Shoulder Pain When Sleeping – 5 Causes To Know
Get Help With Shoulder Pain When SleepingNight after night, your shoulder pain awakens you. The pain is hot and searing and getting worse.
Why does your shoulder hurt at night? There are many causes of shoulder pain when sleeping. We’ll talk about all of them and how they occur. We will also look at the treatment options for shoulder pain when sleeping. Are there non-surgical treatment options? If so, where do you find them?
Let’s dig in.
How You Could Get Shoulder Pain From Sleeping
The shoulder involves the clavicle, scapula and humerus bones. Also, there are many shoulder muscles that attach to the humerus and scapula.
When we sleep, especially on one side, the joint is not in its shallow socket on the shoulder blade; it may be slightly out of position. The nerves can easily become impinged in this position and this can even cut off circulation to the joint, which further irritates it.
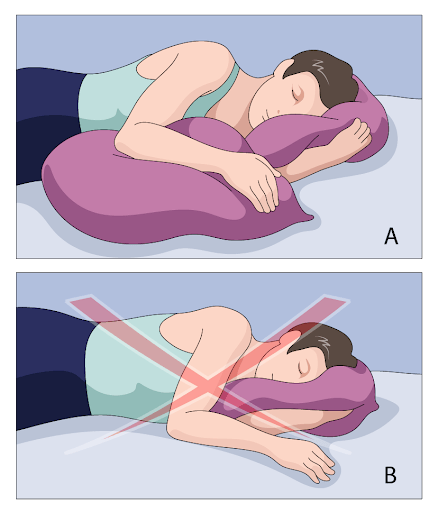
When people sleep, they tend to internally rotate their arm, which can worsen or aggravate shoulder pain. Instead, as shown in the image below, placing a throw pillow to support your forward shoulder can ease the rotation and maintain its normal position.
Types of Nighttime Shoulder Pain
These are the different types of shoulder pain we experience at night:
- Shoulder Sprain: This is caused by stretching the tendons and or ligaments in the shoulder. The pain is usually dull, aching, and limited to around the joint. If a tendon is sprained, it needs good blood supply to try to heal. Lying on the shoulder can constrict blood supply which can cause more pain in the tendon.
- Shoulder Irritation: This is usually due to impingement, bursitis, or tendonitis. The shoulder pain at night in this case is constant, may be accompanied by some swelling, and may also be of a burning type. In some cases, there may be tingling and numbness.
- Shoulder Nerve Injury: Injuries to the shoulder tend to cause shoulder pain that can radiate down the arm. It is persistent and may severely limit the movement of the joint.
Common Causes of Nighttime Shoulder Pain
Shoulder pain can occur at any part of the day. When it’s more pronounced in the morning, it’s often a sign of arthritis.
Some common causes of shoulder pain at night are discussed in detail below.
Poor Sleeping Position
There are several reasons why shoulder pain at night occurs or is aggravated. The common explanations include:
- Sleep typically involves a static position lasting hours at a time with little or no movement.
- Sleeping on your side places additional pressure on the tendons and bursa of the shoulder.
- Sleep can cause muscles and tendons to settle in a slightly different position resulting in additional pressure and reduced blood flow.
Frozen Shoulder
A frozen shoulder is usually due to chronic inflammation that causes the shoulder joint to stiffen. This causes pain but it is worse at night for a number of reasons. The first is that the joint capsule tightens up at night. This is a normal physiologic process. Any slight motion of the shoulder causes intense pain as it mobilizes the tight capsule.
Another reason for pain is the reduction of blood flow at night. When you sleep, the body slows down all its processes, including blood flow. This allows more edema and inflammation to persist, which worsens shoulder pain at night.
Rotator Cuff Injury
The rotator cuff is made of four muscles, namely the supraspinatus, infraspinatus, teres minor, and subscapularis. In a rotator cuff injury, one or more of the tendons of the rotator cuff muscles may be torn. Rotator cuff tears and injuries typically tend to be more painful at night. A tear leads to severe inflammation.
