Our preferred Treatment for Meniscus Tears is PRP
Learn MoreMeniscus Tears
The medial and lateral menisci in the knee joint have an essential role. They act as shock absorbers, lubricate the joint, and transfer the load to stabilize the knee. The menisci are the most commonly injured structures in the knee. If you have a torn meniscus, keep reading to learn how it’s diagnosed and treated.
What Is A Meniscus Tear?
The medial and lateral menisci are crescent-shaped fibrocartilages that sit between the femur and tibia. They occupy nearly 70% of the joint surface, and their primary role is to transmit the load across the tibiofemoral joint.
The outer border of the medial meniscus is attached to the joint capsule and the medial collateral ligament (MCL). As a result, the medial meniscus is less mobile than the lateral meniscus, making it more susceptible to injury and tears.
Meniscal tears occur when the knee joint has a large rotational or shearing force. This can happen when these forces occur while the knee is in motion, such as kneeling, squatting, or weightlifting.
Any activity or sport with rapid acceleration and deceleration, a sudden change in direction, or jumping also increases the forces on the knee, which can cause meniscal tears. In someone with degenerative joint changes from arthritis or previous injuries, the menisci are more susceptible to tears.
It is important to also understand that most meniscus tears are not symptomatic! Meaning, meniscus tears are as common as wrinkles or gray hairs. If we MRI’d 100 people on the street with no knee pain over 40 – 80% of them likely would have a meniscus tear on imaging.
Today, we will review all things meniscus but know just because you have a meniscus tear on imaging, does NOT mean that is the cause of your knee pain!!
Six Types Of Meniscus Tears
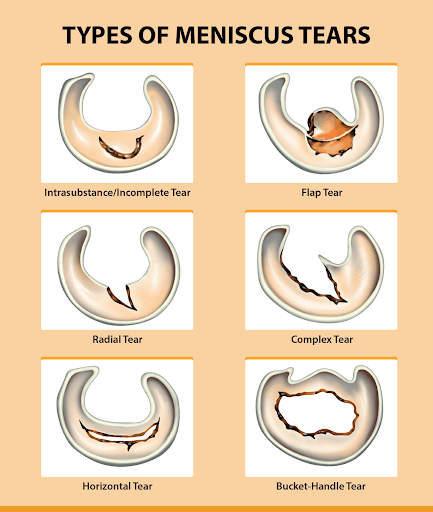
There are six types of meniscus tears: an intrasubstance (incomplete) tear, a flap tear, a radial (transverse) tear, a complex tear, a horizontal (longitudinal) tear, and a bucket handle tear. There is also an isolated tear called the parrot beak tear.
Intrasubstance Tear (Incomplete)
In most cases, intrasubstance tears, also known as incomplete tears, are degenerative tears in the midportion of the meniscus. After age 30, these are pervasive findings on MRI. For this type of tear, physical therapy is the first line of treatment.
Incomplete tears can also occur due to arthritis. When this is the case, there are several treatment options in addition to physical therapy.
For mild to moderate arthritis, Platelet-Rich Plasma (PRP) can help. If the arthritis is moderate to severe, then Bone Marrow Concentrate (BMAC) may be a better treatment option. Most surgeons will not even try to operate on incomplete tears as meniscus surgery doesn’t help and a meniscectomy can worsen the knee.
Flap Tear
A flap tear occurs when a small piece of the meniscus is torn and flipped over. This can cause a catching sensation in the knee, but sometimes it does not hurt. If there is no catching in the knee, then surgery would not be required to remove the affected part of the meniscus.
Physical therapy is the first-line treatment for a flap tear, but PRP and BMAC are also options. If the tear is causing a catching sensation or altered knee motion, it might be a rare case where a partial meniscectomy surgery is indicated to remove part of the affected meniscus as these tears are difficult to repair.
Radial Tear (Transverse)
A radial tear is a left-to-right or “transverse” tear across the meniscus. They are the most common type of tear and usually occur in “the white zone” of the meniscus – the area of the meniscus where it does not get much blood supply. Thus, meniscus radial tears are hard to heal naturally. Physical therapy is the first-of-line treatment, but patients may benefit more from PRP or BMAC.
