If you have, or suspect you have a torn meniscus, and you’re wondering how to heal a torn meniscus naturally, you’ve landed on the right post.
You may be wondering: Do I need surgery? Can you heal a torn meniscus naturally? The short answer is: It depends.
What Is a Meniscus?
The meniscus is a fibrocartilage structure that sits on top of the tibia (lower leg bone). There is one on the medial (inside) aspect of the knee, one on the lateral (outside) aspect of the knee. It is shaped like a C and provides some cushion and support for the knee joint as it acts as a shock absorber.
How Can You Tear Your Meniscus?
A meniscus can be torn with particular injuries typically with sports, twisting, deep knee bending, rotating, or high-intensity type activities, which can sometimes cause some pain and dysfunction. Also, it can just gradually tear or wear out through degeneration throughout the years as we age, which may or may not cause any symptoms whatsoever. Most people believe that if they see a torn meniscus on MRI this automatically means that they may need to have surgery to fix the issue, but this is usually not the case. In fact, if you just get MRIs of people over age 35, most people would likely have a meniscal tear, and most of those folks will not have any symptoms of knee pain whatsoever (1).
Meniscal Surgery Outcomes and Complications
Again, many people believe that meniscal surgery is needed if a meniscal tear is found on MRI and you have some knee pain. However, what is the evidence that having a meniscal surgery would help, and what are the types of meniscal surgeries? About ninety-six percent of the meniscal surgeries that are performed currently are meniscectomies, where the part of the meniscus that is torn or injured is cut and removed.
This is despite many times this being called a meniscal “repair.” Another type of surgery, which is rarer, which is a true meniscal repair is where parts of the meniscus are sewn back together to try to get that meniscus to heal up rather than removing a piece of tissue. Most of the research on arthroscopic surgery, (going in with a scope) for partial meniscectomy shows that the surgery does not work. There was a 2013 study showing that it could not beat physical therapy (2).
There is another study that showed that there was no difference from a fake surgery where you just went in with a scope and performed no procedure (3). Another study showed that surgery was no better than placebo therapy even when the patient had locking and mechanical-type symptoms with a meniscal tear (4). There is even further evidence that suggests that meniscal surgery does not work and can even be harmful to the knee, as removing parts of the meniscus alters the biomechanics of the knee, puts more stress and wear on the cartilage, progressing arthritis at a much faster rate, and, more commonly, leads to a knee replacement (5,6).
There is another study that showed patients that had meniscal surgery were 2.5 times more likely compared to the knee without surgery, even if it had a meniscus tear, to require knee replacement (7,8). Are there any patients that should get this type of surgery? There may be a handful of folks that do have some true mechanical clicking from a specific flap or bucket-handle tear of the meniscus that are not getting better with physical therapy or conservative measures but that is few and far between whereas right now meniscectomy is the most common elective orthopedic surgery despite having multiple research papers showing that it does not work and makes you worse. A true meniscal repair sounds like a much better idea and but is less commonly performed. It usually only can be performed on folks without arthritis, younger people, and only with specific types of tears.
Types of Meniscal tears
Meniscal tears come in a variety of different types, which can affect potential treatments, symptoms or relevance.
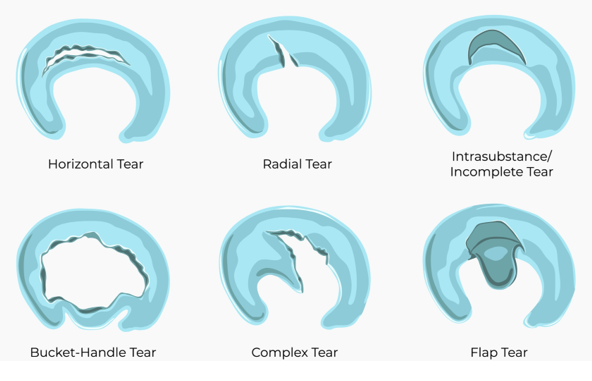
- One type of tear is a radial tear, which is just a left to right tear across the meniscus (see Figure 2 – top row, middle). These are the most common types. Most commonly they are in what we call the white zone of the meniscus where it does not get much blood supply. Thus they are hard to heal naturally, so if you see a surgeon they will likely try to cut this part out despite the evidence saying that a meniscectomy does not work.
- The next type of tear is a horizontal tear, which is basically an up and down or front to back tear in the meniscus (see Figure 2 – top row, left). Many times these tears are in a portion of the meniscus that does get blood supply so they could potentially heal on its own. If they do not heal naturally then surgical repair can sometimes be tried to help.
