ligaments which are called knee ligament surgery. Alternatively, if ‘damaged’ meniscus is detected, it also is trimmed and or removed, which is called meniscus knee surgery.
Read More About Knee Arthroscopy SurgeryNSAIDs
The other day I was evaluating a patient and reviewing the treatment options for their spine condition. After discussing prior treatments, we got to the topic of medications taken for pain relief. She explained that she mainly utilized anti-inflammatory (NSAID) medications and then she told me to hold much she takes and has been for many years…..she takes close to 2 grams (2000 milligrams) on a daily basis which equated to about 9-10 capsules of medication per day. I was shocked, considering she was pre-diabetic and with high blood pressure plus the kicker of it is that her PCP (primary care physician) is ok with this…
Read More About NSAIDsProlotherapy Injections
It has been successful in the treatment of many disorders including neck, shoulder, knee, and ankle pain. Dr. Centeno recently published an article in The Journal of Prolotherapy in which he discusses the use of x-ray guidance with prolotherapy. This ensures that the injection is in the correct place to maximize clinical results. Dr. Centeno discusses the use of prolotherapy for the treatment of neck, knee, sacroiliac joint, ankle, ischial tuberosity, and shoulder pain. At the Centeno-Schultz Clinic x-ray guided prolotherapy is just one of the therapies utilized in the successful treatment of pain. Regenerative injection therapy (RIT) or prolotherapy…
Read More About Prolotherapy InjectionsPRP Injections
PRP is short for platelet-rich plasma, and it is autologous blood with concentrations of platelets above baseline values. The potential benefit of platelet-rich plasma has received considerable interest due to the appeal of a simple, safe, and minimally invasive method of applying growth factors. PRP treatments are a form of regenerative medicine that utilizes the blood healing factors to help the body repair itself by means of injecting PRP into the damaged tissue. In regenerative orthopedics, it is typically used for the treatment of muscle strains, tears, ligament and tendon tears, minor arthritis, and joint instability. There have been more than 30 randomized controlled trials of PRP…
Read More About PRP InjectionsPRP Knee Injections
PRP stands for Platelet-Rich Plasma. Platelets are blood cells that prevent bleeding. They contain important growth factors that aid in healing. Plasma is the light yellow liquid portion of our blood. So PRP is simply a concentration of a patient’s own platelets that are suspended in plasma and are used to accelerate healing. PRP is NOT stem cell therapy. Regrettably, blood contains few circulating stem cells. Rich sources of stem cells are bone marrow and fat. PRP is rich in growth factors. There are many different types of growth factors with different properties. VEGF is a very important one as it can increase the blood flow to an area.
Read More About PRP Knee InjectionsDiagnosing Knee Bursitis In Patients
Knee bursitis can mimic gout, rheumatoid arthritis, osteoarthritis, and meniscal tears. The treatment for all these conditions is vastly different, so it is important to identify and diagnose knee bursitis correctly.
Your primary care physician and orthopedic doctor are the ones who will examine and diagnose you with knee bursitis. Some of the ways to diagnose knee bursitis are listed below.
A Review Of The Medical History
The medical history is a key element to diagnose knee bursitis. The individual’s occupational history, history of recreational activity, the pattern of knee pain, the onset of symptoms, and the aggravating and easing factors are important to identify the cause of the knee bursitis.
Any previous injuries in the past, particularly in the knee, and the presence of other medical conditions that may affect the joints are also important to diagnose bursitis. This can include chronic conditions like diabetes, HIV, SLE, rheumatoid arthritis, gout, kidney disease, and osteoarthritis.
Physical Tests
Doctors will do the physical exam to locate which bursae are affected. It can also help rule out other causes of the symptoms or damage to the ligaments or tendons in the knee. An orthopedic doctor usually will perform the exam and is the best person to diagnose knee bursitis.
- Skin Exam: The first step of the physical exam of the knee is an examination of the skin overlying the knee to identify any redness, warmth, and any wounds.
- Patellar assessment: The doctor will then assess the patella by palpating the area and checking the range of motion. In particular, they are checking for “the bulge sign” which is the presence of fluid when the patella is moved sideways.
Based on the bulge of the medial aspect, the amount of fluid within is estimated.The doctor may also complete a patella tap test to see if the patella moves downwards. An audible tap signifies moderate fluid within the joint. - Cartilage testing: The doctor can also complete other tests to help rule out causes of knee swelling. Apley’s grind test and McMurray’s test are used to check for cartilage tears in the knee.
- Laxity assessment: To check for the laxity of the patella and the patellar ligament ligament, the Lachman test is used. It is also used to test the anterior cruciate ligament.
Imaging Tests
Your doctor may use one or all the physical exam tests based on their clinical suspicion. However, they may also order imaging tests to confirm the diagnosis of bursitis, and rule out other more serious conditions like a fracture or a ligament tear. Some of the imaging tests include:
- X-ray: Plain films are always completed when there is acute trauma to the knee in order to rule out fractures or the presence of a foreign body.
- Ultrasound: An ultrasound is the best method to identify bursitis. Ultrasounds can visualize the bursae during both active and passive motion. A doctor can measure the fluid in the joint with the help of an ultrasound. It can also be used to guide needle aspirations of the joint for treating bursitis. It is usually done after plain films have ruled out a fracture.