If you consult a surgeon, they will likely try to cut the affected part of the meniscus out (called a meniscectomy). However, the evidence says that a meniscectomy does not work and can worsen the knee, so it should not be done for these types of tears (1).
Complex Tear
A complex tear occurs with a combination of different tears – the meniscus can be torn in multiple knee areas. Often, when the surgeon sees these, they will attempt a meniscectomy to remove the affected meniscus as, most of the time, these are difficult to repair.
Horizontal Tear (Longitudinal)
A horizontal tear occurs when the meniscus has an up-and-down or front-to-back tear. Many times these tears are in a portion of the meniscus that does get blood supply (called the red zone), so these types of tears can potentially heal on their own. Physical therapy is the first-line treatment and is often effective.
If the meniscus does not improve naturally or with physical therapy, your physician may recommend arthroscopic surgical repair. A surgical meniscectomy should NOT be done for these tears as they can worsen the knee.
PRP and BMAC containing stem cells is an alternative treatment to surgery that can help heal these tears. These treatments are natural, safe, and have better recovery times than surgery. Therefore, these should be done before considering surgery in most cases. They can also be used in conjunction with surgery to improve surgical results.
Bucket-Handle Tear
A bucket-handle tear occurs when the meniscus rips away from the back of the knee and gets overturned like a bucket handle. It can cause a locked knee because the meniscus fragment gets displaced to the front of the joint. This prevents the knee from straightening out fully.
A bucket-handle tear is a rare type of tear that may need surgery. Typically, a meniscectomy is done as the tear may not respond to surgical repair. If this type of tear doesn’t have mechanical knee symptoms like catching/locking, then the tear may be helped with physical therapy, PRP, or BMAC.
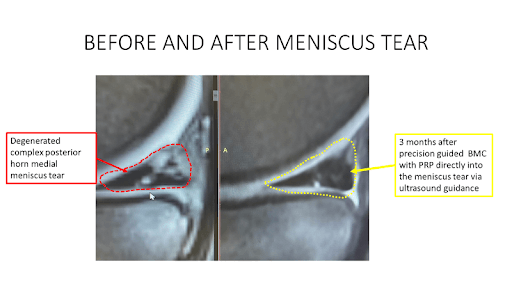
Tear Locations
On an MRI (or to some degree with an ultrasound), you can determine where the meniscus is torn. It’s crucial to decide on the location of the tear as it confirms the diagnosis and dictates the treatment.
Here are the possible tear locations as seen on imaging that correlate with the site of the knee pain:
- Anterior horn tears: the front part of the meniscus is torn
- Body tears: tears in the mid portion of the meniscus
- Posterior horn tears: tears in the back part of the meniscus
- Root tears: tears in the front or back deeper part wear the meniscus attaches to the tibia
Symptoms Of A Torn Meniscus
The following are some of the symptoms a person may experience when they have a torn meniscus:
Anterior Lateral Knee Pain
The knee joint is one of the most complex joints of the human body. The femur, the tibia, patella, and fibula all contribute to this joint. They are held together by a myriad of strong ligaments that stabilize and support the joint. Anterior lateral knee pain is pain that occurs in the anterior and the anterior lateral region of the knee joint. A person may experience this pain front and center, in the outer aspect of the knee, or diffusely throughout the joint. The cause of the pain is some pathology in the anterior and lateral aspect of the knee.