- The next type of tear is a complex tear where you have a combination of different tears where it can be torn in multiple areas of the knee (see Figure 2 – bottom row, middle). Oftentimes when the surgeon sees these, they would attempt a meniscectomy again because most of the time these are difficult for them to try to repair.
- Next type of tear is an intrasubstance tear. Usually these are just degenerative tears in the midportion of the meniscus. Typically, surgeons will not even try to operate on these. After age 30, these are very common findings of a meniscal tear on MRI, which is of little consequence.
- Another type of tear is a bucket-handle tear. This is a tear where the meniscus is torn and flipped over like a bucket-handle (see Figure 2 – bottom row, left). These sometimes can cause some catching or alter the motion of the knee. If that is the case then those would be the rare type of tear that actually would need surgery.
- The next type of tear is a flap tear where a small piece of meniscus can be torn and flipped over (see Figure 2 – bottom row, right). Sometimes this can cause some catching of the knee, sometimes it does not hurt. If there is no catching in the knee, then it would not warrant any surgery to remove that part of the meniscus. If it is causing some catching or altering motion of the knee that might be a rare case where surgery may be indicated.
- Lastly, another rare type of tear is a tear in the root of the meniscus, which was the back part of the meniscus that anchors it onto the tibia. Depending on the nature of this tear, this one can be something that may need some surgical repair to hold it down, but again meniscectomy would not be a good choice for this as this can increasingly make the meniscus more unstable.
- The meniscus also can be what is called extruded, where it sticks out the joint either from natural tearing or from after a meniscectomy. When a meniscus extrudes after surgery it is more abrupt and tends to progress arthritis much faster, whereas if it happens naturally, it is more of a gradual change that your body can many times adapt to.
Natural Remedies For a Torn Meniscus
If you have knee pain and have been told you have a suspected meniscal tear either from an exam or from MRI, much of the time this can heal on its own with 4-6 weeks of rest, doing some physical therapy that would focus on some range of motion and strengthening exercises and correcting any biomechanical problems that may stem from the core, back, hips or the ankles. Nutritional support such as just working on a healthy diet, reducing inflammation in the body, taking some turmeric, fish oil, glucosamine, and chondroitin, can help knee pain and inflammation as well.
Treatments For A Meniscal Tear Without Surgery
- If you go to most pain practices if you fail physical therapy and surgery is not recommended, they may recommend a steroid injection, which can help temporarily reduce inflammation in and around the knee and meniscus, but this is not advised as steroids as we know can cause damage to the joint cartilage, inhibit healing, and has a host of other negative side effects.
- An injection of something called hyaluronic acid, which is a naturally occuring substance that makes up part of the lubricating fluid of the knee joint, could be used for temporary pain relief. It does not help repair the area but may provide a few months of symptomatic benefit if there is not severe arthritis in the knee.
- If you actually want to try and get the body to heal that meniscus on its own when rest and physical therapy has not do the job, PRP has excellent evidence that it helps with meniscal injuries as well as mild to moderate arthritis that can be associated with these issues. PRP, when used in the right hands, should be injected precisely with ultrasound guidance into the torn parts of the meniscus, into any ligaments or tendons that may be injured or loose, and into the knee joint itself for optimal results. Many practitioners just inject into the knee, which still can help quite a bit but not as much as if a more thorough approach is taken. There are more than 25 high level studies showing PRP helps with knee pain (Orthopedic Bone Marrow Stem Cell Historical Timeline (netdna-ssl.com)).
- Bone marrow concentrate that contains the patients stem cells can also be used to promote the body’s healing in more severe meniscal tears or if there are meniscal tears with more moderate to severe arthritis. There are a few randomized control trials that show that this can be helpful for that as well (9-11). Again, you want to have a thorough skilled approach to make sure that image guidance is used, and all of the damaged parts of the meniscus and associated areas of the knee such as tendons, ligaments, and joints are injected as well.
The latter two options are what we focus on at the Centeno-Schultz Clinic, promoting the body’s ability to heal itself with highly specific image-guided procedures that use the body’s own PRP and bone marrow concentrate. These Interventional Orthopedic procedures, performed by board certified specially trained physicians maintain the natural anatomy and structure of the joint, and have more research that is positive than meniscal surgeries. On the other hand, the research on Meniscal surgery shows that except for the rare cases of a flap or bucket-handle tear that can cause mechanical symptoms the surgery is largely ineffective.
Bottom Line
Meniscal tears are common findings in the knee, which many times are of little clinical significance.
