Pain In The Back Of The Heel
Get Help With Pain In The Back Of The HeelHeel pain can be intense and, despite rest and trying a variety of other conservative measures, it can often also be persistent.
Every year, there are over a million visits to primary physicians for plantar heel pain (1). Plantar heel pain affects both men and women equally, and there are many causes of plantar heel pain.
Therefore, it is important to diagnose the cause of the heel pain so that it can be treated appropriately. We will review the causes, complications, and treatment options for plantar heel pain.
Where Does Heel Pain Originate?
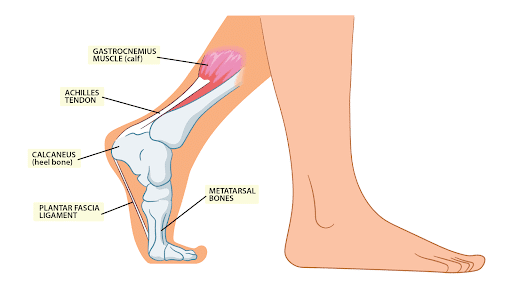
The heel comprises three main structures: the Achilles tendon, which inserts into the bone, the heel bone (or “calcaneus”), and the plantar fascia.
The Achilles Tendon
The Achilles tendon is the fibrous connective tissue that continues from the calf and the soleus muscles. It is attached to the calcaneus bone in the foot. It is the largest tendon of the human body and any injury to the Achilles tendon can lead to heel pain.
The Heel Bone
The calcaneus, also known as the heel bone, is the largest bone of all the tarsal (foot) bones. It lies close to the cuboid and the talus bones of the foot, forming the hindfoot. Conditions such as fractures of the calcaneus, arthritis, and hairline stress fractures can cause severe heel pain.
The Plantar Fascia
The plantar fascia is the connective tissue that connects the calcaneus or heel bone to the toes. It runs along the base of the foot so any inflammation or excessive wear of the plantar fascia because of repetitive stress can lead to heel pain.
Nerves
The local nerves such as the tibial, sural, or Baxter’s nerves can become compressed or inflamed causing heel and foot pain.
Symptoms Associated With Heel Injury
If you have an injury or problem with the heel, then here are some common symptoms you will experience:
Stabbing Heel Pain
Stabbing heel pain is very characteristic of an injury or inflammation to any of the structures in the heel, whether the Achilles tendon, heel bone, or plantar fascia. Stabbing heel pain usually increases with movement and may or may not be relieved with rest.
Pain While Walking On Your Tiptoes
Walking on your tiptoes is a movement called plantarflexion and requires activation of your calf muscles and therefore also the Achilles tendon. Any injury or inflammation of the calcaneus or the Achilles tendon will cause pain during toe walking.
Warm Skin Over The Calcaneus
Warm skin over the calcaneus is a sign of inflammation. When this occurs, the skin over the calcaneus will be red, warm, and tender to the touch. This may or may not be accompanied by swelling. The affected area is warmer than the rest of the foot.
Swelling
Swelling is another sign of inflammation, but can also accompany fractures of the heel bone. If there is persistent swelling, despite icing the heel bone, your physician should look at it. Swelling in the foot can occur because of injury to the muscle, bone or supporting ligaments.
Tingling And Burning Pain
The presence of tingling, decreased sensation, or burning pain in the heel can suggest some sort of nerve entrapment or nerve injury. This is frequently seen in conditions such as neuritis and tibial tarsal syndrome.
Heel And Back Pain Are Often Connected
The backbone may not be directly connected to the heel—however, like with everything in the body, it is connected by the nerve supply.
The structures that make up the heel contain nerve branches that originate in the lower back. This nerve branch handles both sending and receiving signals between the foot and the spine.
This nervous system wiring is, in fact, one massive network. The lumbar spinal nerves are numbered from L1 TO L5 and the sacral spinal nerves are numbered from S1 to S5.
If our S1 nerve becomes irritated in the lower back, it can cause back pain and pain in the heel, too. Injury or disease of the lower spine can affect any structure down the leg–the hip, knee, ankle, heel, and so on.
Interestingly, when a nerve is irritated in the back, there may not always be pain in the back. Sometimes, the only warning sign you may have is heel pain, with symptoms similar to plantar fasciitis, that just won’t subside. Therefore, it’s so critical to have your back checked when you have heel pain.