- MRI: An MRI is not necessary for diagnosing bursitis, but it may be ordered if a ligament tear is suspected. It can also be useful to visualize the deeper bursae of the knee.
- CT: A computed tomography (CT) scan is not usually needed unless the doctor wants to check the muscles and ligaments in and around the knee, or suspects a tumor in the knee joint.
Aspiration Of The Knee
Aspiration can be both diagnostic and therapeutic. Aspiration is a surgical procedure where a doctor will use a needle and syringe to draw out fluid from the bursa to assess it for white blood cells, the presence of microbes, red blood cells, and other substances. This is done especially when there is a palpable swelling in conjunction with limited range of movement.
Most people will find immediate relief when the fluid is aspirated from the joint. The joint fluid is then sent for testing to determine the cause of bursitis. Gram stains of the joint fluid will identify the bacteria in the fluid.
Preventing Bursitis In The Knee
You can prevent knee bursitis by taking a few steps:
- Using a knee support when working: Knee braces and knee supports are good for those who work in occupations that require them to frequently kneel and squat. These braces and supports can cushion the joint and reduce the friction on the knee and bursae.
- Exercises: To prevent the bursae from getting inflamed, it is good to always warm up the muscles before starting any strenuous activity as this can increase blood flow and oxygen to the area. Hamstrings stretch, quad stretches, calf stretches, leg lifts, leg raises, and heel slides can be used as both a warm up and also to strengthen the knee joint.
- Reduce stress to the knee: Avoid injuries to the knee where possible. Additionally, try not to overload your muscles by maintaining an optimal weight and resting frequently, particularly if you have a manual job or compete in contact sports. Avoid sitting or kneeling for too long as well, and if you must sit close to the floor, then use a stool.
- Understand your body: If you have knee pain with certain activities and exercises, discontinue them until the knee is healed. Do not overwork the muscles and the joint. Additionally, make sure you allow your body to rest adequately in between different activities.
If you find your knee is getting sore, ice it to prevent it from swelling and to reduce inflammation. If the knee swells or the pain is severe or worsening over time, then seek medical help.
Recovering From Knee Bursitis
The recovery from knee bursitis depends on the severity of the condition and the treatment. Irrespective of the type of treatment, you will need physical rehabilitation to strengthen the knee joint. Rehab plays a big role in recovery and prevention of further injuries to the bursae.
Conservative treatment includes RICE therapy, supportive therapy, phycial therapy and medications. With conservative treatment, it should take about three weeks to fully recover. Septic bursitis can take about six to twelve weeks and is treated with antibiotics.
For those who need surgery, you will need a period of immobilization to recover. Then it will take about two to four weeks until you can move around fully or once the inflammation subsides. Following this, you will start physical exercises for flexibility and full range of motion which can take about three to six weeks.
The Prognosis For Knee Bursitis
Knee bursitis has an excellent prognosis if it is diagnosed accurately and treated promptly. Complications can arise if there is a delay in treatment, or after surgery. That is why it is important to treat knee bursitis early and that the relevant healthcare professionals are involved to prescribe and oversee the appropriate treatment and management plan.
If you suspect you have bursitis of the knee, schedule a consultation with one of our board-certified, fellowship-trained doctors to discuss your treatment options.
Doctors that Treat Knee Bursitis

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreMore Resources for This Condition
-
What Is Golfer’s Knee, And What Can I Do About It?
The nature of golf is such that both the backswing and downswing affect the knee. The entire swing takes a little over one second. However, it can exert a force of 4 times the body weight on the front knee and 3 times the weight on the back knee (1). This makes knee injuries just as…
-
Knee Pain Location Chart: What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
Understanding Knee Pain Symptoms To Get The Best Treatments
Knee pain affects about 25% of the population (1). The knee joint involves three bones, namely the patella, the femur, and the tibia. Knee pain can be a sign of damage to the ligaments, bones, bursae, or muscle tendons because there are so many structures within the knee joint. In this post, we’ll discuss the…
-
KT Tape For Hamstring Tendonitis
Hamstring tendinosis is a condition that causes pain and inflammation in the hamstring tendons. The hamstring tendons are the tough bands of tissue that attach the hamstring muscles to the bones in the back of the thigh. Hamstring tendinosis is a degenerative condition, meaning that it is a condition that causes the tissue to break…
-
6 Meniscus Tear Types And How To Treat Them Properly
Even a small meniscus tear can make walking difficult for you. If you are experiencing any of these symptoms, you may want to seek medical help as soon as possible, depending on the type of tear you have. Needless to say, a lot depends on understanding the meniscus tear types there are and what each…
-
How To Heal A Torn Meniscus Naturally
If you have, or suspect you have a torn meniscus, and you’re wondering how to heal a torn meniscus naturally, you’ve landed on the right post. You may be wondering: Do I need surgery? Can you heal a torn meniscus naturally? The short answer is: It depends. What Is a Meniscus? The meniscus is a…
Ready to get help for your knee bursitis?
References
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Bursitis: Overview. 2018 Jul 26. Available from: https://www.ncbi.nlm.nih.gov/books/NBK525773/