Read More About Anterior Lateral Knee PainBack of Knee Swollen
Back of knee swollen? Swelling in the back of the knee is not something that is talked about too often. It can be uncomfortable or sometimes painful with the movement of the knee or, even with rest. It often stems from an orthopedic-related issue or, perhaps some other medical condition. Let’s dive in…What’s Causes Swelling in the Back of Your Knee? The back of the knee contains a variety of anatomical structures that can be affected and result in pain, swelling, numbness, tingling, etc. Muscles and tendons behind the knee that could be the source of pain or pathology could be one or more of the following: Gastrocnemius, Soleus…
Read More About Back of Knee SwollenBack of Knee Tight
Stiffness in the back of the knee can be a sign that there is damage or inflammation in the joint, arthritis, or a baker cyst. This might be due to an injury, overuse, or medical condition. If you are experiencing stiffness in your back knee, it is important to see a doctor determine the cause and get treatment. Common causes of stiffness in the back of the knee include: tight muscles, tendons, and ligaments, Injury to the joint or surrounding tissue, overuse such as from running or biking for long periods. Stiffness at night can potentially indicate damage to the joint…
Read More About Back of Knee TightBurning Pain on Outside of Knee When Kneeling
There are many possible causes of burning pain on the outside of the knee while kneeling. One possibility is that you may have patellofemoral syndrome, which is a condition that results in pain around the kneecap. This pain can be aggravated by activities such as kneeling or squatting. Other potential causes of this type of pain include iliotibial band syndrome, runners knee, and meniscal tears. If you are experiencing burning pain on the outside of your knee while kneeling, it is important to see a doctor for evaluation. Some of these conditions can be treated with conservative measures such as rest, ice, and physical therapy…
Read More About Burning Pain on Outside of Knee When KneelingCan’t Straighten Knee
Your knee is capable of moving in a number of directions. The most common are flexion and extension. Flexion is when you bend your knee and the shin bone moves towards the buttock. Knee extension is when you straighten out your knee. The extension is the opposite of flexion. PT, trainers, and physicians alike measure the degree of knee flexion and extension. When lying flat on an examination table or hard surface your knee should be able to extend so that there is no angle between the thigh and shin bone. The inability to straighten the knee is also known as an extension lag and is a reason for concern.
Read More About Can’t Straighten KneeKnee Buckling
Knees can buckle, causing a sensation of one or both knees giving out that affects nearly 17% of adults. The knees are regarded to be one of the most essential (and biggest) joints in the human body because they play significant roles in basic activities such as walking and sitting. When our knees begin to feel unstable, weak, or begin giving out, it is easy to become stressed since we rely so heavily on them for movement. The knee can become stable from numerous types of injuries. The knee is kept stable by the following structures: Tendons attach the leg muscles…
Read More About Knee BucklingKnee Hurts When I Bend It and Straighten It
Your knees bend countless times throughout the day. Running up the stairs, down the hall after kids, and getting into the car. You straighten the knee as you walk, descend stairs or get into and out of the car. Bending and straightening the knee are necessary for daily activities. Knee pain with bending or straightening may be a mild, transient irritation or may indicate a more significant problem. Learn more below and avoid further injury and dysfunction. Knee pain can vary significantly depending upon many factors including the actual source of the pain, the severity of the injury, general health, and level of activity…
Read More About Knee Hurts When I Bend It and Straighten ItKnee Locking & Catching
Knees have the ability to bend forward and back, as well as rotate slightly. When a knee is unable to execute these actions, it impairs mobility and the capacity to complete daily chores such as sitting, standing, squatting, or kneeling. A locked knee occurs when a knee cannot be bent or straightened so it gets stuck or feels locked in a certain position for an extended period of time. There are two forms of locked knees: one that is due to inability to move because of an actually physical or mechanical restriction and there is one that feels locked due to the pain involved in moving it. When a person has their knee joint effectively frozen into place and cannot move, this is known as a true locked knee….