When you lie down, gravity stretches and pulls the tendons as well as the bursae, causing the pain from the inflammation to worsen at night.
Tendonitis
Tendons are thick bands of connective tissue that connect muscle to bone. There are several tendons around the shoulder including the four rotator cuff tendons, the biceps tendons, traps, coracobrachialis, the pec tendons, teres major, lats and more around the shoulder blade. They are susceptible to injury and can become inflamed, degenerated, or torn (1).
Tendonitis is a misnomer as most tendons do not get inflamed. Some tendons have a sheath like the long head of the biceps tendon and can have inflammation more appropriately named tenosynovitis. Most other tendons have more degeneration, tears, and abnormal thickening, more broadly termed tendinopathy which means “bad tendon.”
Common causes of shoulder tendonitis/tendinopathy include overuse, repetitive motion, trauma, poor blood flow, or prior surgery (2). Pain is the most frequent symptom which is aggravated by overhead activity. Shoulder pain at night is common with shoulder tendonitis.
Bursitis
A bursa is a fluid-filled sac that allows tendons, ligaments, and muscles to slide smoothly over bony surfaces. There are several bursae in the shoulder that can become inflamed and may be a source of shoulder pain at night (3).
The most common bursa in the shoulder that can become inflamed is the subacromial/subdeltoid bursa. Pain is typically aching in character and worsens with movement.
Some patients complain of a reduced range of motion. Bursitis is a common source of shoulder pain at night as pressure is applied to the bursae when lying on the affected side.
Osteoarthritis
The shoulder is a ball-socket joint. The joint is lined with cartilage which allows the two bones to easily move together. This allows you all the remarkable movements of the shoulder, such as throwing, grabbing, or lifting overhead.
Unfortunately, the cartilage can be damaged or eroded, leading to shoulder arthritis. Most commonly prolonged shoulder instability from ligament injuries, tendon injuries, and or muscle weaknesses or imbalances lead to excess stress on the joint cartilage.
Direct injury to the cartilage or repetitive trauma can lead to cartilage damage as well. Pain, stiffness, and grinding or clicking sounds are common (4). As arthritis advances, most patients complain of reduced range of motion and shoulder pain at night.
Shoulder Impingement Syndrome
Shoulder impingement syndrome involves Inflammation of the rotator cuff tendons as they pass through the narrow bony passageway in the shoulder, called the subacromial space (5). Pain, weakness, and restriction in range of motion are the most common symptoms (6).
Pain typically develops over time and is often localized on the top of the shoulder with radiation to the side of the arm (7). Shoulder pain at night is common in patients with shoulder impingement syndrome.
Neck Injury
Referred pain is pain that is perceived or felt in an area different from the location of the actual injury.
For example, disc protrusion or herniations in the neck can cause pain that is referred into the shoulder. Small joints in the neck, called facet joints, can also refer to pain into the shoulder. Facet joints can be injured in motor vehicle accidents or other types of trauma.
Finally, nerves in the neck such as the C6 nerve can be compressed or irritated, resulting in pain that is referred to the shoulder. Changes in the neck position can cause or aggravate shoulder pain at night.
More Conditions Associated With Shoulder Pain At Night
L5-S1 Annular Tear
The labrum is a cartilaginous cup that circles the shallow shoulder socket (the glenoid) to make the socket deeper. The labrum supports and stabilizes the shoulder joint. Causes of Shoulder Labral Tears Injury to the labrum typically occurs from repetitive trauma in overhead throwers, such as in baseball. It can also occur from a traction injury to the arm, such as lifting a heavy object off the ground or getting your arm jerked. Symptoms of Shoulder Labral Tears. Typical symptoms include pain in the front of the shoulder or deep inside the joint. Treatment options initially include physical therapy which is designed to restore range of motion and strength to the shoulder.