The longer you wait, the more difficult it can be to treat. Ignoring your heel pain could lead to not only chronic back problems but also Achilles tendon or calf muscle tears. Treating a small issue is much easier than cleaning up the mess of a much bigger issue..
Besides heel pain, the irritated nerves in your back can cause chronically tight or twitching calf muscles, wreaking havoc on your plantar fascia (the broad connective band of tissue that lines the sole) over time.
Common Causes Of Heel Pain
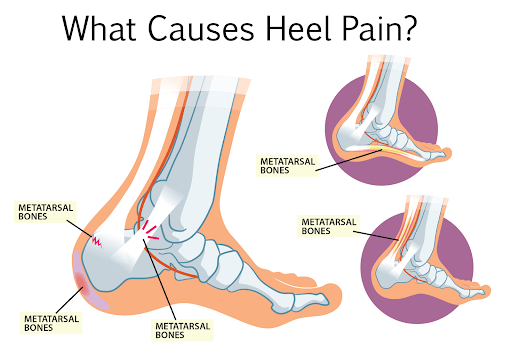
Now that you know the anatomy of the hindfoot, it is easier to understand the causes of heel pain. We list the most common causes below:
Plantar Fasciitis
Your heel pain initially was mild and aching. It is now a constant forest fire at the base of your heel. Each morning you take your first step with great trepidation knowing that the searing pain is literally a step away. Medications, rest, and physical therapy have not helped. Your doctor is concerned and thinks you may have Plantar Fasciitis. What is Plantar Fasciitis? What are the symptoms of Plantar Fasciitis? What are the risk factors? Is Plantar Fasciitis simply inflammation? What are the treatment options for Plantar Fasciitis? What to do for Plantar Fasciitis so bad I can’t walk? Beware as not all heel pain is Plantar Fasciitis.
Read More About Plantar FasciitisPlantar Plate Tear
The plantar plate is a fibrocartilage structure located at the ball of the foot. The ball of the foot involves a joint which anatomically is called the metatarsal phalangeal joint (MTP) joint. The MTP joint is where the long foot bone (metatarsal) meets the toe (phalanx). Each toe in the foot has an MTP joint which is numbered 1 through 5. The plantar plate allows the foot to absorb the enormous forces of walking and running in addition to limiting extension (1). There are ligaments that attach the plantar plate to the long bones of the foot which are illustrated by the red and blue bands in the picture. The plantar plate and the supporting ligament provide critical stability for the MTP joint.
Read More About Plantar Plate TearAchilles Tendonitis
Heel pain is one of those issues that can affect most of what you do in a day and can be disabling. A common cause of heel pain is the Achilles tendon. What is the Achilles tendon? What is Achilles tendonitis? What are the different injuries? Is stem cell therapy for Achilles tendonitis a viable option? Where & What Is the Achilles Tendon? A tendon is a thick fibrous band of connective tissue that connects a muscle to bone. There are more than 30 million tendon and ligament injuries annually. The Achilles tendon, which is the thickest tendon in the body connects the calf muscles to the heel bone. It consists of the gastrocnemius and soleus muscles that unite to form a thick band that is immediately above the heel tab on your shoe. It enables the downward movement of the foot and bending of the knee.
Read More About Achilles TendonitisPlantar Fasciitis
Plantar fasciitis affects about two million Americans per year. The plantar fascia has a central, medial, and lateral side. The medial portion is the most vulnerable as it supports the longitudinal arch of the foot. It is attached to the medial tuberosity of the calcaneus. If the mechanical load on the foot increases, this medial portion elongates.
Standing for long hours, flat feet, soleus-gastrocnemius complex dysfunction, increased body weight, and instability of the ankle can put more load on the fascia. Additionally, as you grow older, the elasticity of the plantar fascia decreases, which can further stress the area. The cumulative effect of all these conditions is degeneration of the plantar fascia.
Patients with plantar fasciitis complain of heel pain when they take their first steps in the morning after waking up. They also complain of heel pain when they stand after sitting down for hours. In cases of chronic plantar fasciitis, pain persists at rest and during activity.
On examination, there is tenderness inferiorly over the medial calcaneal tubercle which is at the beginning of the arch along the base of the foot. The plantar fasciitis overlaps the calcaneus, so when you examine it, there is tenderness over the tubercle and a sure sign of plantar fasciitis.