If a meniscal tear is associated with pain, depending on the tear, most of these can be handled with nonsurgical treatment measures. When the traditional measures of rest, physical therapy, diet and supplements fail, then PRP and bone marrow concentrate for more severe problems can be a great alternative to help the body heal itself, reducing pain, keeping the natural anatomy, and reducing the risk for future surgeries. Meniscal surgery, despite being the most common orthopedic surgery has little evidence to support it and actually good evidence to suggest that we should eliminate the majority of these types of surgeries. If you or anyone you know has a meniscal tear or knee pain and are interested to see if you are a candidate for our non-surgical treatment for knees, please contact us. We are world experts at helping the body heal itself through regenerative measures for orthopedic problems.
References
(1) Risberg MA. Degenerative meniscus tears should be looked upon as wrinkles with age—and should be treated accordingly. British Journal of Sports Medicine 2014;48:741. http://dx.doi.org/10.1136/bjsports-2014-093568
(2) Katz JN, Brophy RH, Chaisson CE, et al. Surgery versus physical therapy for a meniscal tear and osteoarthritis [published correction appears in N Engl J Med. 2013 Aug 15;369(7):683]. N Engl J Med. 2013;368(18):1675–1684. doi:10.1056/NEJMoa1301408
(3) Sihvonen R, Paavola M, Malmivaara A, Itälä A, Joukainen A, Nurmi H, Kalske J, Järvinen TL; Finnish Degenerative Meniscal Lesion Study (FIDELITY) Group. Arthroscopic partial meniscectomy versus sham surgery for a degenerative meniscal tear. N Engl J Med. 2013 Dec 26;369(26):2515-24. doi: 10.1056/NEJMoa1305189.
(4) Sihvonen R, Englund M, Turkiewicz A, Järvinen TL; Finnish Degenerative Meniscal Lesion Study Group. Mechanical Symptoms and Arthroscopic Partial Meniscectomy in Patients With Degenerative Meniscus Tear: A Secondary Analysis of a Randomized Trial. Ann Intern Med. 2016 Apr 5;164(7):449-55. doi: 10.7326/M15-0899.
(5) Netravali NA, Giori NJ, Andriacchi TP. Partial medial meniscectomy and rotational differences at the knee during walking. J Biomech. 2010 Nov 16;43(15):2948-53. doi: 10.1016/j.jbiomech.2010.07.013.
(6) Cohen SB, Short CP, O’Hagan T, Wu HT, Morrison WB, Zoga AC. The effect of meniscal tears on cartilage loss of the knee: findings on serial MRIs. Phys Sportsmed. 2012 Sep;40(3):66-76. doi: 10.3810/psm.2012.09.1983.
(7) Longo UG, Ciuffreda M, Candela V, Rizzello G, D’Andrea V, Mannering N, Berton A, Salvatore G, Denaro V. Knee Osteoarthritis after Arthroscopic Partial Meniscectomy: Prevalence and Progression of Radiographic Changes after 5 to 12 Years Compared with Contralateral Knee. J Knee Surg. 2019 May;32(5):407-413. doi: 10.1055/s-0038-1646926.
(8) Katz JN, Shrestha S, Losina E, Jones MH, Marx RG, Mandl LA, Levy BA, MacFarlane LA, Spindler KP, Silva GS; MeTeOR Investigators, Collins JE. Five-year outcome of operative and non-operative management of meniscal tear in persons greater than 45 years old. Arthritis Rheumatol. 2019 Aug 20. doi: 10.1002/art.41082.
(9) Centeno C, Sheinkop M, Dodson E, Stemper I, Williams C, Hyzy M, Ichim T, Freeman M. A specific protocol of autologous bone marrow concentrate and platelet products versus exercise therapy for symptomatic knee osteoarthritis: a randomized controlled trial with 2 year follow-up. J Transl Med. 2018 Dec 13;16(1):355. doi: 10.1186/s12967-018-1736-8. PMID: 30545387; PMCID: PMC6293635.
(10) Hernigou P, Bouthors C, Bastard C, Flouzat Lachaniette CH, Rouard H, Dubory A. Subchondral bone or intra-articular injection of bone marrow concentrate mesenchymal stem cells in bilateral knee osteoarthritis: what better postpone knee arthroplasty at fifteen years? A randomized study. Int Orthop. 2020 Jul 2. doi: 10.1007/s00264-020-04687-7. Epub ahead of print. PMID: 32617651.
(11) Hernigou P, Delambre J, Quiennec S, Poignard A. Human bone marrow mesenchymal stem cell injection in subchondral lesions of knee osteoarthritis: a prospective randomized study versus contralateral arthroplasty at a mean fifteen year follow-up. Int Orthop. 2020 Apr 23. doi: 10.1007/s00264-020-04571-4. Epub ahead of print. PMID: 32322943.