Read More About L5-S1 Annular TearAC Joint Impingement
AC joint Impingement is a painful condition that occurs when the space beneath the acromion bone is narrowed. This narrowing can result in irritation of the rotator cuff tendons and bursa. A bursa is a fluid-filled sac that reduces the friction on tendons and muscles as they cross bony surfaces. A tendon is thick collagen tissue that connects muscles to bones. The rotator cuff tendons provide important support and enable movement in the shoulder. If severe, impingement can cause tears in the rotator cuff tendons. Patients with AC joint impingement typically have pain with elevation of the arm and or while lying on the shoulder.
Read More About AC Joint ImpingementAvascular Necrosis of the Shoulder
Avascular Necrosis is essentially a lack of blood flow, eventually resulting in necrosis, or dying of the bone. This happens in multiple joints. And today we are talking specifically about the shoulder. So talking about AVN in the shoulder, patients typically come up with two main questions. Number one, can this heal on its own? And if not, how long or how fast will this progress? Now we classify AVN in multiple different stages: Number one: we have stage one, where it is very normal X-ray — usually, typically, someone just has pain with activity. Is the bone itself continues to deteriorate, then we start getting some changes on your X-ray.
Read More About Avascular Necrosis of the ShoulderCalcific Tendonitis of the Rotator Cuff
Calcific tendonitis of the rotator cuff is a relatively common yet frequently misunderstood shoulder condition. Characterized by the deposition of calcium crystals within the tendons of the rotator cuff, this ailment can lead to significant pain and limited mobility for the affected individual. While it often strikes seemingly out of the blue, its origins and progression are rooted in a combination of biological processes, genetics, and, potentially, lifestyle factors. This article aims to delve deep into the intricacies of this condition, shedding light on its causes, symptoms, treatment options, and preventive measures. This article aims to delve deep into the…
Read More About Calcific Tendonitis of the Rotator CuffEhlers-Danlos Syndrome (EDS)
Disorders that affect and weaken the connective tissues such as tendons and ligaments. It is a hereditary disorder which means you are born with it. EDS has many different signs and symptoms which can vary significantly depending upon the type of EDS and its severity. It most commonly affects the skin, joints, and blood vessels. Joints are typically hypermobile with excessive joint range of motion because of a defect in collagen formation. In most cases Ehlers-Danlos syndrome is inherited. That is to say that you are born with it. The two main ways EDS is inherited are: autosomal dominant inheritance and autosomal recessive inheritance…
Read More About Ehlers-Danlos Syndrome (EDS)Frozen Shoulder
Frozen shoulder, also known as adhesive capsulitis, is a painful loss of shoulder movement and range in motion. The incidence of frozen shoulder is 3-5% in the general population and up to 20% in those with diabetes. The peak incidence is between 40-60 years of age. The exact mechanism is poorly understood. In general, the capsule becomes inflamed, thickened, and contracted with pain and significant restriction in range of motion. causes are poorly understood but risk factors include trauma, prolonged immobility, systematic diseases such as diabetes, stroke, connective tissue disease, and heart disease. Other causes include post-surgery, chronic inflammation causing stimulation of myofibroblasts
Read More About Frozen ShoulderRotator Cuff Tear
Are you plagued by shoulder pain that has now transitioned from intermittent to constant and keeps you up at night? Are daily shoulder movements, such as dressing and reaching for objects in the kitchen cabinets, painful? Is your range of motion decreasing as your pain is increasing? You may have a full- or partial-thickness rotator cuff tear. Has conservative therapy in the form of heat, ice, stretching, rest, and acupuncture failed to provide significant relief? Has an MRI demonstrated a full-thickness or partial-thickness tear of the rotator cuff? What to do? If left untreated, full-thickness and 26% of partial-thickness tears will progress.