Achilles Tendinitis
Achilles tendinitis is an injury caused by overuse of the Achilles tendon. It is commonly seen in runners who are constantly training or increasing the intensity of their workout. When you increase the duration and intensity of running, the tendon fibers respond to this increased load. However, without sufficient recovery, the fibers can become inflamed.
To avoid this, it’s important to escalate running intensity and also rest long enough to allow the fibers to repair and recover before another intense running period.
This inflammation generates edema which is rich in inflammatory cells. Fibrin exudate, which causes crepitus and limits the movement of the tendon with the sheath, follows this inflammation. One of the first signs of this inflammatory process is heel pain.
Bursitis
Inflammation of the heel bursa can cause heel pain. Bursae are small fluid-filled sacs that cushion the joints of the body. There are only two bursae in the heel, namely the retro calcaneal and calcaneal bursa.
Heel bursitis can occur when someone awkwardly lands on their heels, or lands too hard, and also prolonged standing or even because of wearing the wrong footwear for too long. Heel pain from bursitis is characteristic in how it is felt deep inside the heel and gets worse as the day progresses.
Other Less Common Causes Of Heel Pain
Apart from the more common causes of heel pain, there are many other conditions that can also cause heel pain, or cause referred pain in the heel. Referred pain is when pain is perceived at another site instead of the location of the injury itself because of the common nerve supply.
We list these conditions below:
Bone Spurs In The Heel
Heel spurs also cause heel pain. Long-term stress on the plantar fascia, because of prolonged standing, obesity, and repetitive activity, can lead to the formation of heel spurs where the plantar fascia attaches to the calcaneus bone.
These spurs are abnormal bone growths in response to repeated stress on that area of the bone. They occur as a reaction to constant plantar fasciitis. Studies show that 82% of those who have bone spurs in the heel are overweight (2).
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is an entrapment syndrome where the structures within the tarsal tunnel are compressed. The tarsal tunnel is formed by the bone of the ankle and the ligaments that stretch across the foot.
It contains the tendons of the posterior tibialis, flexor digitorum longus, and flexor hallucis longus muscles, the posterior tibial artery and vein, and the posterior tibial nerve. This tunnel can be compressed because of trauma, gout, lipoma, ganglion cyst, arthritis, neuroma, and ankle sprains.
Compression of the posterior tibial nerve within the tarsal tunnel can give rise to burning pain in the foot, tingling, and numbness. Often people experience a sharp, shooting pain in the foot because of this nerve being compressed.
Additionally, any vascular occlusion that can affect the posterior tibial artery can lead to a reduced blood supply to the nerve, which will lead to neuropathic pain in the heel. Tarsal tunnel syndrome can occur because of any structure within the tunnel being injured or trapped, be it nerve, artery or tendon.
Calcaneal Stress Fractures
A calcaneal stress fracture is a small hairline fracture in the calcaneus bone. In a 4-year study of U.S. soldiers, calcaneal stress fractures accounted for about 20% of the lower extremity fractures (3). These fractures are also seen in new runners, the sudden increase in intensity and duration of standing or running, overweight individuals, and those with rheumatoid arthritis.
The abnormal stresses of these activities can result in hairline fractures of the calcaneus bone. Without adequate time to rest, the area does not have time to recover and remodel the bone, which can lead to heel pain.
Heel Pad Bruise
A heel pad bruise, commonly referred to as a police officer’s heel, can occur because of acute injury or trauma to the fat pad that protects your heel, such as repeated jumping or falling from a height. In these cases, it’s not just the muscles that are injured, but also the blood vessels. This type of heel pain is usually accompanied by redness and swelling of the heel pad.
People with a heel pad bruise experience pain in the back of the heel with redness with no swelling as well. The breakage of the vessels causes blood to extrude into the muscle fibers, giving it its characteristic appearance of the bruise.
Heel Pad Syndrome
Heel pad syndrome occurs when the fat pad protecting the heel gradually thins out. The heel pad is made of fatty tissue and thick elastic connective tissue. It functions as shock absorbers and cushions the heel during activities like jumping and running.
Over time, the heel fat pad can atrophy due to wear and tear, age, starvation, cancer cachexia, and prolonged high-impact activities like gymnastics and basketball. In some people, repeated jumping, as seen in athletes, can flatten the fat pad, displace it sideways, or cause degeneration over time.
People with heel pad atrophy experience diffuse central plantar heel pain. This is exacerbated by walking barefoot on a firm surface. While examining the foot, it’s common to find tenderness on the central part of the calcaneus.