Read More About Knee Locking & CatchingKnee Pain
Knee pain can be caused by many factors. Overuse injuries, direct trauma to the knee and arthritis are the most common causes of knee pain. Damage to the knee structures may cause swelling, scar tissue formation (fibrosis), and loss of function of the joint. Pain is often accompanied by difficulty walking, weakness, and instability. When the knee is overused, the thigh and shin bones (femur and tibia), cartilage, or tendons may experience stress. This leads to pain and discomfort as well as stiffness in the knee. Overuse injuries are common among athletes who participate in sports that involve running, jumping…
Read More About Knee PainKnee Popping
Knee popping can be a sensation that something is moving around in the knee. There may also be an audible sound associated with the popping, which in medical terms is called crepitus. This can also cause what we call mechanical catching or locking, which may make the knee feel like it is stuck in an extended or flexed position, and you have to move it in certain ways to get out of that. This knee popping sensation or sound or could be a very simple issue or it could be a sign that more serious damage is going on in the knee, so determining what is causing it is very important. So, the knees may pop and get in a certain position….
Read More About Knee PoppingKnee Swelling
Swelling of the knee, also known as water on the knee, is a condition in which fluid collects around the knee joint. Swelling can occur for a variety of reasons and affect patients of any age. Some swelling can be treated with over-the-counter medicines, but persistent and continuous swelling might result in tissue damage, bone softening, and cartilage deterioration. Over-the-counter medicines will assist relieve pain for individuals with a history of osteoarthritis and swelling following physical activity, such as exercise or running. During and after activity, the patient may apply compression sleeves to reduce the inflammation. Ice is another method…
Read More About Knee SwellingOutside Knee Pain
What causes outside knee pain? How do you treat it? Let us go over all of this and also review how one patient avoided a huge surgery. What is On the Outside of the Knee? You have a couple of key structures here (1). They include the: Lateral meniscus, Lateral joint compartment, Popliteus tendon, Iliotibial band, Lateral collateral ligament , and anterolateral ligament, and Fibula. The meniscus is a figure-8 shaped fibrous structure (shown here from above) that is a shock absorber for the knee joint. It has an outside part (lateral meniscus) that cushions the joint. The meniscus can become torn or degenerated. If you are young…
Read More About Outside Knee PainPain Behind Knee
First off, this is where the hamstrings and calf muscles attach. They have tendons here that are inserted into the bone. So if there’s a problem in the muscle or the tendon, you’re going to feel it right here. This is also where deep muscles like the popliteus and plantaris live. So, if these have issues, you’re going to feel it in the back of the knee. In addition, the tibial nerve is back here. So if there’s an issue with a nerve in your back or a nerve locally, behind the knee, you’re going to feel it here. And the meniscus or the joint spacer lives back here. And the meniscus or the joint spacer lives back here. So a tear in the meniscus could cause pain…
Read More About Pain Behind KneeReduced Range of Motion in Knees
A knee can feel stiff if there is some swelling in or around the joint or muscle tightness can caused restricted motion This can occur from a problem in the knee joint, such as inflammation, arthritis, or infection, or an injury. The distance and direction that a joint may move are referred to as its range of motion. Various joints in the human body have specific normal ranges set by doctors and therpists. One study, for example, found that a normal knee should be able to bend to between 133 and 153 degrees. A typical knee should also be able to extend fully straight. Limitation of motion occurs when a person range of motion in any limb is reduced below the normal range….
Read More About Reduced Range of Motion in KneesTightness in Knee
What could tightness in your knee mean? When fluid builds up inside the knee as a result of an injury, overuse, or medical problem, the knees become swollen and tight. Swelling might be mild, so you may not always notice it unless it is serious damage. You may feel this as stiffness in the knee since swelling may not be visible. Swelling restricts movement since there is less room in the knee. Fluid buildup can be caused by irritation, internal bleeding, and injuries to the knee. Arthritis, gout, tumors, and baker cysts are all causes of swelling. Pain and swelling are the responses of your body to damage. Together they can lead to stiffness in your knee…
Read More About Tightness in KneeWeak in Knees
Weakness in the knee can be a symptom of many different knee conditions. Some of the most common causes of weakness in the knee include ligament tears, meniscus tears, and arthritis. Another important but often overlooked cause of knee weakness is irritation or injury of the nerves in the low back. If you are experiencing any type of weakness in your knee for long durations of time (3 weeks), it is important to see a doctor to determine the cause. Some of the most common symptoms of knee weakness include difficulty standing up from a seated position, difficulty walking, climbing or descending stairs…
Read More About Weak in KneesCommon Causes Of A Torn Meniscus
Here are some causes of a torn meniscus:
Forced Knee Twist
A forced twisting of the knee is a common cause of a meniscus tear. This can occur during any of the following:
- Occupations involving kneeling and squatting
- Sports with rapid acceleration, deceleration, or sudden changes in direction like rugby, football, basketball, baseball, skiing, and wrestling
- Infantry duties like mounting and dismounting, marching for several hours with a heavy weight, or crawling and kneeling in rough terrain
Aging
As people age, the knee cartilage loses water and becomes stiffer, leading to a degeneration of the menisci. The degenerative changes make the menisci more susceptible to tears and shearing. Horizontal tears are common in men over 40 due to the degeneration of the fibers that run parallel to the tibial plateau (2).