Read More About Rotator Cuff TearRotator Cuff Tendinitis
Rotator cuff tendinitis, also known as rotator cuff tendinopathy, is a condition characterized by irritation, inflammation, and degeneration of one or more of the tendons of the rotator cuff muscles in the shoulder. This condition typically arises due to overuse or acute injury, resulting in pain, tenderness, and impaired movement of the shoulder joint. The rotator cuff itself is an anatomical ensemble composed of four muscles and their associated tendons that attach the humerus (the upper arm bone) to the scapula (shoulder blade). These muscles include the supraspinatus, infraspinatus, teres minor, and subscapularis. Each of these muscles plays a pivotal role in stabilizing the glenohumeral (shoulder) joint and allowing for a wide range of motion, including lifting, rotating, and providing the fine motor control necessary for complex arm movements.
Read More About Rotator Cuff TendinitisShoulder Arthritis
Arthritis in the shoulder can present with different symptoms based on the underlying cause of the arthritis. Here’s a list of symptoms associated with shoulder arthritis: Pain can occur in different shoulder locations, which can indicate which part is affected: When the acromioclavicular (AC) joint is affected, the pain is usually experienced at the top of the shoulder. Pain surrounding the shoulder can indicate an involvement of the rotator cuff. The pain can disrupt joint
Read More About Shoulder ArthritisShoulder Impingement Syndrome
Pain is the most common symptom. It typically occurs with the elevation of the arm, forced movement overhead, and when lying on the shoulder. Impingement can also cause shoulder pain when reaching across the body. Narrowing of the subacromial space is the most common cause of shoulder impingement syndrome (6). The subacromial space is the area between the top of the arm bone (humerus) and the AC joint. This narrowing compresses or pinches the rotator cuff tendons and bursa. If left untreated the rotator cuff tendons can become inflamed, damaged, and or torn.Bursa and tendons can not be seen on x-ray. An x-ray may demonstrate…
Read More About Shoulder Impingement SyndromeShoulder Labral Tears
The labrum is a cartilaginous cup that circles the shallow shoulder socket (the glenoid) to make the socket deeper. The labrum supports and stabilizes the shoulder joint. Causes of Shoulder Labral Tears Injury to the labrum typically occurs from repetitive trauma in overhead throwers, such as in baseball. It can also occur from a traction injury to the arm, such as lifting a heavy object off the ground or getting your arm jerked. Symptoms of Shoulder Labral Tears. Typical symptoms include pain in the front of the shoulder or deep inside the joint. Treatment options initially include physical therapy which is designed to restore range of motion and strength to the shoulder.
Read More About Shoulder Labral TearsSwimmer’s Shoulder
On average, a swimmer swims 60,000 meters per week. A large proportion of the forward propulsion in swimming is generated by the upper body. 90% of the driving force in the upper body comes from the torque generated by the shoulder. As a result, the shoulder is put under tremendous load during various swimming strokes to generate this propulsive force. Similar forces act on the shoulder when a person lifts heavy weights overhead or works in a profession or sport with the same shoulder movement. These forces can lead to swimmer’s shoulder, whether caused by impingement of a nerve, a tear in the…
Read More About Swimmer’s ShoulderThoracic Outlet Syndrome
The thoracic outlet is an area around the collar bone where the nerves that come from your neck meet up with the blood vessels from your heart and together supply the entire upper extremity (shoulder and arm). These blood vessels (subclavian artery and vein) and nerves (brachial plexus) travel from the base of your neck to your armpit (axilla) and are considered the “thoracic outlet”. Now that you know what the thoracic outlet is, what is thoracic outlet syndrome? Simply listening to a patient’s history and completing a physical examination is all that is needed to diagnose TOS. But more involved imaging such as X-rays…
Read More About Thoracic Outlet SyndromeThoracic Spine Tumor: Symptoms, Causes, and Treatment Options
The labrum is a cartilaginous cup that circles the shallow shoulder socket (the glenoid) to make the socket deeper. The labrum supports and stabilizes the shoulder joint. Causes of Shoulder Labral Tears Injury to the labrum typically occurs from repetitive trauma in overhead throwers, such as in baseball. It can also occur from a traction injury to the arm, such as lifting a heavy object off the ground or getting your arm jerked. Symptoms of Shoulder Labral Tears. Typical symptoms include pain in the front of the shoulder or deep inside the joint. Treatment options initially include physical therapy which is designed to restore range of motion and strength to the shoulder.