Haglund’s Syndrome
Haglund’s syndrome is a syndrome with multiple abnormalities and includes the inflammation of the retro calcaneal bursa and Achilles tendon, and a bony prominence of the calcaneus bone. Each of these conditions can occur in isolation.
Haglund’s syndrome can be hard to diagnose, but imaging techniques including ultrasound can be extremely helpful to identify each of the conditions of this syndrome outlined above. An ultrasound will catch inflammation of the bursae and tendons, as well as inflammation round the bone. An Xray can show a large bony protuberance.
Patients often present with a visible bump at the back of the heel, swelling, and redness near the inflamed tissue, along with heel pain at the site of the attachment of the Achilles tendon to the heel bone.
Sever’s Disease
Sever’s disease, otherwise known as calcaneal apophysitis, is a common cause of heel pain in the pediatric population. It is inflammation and pain around the heel growth plate. It is commonly seen between the ages of 8 and 15 in children who are overweight or those who have extremely high levels of physical activity.
Children involved in high-impact sports like ballet, soccer, track, and field sports, cross-country, gymnastics, and tennis are prone to Sever’s disease.
The onset of symptoms is usually very gradual, and the heel pain is relieved by rest. There may also be pain where the tendon Achilles tendon is attached to the bone.
Is Heel Pain Serious?
Heel pain can resolve on its own, however, the pain can get worse if left untreated. Disregarding heel pain can also affect the tendons, ligaments, your movements, and range of motion. Therefore, it’s important not to ignore heel pain.
- One effect of chronic heel pain is altered movement. The first thing that will change is your gait. To get around the pain, you might walk differently. An altered gait may then affect your knees, hips, and spine because of the unnatural movements.
- The heel pain can also make you more sedentary, which can further weaken the muscles that support the lower leg and foot.
- Heel pain that occurs because of inflammatory conditions can permanently affect your joints, bones, and tendons. Inflammatory conditions, if left uncontrolled, can further wear out the joints in the foot like the talocalcaneonavicular joint, calcaneocuboid joint, and the cuneonavicular joint because of their exposure to inflammatory chemicals and proteins.
These chemicals and proteins break down healthy tissue so you cannot ignore heel pain because of inflammatory disease. - Heel pain can also be a sign of a hairline fracture in the calcaneal bone and so you should not ignore it without getting your heels examined by a doctor.
Risk Factors Of Heel Pain
Certain people are more prone to heel pain. Common risk factors of heel pain are:
- Age: The older you get, the more likely you are to develop heel pain. This is because the pads under your heel wear with age. These pads act as shock absorbers when you walk and run.
However, with increased wear of the heel pads, these pads are less able to absorb shock, which can lead to heel pain. The plantar fascia also loses elasticity over the years, and this can cause heel pain. - Activity: Athletes are prone to heel pain because of all the stress of their exercise and activity. Repetitive movements, like in sports such as ballet dancing, that strain the muscles, ligaments, and bones of the foot can cause ankle pain.
Tissue damage in the foot is also observed in those athletes who have higher pronation of the foot and improper flexion of the muscles, which can lead to heel pain. Improper flexion is common in sports where there are sudden changes in the speed, intensity or activity of the muscles.
Higher pronation is commonly observed in gymnastics and long-distance runners. - Weight: Increased body weight has been associated with an increased risk of heel pain. This is because the extra pounds put additional stress on the heel.
- Chronic Conditions: Inflammatory conditions like osteoarthritis, rheumatoid arthritis, and psoriatic arthritis can cause inflammation of the joints and lead to heel pain, especially during flare-ups. Flat feet can also predispose you to heel pain. Pes planus is a deformity that occurs from birth.
It is a chronic condition where a person has little to no arch. Heel pain occurs in this condition because the muscles and ligaments connecting the feet are strained, particularly if the ankles turn inward. In the absence of proper arch support, the ligaments can face extra stress during walking and running. - Footwear: If you wear footwear that strains the ankles and calves like high-heeled shoes for extended periods, the chances of developing heel pain are much higher. This is because the ultra-narrow heel concentrates the weight on one small area of the heel rather than the whole heel.
Five Ways To Ease The Pain At Home
How soon will you see pain relief? It depends on the cause. For those who have heel pain because of repetitive movements or stress from exercise, simply abstaining from that activity could help to relieve the heel pain. For others, it may not be so simple.