Risk Factors For A Torn Meniscus
The meniscus can be torn during sport, high-intensity exercise, or trauma. Risk factors include low physical activity levels, high of intensity exercise, poor form, incorrect biomechanics, and being overweight.
Additionally, movements like twisting the knee, deep knee flexion, and rotating the knee can predispose to injury. The biggest risk is having an unstable knee! Which is critical to understand, when treating a meniscus tear, also need to address the underlying instability of the knee, of the tear and/or symptoms are more likely to return!
Preventive Steps To Protect Yourself From A Meniscal Tear
While you cannot avoid aging, there are some basic steps that you can take to protect yourself from a meniscal tear. Some helpful preventative tips are listed below:
- Keep the muscles strong: It’s important to build up the knee muscles to prevent the knee joint and menisci from overloading. You can achieve this with resistance and endurance exercises. Larger and stronger muscles can absorb shock better and transmit the load more equally across the knee joint.
- Always warm up: Warming up the body before exercise increases the blood supply to the knee joint. This increases the oxygen and nutrient supply, preparing the body before any demand is placed on the knees during activity and movement.
- Rest between workouts: It’s important to rest In between workouts or intense activity. Rest allows the muscles and tissues to replete their nutrients and oxygen levels. This will also repair micro-injuries and tears.
- Wear properly fitted shoes: Wearing the right footwear is important to protect against knee injuries. Many work out with the wrong shoes or wear high-heeled shoes for prolonged periods. This puts undue strain on the calves and knees.
As a result, the knees cannot properly transmit forces and load across the calves and ankles. This shearing force can return to the knee, causing an injury to the knee or a meniscal tear. - Maintain flexibility: Keep yourself flexible with exercises like stretching or tai-chi. This will help prevent degeneration of the muscles, bones, and tissues around the knee joint which can stave off age-related meniscus injuries.
- Train progressively: As you work out, build your regimen incrementally with progressive increases in weights, inclines, and distances. Sudden increases in exercise or workouts can lead to knee injuries as it may put more load on the joint than it is accustomed to.
Examining And Diagnosing A Meniscus Tear
Here are how doctors examine and diagnose a meniscus tear:
- Physical examination: The doctor will check your knee for pain, especially over the anteromedial and anterolateral joint line. They will also look for signs of locking, popping, clicking, catching, an inability to fully straighten the knee, or buckling, which may be present depending on the type and extent of the meniscal tear.
A close examination for edema, palpation of the joint line, standing and supine range of motion (ROM), and muscle strength will also be evaluated. - Special tests: Certain tests are done to provoke the knee and assess which structures are affected. For example, tests such as the Thessaly test, McMurray’s test, or Apley’s test.
For the Thessaly test, the patient stands on one leg. Then, the patient squats down to 20 degrees of knee flexion while rotating the knee with the hip abducted (the leg away from the body) and then adducted (the leg towards the center of the body). The test is positive if it provokes pain.
To perform McMurray’s test, the doctor passively extends the knee while the patient is supine from a fully flexed position to 90 degrees flexion while fully rotating it. The test is positive if there is pain.