Read More About Thoracic Spine Tumor: Symptoms, Causes, and Treatment OptionsOther Bedtime Discomforts
Shoulder pain may not just be due to problems in the shoulder. Pain from other areas might be affecting the shoulder which can also lead to shoulder pain while sleeping.
- Neck Pain: Pain in the neck can easily affect the shoulders. The nerves that supply the shoulder emerge from the cervical spine. Hence, any injury or damage to the cervical spine can lead to shoulder pain.
- Upper Back Pain: Muscles that support the scapula also fan out over the back and thoracic spine. If there is any strain on these muscles, there’s bound to be some shoulder pain as well.
- Arm Pain: Pain in the arms can also lead to shoulder pain. This could be due to hairline fractures of the humerus or muscle tears of the larger muscles of the arm which also contribute to the shoulder.
- Headache: The shoulder and the neck share some muscles. These muscles also wrap around the nape of the neck. Headaches can radiate to the nape, neck, and the shoulder which can cause shoulder pain at night. At night, the pain is more noticeable as the body is rested and the brain is focused on recovery.
Pain-Reducing Strategies for Improving Sleep Hygiene
Here are some strategies for sleep hygiene that can reduce shoulder pain when you sleep.
- Introduce A Nighttime Routine: It is important to establish a nightly routine that prohibits excessive shoulder movement. This includes no tennis, squash, or bowling in the late evenings.
Try not to hold up a book while in bed that strains the muscles of the arm and forearm. If you have to lift kids, try using a stroller instead.
- Exposure To Natural Light: Reduce exposure to light before sleeping. Late night light exposure disrupts the chemical secreted by the brain called melatonin, which plays a huge role in our sleep-wake cycle.
If you’re exposed to light before bed, it’s harder for you to sleep and harder for the body to rest and relax.
- Avoid Stimulants And Naps Before Bedtime: Stimulants like caffeine, certain medications, and even arguments can affect your brain and its neurochemistry. This affects your sleep and recovery from stress and injury.
Naps before bedtime also contribute to your sleep-wake cycle, thus affecting your sleep. You will find yourself sleeping later and tossing and turning until you do. - Get A Better Mattress: You need a good mattress that supports your spine and shoulders. If the mattress is not firm enough, you may find yourself sinking into it, causing shoulder pain and back aches. If the mattress is too firm it may put too much stress on the shoulder.
Prevention of Shoulder Pain When Sleeping
You can prevent shoulder pain when sleeping by following a few basic steps. They are listed below, based on the time of day and activity.
Bedtime Prevention
At bedtime, follow the following steps to prevent shoulder pain:
- Changing your sleeping position may reduce your shoulder pain. Sleep on your back or your stomach, instead of your side.
- Try out which sleeping postures help with not only minimizing the pain, but also overall sleep quality and comfort.
- Avoid sleeping on the affected shoulder. Sleep on the pain-free side.
- Placing a pillow underneath your chest wall can also help reduce the pressure on the shoulder.
- Placing a firm pillow behind the shoulder helps prevent additional movement.
- Elevating the head of the bed has proven successful for many patients.
Daytime Prevention
During the day, you can take the following steps to prevent shoulder pain:
- Avoid overexertion during sports that require overhead motion or work that requires heavy lifting.
- Take breaks from repetitive motion, like painting or hammering.
- Use wheelbarrows or dollies for carrying heavy loads.
- To prevent shoulder pain, one of the most important steps is to improve posture. Whether while sleeping, standing, or working, your posture affects your shoulders. Since the shoulder joint is complex with the clavicle, scapula, and humerus, the group of muscles and tendons supporting it stretch across the chest and back.