If you have heel pain, you can try conservative therapy first and see if that helps. In most cases, heel pain resolves on its own or after supportive treatment that you can do yourself. Here are some ways you can ease the pain in your heel at home:
- Rest: If your heel pain is because of sports or an exercise regimen, like running or brisk walking, then take a break. A period of rest will reduce inflammation and allow the heel to heal. Try to keep your weight off the affected foot during this time and change your training program so that the heel has time to rest and recover.
- Ice: When you have an injury to the heel or an ankle sprain, the first thing you can do is apply ice packs to your heel. Use ice wrapped in a towel if you do not have an ice pack. This will constrict the blood vessels and prevent swelling of the foot. You can ice the heel several times a day as needed.
- Well-heeled shoes: Use well-heeled shoes that support your arch. Heel pain is worsened by the wrong footwear. If you spend long hours standing, wear shoes that maintain the natural arch and shape of the foot. They should be comfortable and should support your calves as well. High-heeled shoes and uncomfortable shoes affect your balance, posture, and your feet, as they do not distribute your weight evenly.
- Foot supports: There are many types of foot supports. Arch support sleeves, toe spreaders, bunion correctors, toe guards, arch support cushions, silicone heel cushions, gel insoles, and heel pads are all available to relieve heel pain. You can choose any one of them depending on what is causing your heel pain.
Or you can ask your podiatrist to recommend what’s best for you. Heel inserts can also decrease the plantar calcaneal pitch angle and shift the bony calcaneal projection away from the soft tissues in the area.
This can help reduce the friction and lessen any heel pain with Haglund syndrome and bony spurs. Conversely, heel cups are commonly used to treat Sever’s disease. - OTC Medications: Over the counter (OTC) medications like ibuprofen and naproxen can relieve heel pain and reduce inflammation. These medications can be taken twice or thrice a day initially to relieve your heel pain. However, they do not treat the cause of heel pain.
- Plantar fascia splint: a splint to stretch the foot and ankle can help with plantar fasciitis.
When To Visit Your Healthcare Provider
Conservative treatment with rest, ice, and over-the-counter medications for the pain might help you for a while. However, if symptoms worsen or persist even with all the self-care, then you may need to get your heel examined. Here are some signs that should prompt you to seek medical treatment:
- Heel pain that does not improve after a few days
- Pain that worsens despite OTC medications
- Heel pain that is accompanied by swelling
- Numbness in the heel or any part of the foot
- Tingling in the heel
- Fever or chills
- Change in gait
- An inability to flex the foot upwards or downwards
- An inability to rise on the toes
- An inability to bear weight on the affected foot
Get A Solid Diagnosis!
After you meet with your doctor, he or she will do the required tests and diagnose you. You need to have a diagnosis so that you are treated appropriately. Here are some things to avoid while you are waiting for a diagnosis (or if the diagnosis is unclear):
Avoid Unnecessary Surgery
Your goal in treating your heel pain should be to first use conservative treatment and only use surgery once you have exhausted conservative management options. One of those is a brutal surgery: the gastrocnemius recession. Read more about it here.
Traditionally, this surgery is used for some deformities in the legs. However, in recent years, it has been performed as an elective orthopedic surgery for some conditions, such as plantar fasciitis, calf tightness, and heel pain.
The surgery involves cutting the calf muscle to force it to lengthen. But as with any surgery that attempts to rearrange the body’s biomechanics, it is a bad idea in most cases.
Avoid Unnecessary Steroids
Steroids should not be used where possible. Not only does the effect of steroids diminish with each subsequent injection, but steroids have also been associated with both cartilage and local stem cell destruction.
Treat The Root Cause Fast
Heel pain can be treated in a variety of ways, depending on the cause. It is important to find out what is causing your heel pain and have it treated right away. Studies suggest that treating heel pain early within six weeks of the development of symptoms will hasten recovery (3).
The longer you ignore the problem, the worse it will get. If you have heel pain, do not wait. Visit your doctor and find out what is causing your heel pain.
Ready to take your life back from heel pain?
References
- Allam AE, Chang KV. Plantar Heel Pain. [Updated 2022 Jun 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK499868/
- Moroney PJ, O’Neill BJ, Khan‐Bhambro K, et al. (2014) The conundrum of calcaneal spurs: do they matter? Foot Ankle Spec 7, 95–101.
- Buchbinder, R., 2004. Plantar fasciitis. New England Journal of Medicine, 350(21), pp.2159-2166.