For Apley’s compression test, the patient starts in a prone position. The doctor passively flexes the knee to 90 degrees and then rotates it with axial compressive force.
Any pain reproduced during these tests indicates a problem with the meniscus. These tests have varying degrees of specificity and are usually used in conjunction with imaging. - Imaging: When doctors suspect a meniscal tear, imaging is recommended. Various X-ray views, including in weight-bearing, are done to assess for bone pathology, loose bodies, and osteoarthritis.
However, MRI is the best test to diagnose a meniscal tear as it is the most sensitive imaging modality. The gold standard test for diagnosing a meniscal tear is arthroscopy as doctors can directly visualize the tear. This is done when surgical intervention is also being planned to treat the tear.
Common Treatments For A Torn Meniscus
The treatment for a torn meniscus depends on the cause and the severity of the tear. Some of the common therapies for a torn meniscus are explained in detail below:
Rest
Rest is part of the R.I.C.E treatment (rest, ice, compression, elevation). The goal is to cease the aggravating activity, whether kneeling, squatting, jumping, or playing a sport. Rest helps control the pain or swelling and begins the healing process.
Ice
Icing the knee with cold compresses and ice packs will help reduce inflammation and swelling in the knee joint. This is a helpful initial treatment for mild tears and injuries to provide symptomatic relief. You can ice the knee for 10 minutes at 20-minute intervals several times a day.
Compression
Compression of the knee using a brace can help reduce the swelling and direct the excess fluid to be absorbed within the joint. This is a good initial treatment for mild injuries with slight pain and swelling.
Elevation
Elevating the knee can help reduce any effusion or bleeding in the joint. This reduces the pressure on the injured meniscus and allows it to heal. Additionally, by keeping the knee elevated, it prevents any activity or motion so the knee can rest.
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
NSAIDs are a type of pain-relieving medication. They reduce pain and inflammation at the site of the tear by blocking the enzymes in the inflammatory pathway. As a result, NSAIDs, such as celecoxib and ibuprofen, can provide moderate pain relief.
Surgical Treatments
Surgery may be recommended for severe meniscal tears, mainly when other conservative treatments have been unsuccessful. Some of the different types of surgeries used to treat a meniscal tear are explained below:
Partial Meniscectomy
Arthroscopic partial meniscectomy – meaning partial removal of the meniscus – is not the first-line treatment for a meniscal tear.
It is usually only used for patients with mechanical symptoms like clicking, locking, and an inability to straighten the knee. It may also be recommended when other conservative measures have failed, such as RICE (rest, ice, compression, elevation), and pain medications. A partial meniscectomy may also be used if the symptoms persist for more than six months.
Meniscus Repair
In a meniscus repair, the surgeon sutures the torn cartilage. The body reabsorbs these sutures over time. Meniscus repairs are done for smaller tears via an arthroscopic procedure.
Repair is preferred over meniscectomy (removal of the meniscus) as even partial removal of the meniscus can lead to an accelerated risk of osteoarthritis. Larger tears are treated with open meniscus repair or meniscectomy.
Regenexx Procedures
Regenexx procedures are newer therapies that use regenerative techniques. This can include platelet-rich plasma (PRP) for knee conditions and other cellular therapies such as bone marrow concentrate. These therapies use plasma and stem cells taken from the individual and processed.
These cells are then reintroduced into the cartilage with growth factors to boost healing. With the right nutrients, the cartilage and damaged tissue can repair and recover using the body’s healing mechanisms.
Recovering From A Meniscus Tear
It is possible to return to peak performance after a meniscus tear. However, irrespective of the type of treatment (medical or surgical), you will need a rehabilitation program. The goal of the treatment from the very beginning is to achieve quadricep control. This is achieved by following a tailored rehab program.
Depending on the surgery, the rehab program may include knee flexion and weight-bearing restrictions for the first six weeks after the surgery. It will also vary based on the type of tear and the type of repair.
Some medical rehab teams will use cryotherapy, while others will use aquatic therapy to help rebuild the knee during the rehab program. The rehab protocol can vary and what it includes will vary based on the tear and what will be incorporated into the protocol as each person is different and will progress at a different pace.