Here are some ways you can improve posture:
- Roll your shoulders and relax the shoulders while you sit or stand in one position for long periods.
- Support your shoulders while you sleep with a towel or a pillow.
- Align your shoulders so that they are always above your hips and not leaning forward, which adds more tension from the neck muscles.
- work on bringing the shoulder blades down and back by learning to activate the rhomboids and external rotators of the shoulder
When You Should See The Doctor
While you may try to rest and use pain medications for your shoulder pain, these are some signs that you may want to visit a doctor:
- Persistent Pain: Severe pain that’s persistent and disrupting your sleep for more than 6 weeks needs to be seen by a doctor.
- Weakness or Motor Impairment: If you have weakness in the shoulder and arm or if you find that you cannot do the same functions like lift, push, or pull as before, see a doctor.
- Numbness: If you have numbness, tingling, or a change in sensation in the shoulder area, then see a doctor as this may be due to a nerve impingement.
- Previous Injuries: For those with a history of shoulder injuries and surgeries, any shoulder pain at night must be seen by a doctor to ensure there is no recurrent injury or blood clots.
Diagnostic Procedures
Various imaging modalities are used to diagnose what is causing shoulder pain while sleeping.
- X Rays: X Rays are first done to evaluate the bone and any bony anomalies or injuries. Measurements of the acromiohumeral distance (AHD) can detect rotator cuff pathologies.
- MRI: An MRI is useful when conservative treatment methods fail after more than six weeks of injury or pain. It allows detailed evaluation of bones and soft tissues within the shoulder girdle.
- CT Scans: While a CT scan is not better than an MRI when it comes to shoulder pain, it is used when MRI is contraindicated in some patients, due to implants or claustrophobia.
- Ultrasound: An ultrasound is a cheaper alternative to an MRI when pathologies such as bursitis, tendinopathy, and/or tendon ruptures are suspected.
What Can Be Done to Treat Shoulder Pain From Sleeping?
The treatment of shoulder pain from sleeping depends entirely on the cause of the pain. Based on what’s causing the shoulder pain, different treatments are offered. The chronicity of the pain can also determine what type of treatment is better.
Below are listed various traditional treatments that are used for shoulder pain during sleep.
Pain Relievers
Pain relievers are pain medications that temporarily reduce pain. These can be NSAIDS (nonsteroidal antiinflammatory drugs) like ibuprofen which reduce inflammation as well. It can also include acetaminophen and even natural compounds like curcumin.
These medications work for four to twelve hours by relieving pain and reducing local inflammation in the shoulder area. If the shoulder joint is only inflamed, then these can treat your condition. However, if there is a chronic cause of inflammation, then these pain relievers are not effective in the long term and have many potential side effects.
RICE
RICE stands for rest, ice, compression, and elevation. This is a conservative therapy for treating shoulder pain but is a bit outdated. Rest should mean avoiding activities or nighttime positions that cause pain. You still want to use your shoulder and work around pain as much as able.
Rest the shoulder by avoiding any overhead movement or lifting. When you sleep, try sleeping on your back or on the side that is pain-free.
If you sleep on your stomach, use a rolled towel underneath your shoulders and a pillow under your hip to align your spine and prevent the shoulders from sagging. Icing the area can temporarily reduce the inflation in the shoulder by constricting the blood vessels but has no evidence that it helps tissue heal in the long term and could be detrimental to healing. Ice should just be used if severe swelling and only for 2-5 minutes at a time.
Compression can also reduce pain and inflammation by constricting blood vessels, which increases blood flow to the area. Elevating the arm can reduce swelling and edema. While you sleep, it would be good if you could rest the shoulder and arm on a side pillow.
Physical Therapy
A physical therapist can help you better by localizing where the pain is coming from and biomechanical problems that could have led to your shoulder pain. A good physical therapist will evaluate your posture and shoulder movement patterns then develop a specific treatment plan for you.
Treatments would include mobility and stabilizing exercises for the shoulder, exercises or stretches to release any tension in tight muscles, and exercises to activate weak muscles. They can also show you which exercises to avoid that can aggravate your condition.
Surgery
Surgery is a last resort when the shoulder pain is unbearable and affects quality of life. If the pain persists for months and months even with conservative treatment and physical therapy, then surgery may be considered. The surgical options depend on the cause of the shoulder pain when sleeping.
For those with complete rotator cuff tears, repair procedures are undertaken; if there is bursitis, then a bursectomy is recommended. For those who have severe shoulder impingement, subacromial decompression and acromioplasty is done to remove the impingement but this is controversial. If there is severe osteoarthritis, shoulder replacement can be performed to relieve shoulder pain.
Steroid Injections
When conservative care fails to provide significant improvement, many patients are referred for steroid injections. Steroids are very powerful anti-inflammatory agents that are toxic to cartilage and should be avoided (8). Repeated steroid injections can weaken the tendons and ligaments and accelerate arthritis.
Regenerative Treatments for Shoulder Pain
There are many regenerative options to treat shoulder pain. PRP and stem cells are some of the most effective, nonsurgical treatment options for shoulder arthritis, bursitis, tendonitis/tendinopathy, labral tears, and partial thickness tears in the rotator cuff.
The PRP and stem cell injections are performed under ultrasound and or Fluoroscopic (Xray) guidance to ensure accurate placement of the platelets and stem cells. This will ensure the best clinical outcome. The injections cannot be performed by your PCP or orthopedic surgeon as they require a specialized skill set.
Moreover, the preparation and processing of stem cells and PRP requires a specialized laboratory that is not available at a typical doctor’s office.
Our randomized controlled study examined the use of bone marrow concentrate containing stem cells for rotator cuff tears and demonstrated significant clinical and radiographic improvement in comparison to patients who underwent exercise therapy (9).
We also published a prospective registry data study examining the use of bone marrow concentrate for shoulder arthritis and rotator cuff tears show significant improvements in patients pain and function (JPR-80872—-a-prospective-study-of-the-safety-and-efficacy-of-a-speci (nih.gov)).
Disc herniations and bulges that cause referred pain in the shoulder can be treated with PRP and bone marrow concentrate containing stem cells as well.
We have published on the use of prolotherapy and PRP treating cervical spine pain (Cureus | Regenerative Injection Treatments Utilizing Platelet Products and Prolotherapy for Cervical Spine Pain: A Functional Spinal Unit Approach | Article).
This allows patients to avoid the side effects of steroid injections and pain management procedures that burn the nerves in the neck. It also enables patients to avoid shoulder surgery.
To learn more about shoulder pain and how you can avoid shoulder surgery, click here.
At the Centeno-Schultz Clinic, we are experts in the treatment of shoulder injuries. Every new patient examination includes an ultrasound examination of the shoulder. These examinations can identify instability and small defects in the tendons and ligaments not often found on MRI or CT.
You Can Sleep Without Shoulder Pain
Shoulder pain at night can be debilitating. The best treatment for shoulder pain at night involves identifying the underlying problem; only then can the appropriate therapy be applied to the area of damage or irritation.
Conservative therapy, when appropriate, is the first-line therapy. Steroid injections should be avoided, as they are toxic. PRP and stem cells are effective, non-surgical options in the treatment of shoulder pain at night.
Most importantly, shoulder pain at night is an indication that something is wrong and action is required. If left untreated, the small problem may grow into something more difficult to manage.
If your shoulder keeps you up at night, or if you are awakened regularly when you roll over, please schedule a telemedicine consultation from the comfort of your home. Identifying and treating this early allows doctors to use many options before surgery. If caught on time, only conservative management would be enough to ease the pain.
Speak with a board-certified, fellowship-trained physician who will provide you with a diagnosis and the appropriate regenerative treatment options.
Reclaim the comfort of a proper sleep. Consult with us today!