On average, it can take 8 to 22 weeks to recover from meniscal tear surgery and a few more months to return to competitive sport or athletic performance. Until the person can fully contract the muscles supporting the knee without pain, crutches are prescribed.
This is also to prevent any weight-bearing until there is complete healing of the tear. Once normal gait is achieved, neuromuscular training and other unilateral exercises can begin.
A Torn Meniscus Is Common But Treatable
If you suspect you have a torn meniscus, the first step is to be examined by a board-certified orthopedic doctor. They may confirm the diagnosis with a history, physical examination, and imaging.
The diagnostic tests will also determine the best treatment for your torn meniscus, which may include newer therapies like regenerative medicine. If you have a torn meniscus, contact us today to consult with one of our doctors.
Are you a Candidate?

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreOther Resources for Meniscus Tears
Free Download: The Knee Owner’s Manual

This e-book by Dr. Chris Centeno examines the knee and its role in the human musculoskeletal system and the body as a whole. The Knee Owner’s Manual provides a series of tests and clearly defined exercises that you can perform on your own to assess and monitor your own knee health. It will allow you to look for trouble spots where your own body may be having difficulty with stability, articulation, symmetry, and neuromuscular function. You’ll be able to see how these deficits in other regions of the body relate to the knee.
The Knee Owner’s Manual also discusses how Regenexx is pioneering the development of interventional orthopedics, a new branch of medicine that employs regenerative biologic therapies such as adult bone marrow concentrate and platelet-rich plasma to help repair and strengthen damaged tissues in other areas of the body.
This is contrasted with invasive knee surgeries, which often remove important tissues or replace the entire knee itself when it becomes damaged. With hyperlinks to more detailed information, related studies, and commentary, this book condenses a vast amount of data, images, and resources into an enjoyable and informative read. This is the first edition of The Knee Owner’s Manual, a companion book to Orthopedics 2.0.
-
Partial ACL Tear
A partial ACL (anterior cruciate ligament) tear occurs when the ligament in the knee is partially damaged, often leading to instability, pain, and limited range of motion. This injury typically results from sudden stops, pivots, or direct impacts, commonly seen in athletes. Early diagnosis and appropriate management are crucial to preventing further damage and ensuring…
-
Degenerating Meniscus
Degenerating meniscus is a common issue, particularly in aging populations, that can lead to significant knee pain and impaired mobility. This condition often arises from wear and tear over time, resulting in the breakdown of the meniscal cartilage, which is crucial in cushioning and stabilizing the knee joint. Early detection and appropriate management are key…
-
What Is Golfer’s Knee, And What Can I Do About It?
The nature of golf is such that both the backswing and downswing affect the knee. The entire swing takes a little over one second. However, it can exert a force of 4 times the body weight on the front knee and 3 times the weight on the back knee (1). This makes knee injuries just as…
-
Knee Pain Location Chart: What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
Understanding Knee Pain Symptoms To Get The Best Treatments
Knee pain affects about 25% of the population (1). The knee joint involves three bones, namely the patella, the femur, and the tibia. Knee pain can be a sign of damage to the ligaments, bones, bursae, or muscle tendons because there are so many structures within the knee joint. In this post, we’ll discuss the…
-
6 Meniscus Tear Types And How To Treat Them Properly
Even a small meniscus tear can make walking difficult for you. If you are experiencing any of these symptoms, you may want to seek medical help as soon as possible, depending on the type of tear you have. Needless to say, a lot depends on understanding the meniscus tear types there are and what each…
References
- Zhang K, Li L, Yang L, et al. Effect of degenerative and radial tears of the meniscus and resultant meniscectomy on the knee joint: a finite element analysis. J Orthop Translat. 2019;18:20-31. Published 2019 Jan 21. doi:10.1016/j.jot.2018.12.004
- Raj MA, Bubnis MA. Knee Meniscal Tears. [Updated 2022 Jul 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK431067/