Annular Tear
Causes, Symptoms, Treatments, & More Resources
Low back pain can be debilitating and have many different causes. Today we’ll be discussing annular tears. The first question is what is an annular tear? Are annular tears painful? Is an annular tear the same as a herniated disc? What are the annular tear treatment options? Let’s dig in.
What is An Annular Tear?
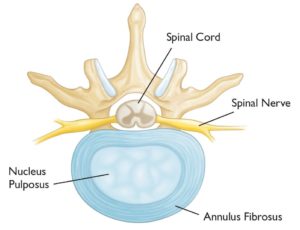
To understand annular tears, let’s first review the anatomy of the spine. The lumbar spine is comprised of 5 boney building blocks called vertebral bodies. Sandwiched between the vertebral bodies are the lumbar discs. Each disc is comprised of an outer fibrous ring, the annulus fibrosis that surrounds the inner gelatinous center, which is called the nucleus. The disc absorbs the forces of daily living. The annulus has multiple layers of collagen that provide important support. The annulus is similar to the sidewall of a tire which provides important stability for the tire.
Causes of Annular Tear
Through trauma or degeneration, the outer annular fibers can become injured and or weakened. This weakening in one or more annular layers can result in an annular tear. The diagnosis of an annular tear is made after a radiographic examination such as an MRI. An annular tear is a bright signal in the outer wall of the disc which can also be referred to as a high-intensity zone in MRI reports (1).
To learn more about annular tears please watch the video below.
Common Symptoms of an Annular Tear
Calf Muscle Twitching
A twitching calf muscle may seem like no big deal, and if it’s just a temporary annoyance that lasts a couple of days and then goes away, it may be. However, it can also be a warning sign of something bigger, especially if it continues. So, today, we’re going to explain a little about the calf and why it’s not a good idea to ignore calf muscle twitching. If there’s one muscle you’re likely familiar with, it’s the calf muscle. If you reach around and grab your calf and flex it, the muscle you are actually feeling just under the surface is called the gastrocnemius muscle.
Read More About Calf Muscle TwitchingLower Back Pain When Sitting
After a long day on your feet sitting down is supposed to be way to relaxing. Unfortunately for some sitting for any length of time can be painful. Most people experience low back pain at some point in their life. The lifetime prevalence of low back pain is 85% (1). Let’s take a deeper look at the different types of pain and causes of low back pain when sitting. Pain can present in many different ways. It can be intermitent or constant. The quality of the low back pain can also vary depending upon the actual source of injury. Common examples include: Sharp and Stabbing, Dull and Aching, Throbbing/ Pulsating, Pins and Needles, Burning, Electrical
Read More About Lower Back Pain When SittingLower Back Pain When Standing
When you’re seated, the facet joints in your lower back are in an open and slightly flexed position. When you stand up, these joints compress. If they are painful or have arthritis, you’ll have pain as you stand up because this puts pressure on the painful joints. In addition, if there is any type of movement of one vertebra forward on another (called spondylolisthesis), then this shift will have occurred as you sit. This is called degenerative spondylolisthesis. When you get back up, the vertebrae will come back into position after a few seconds, leading to that awkward “walk it out period” that starts out painful and ends up more normal.
Read More About Lower Back Pain When StandingUpper Back Pain Between The Shoulder Blades
Upper back pain between the shoulder blades is also known as interscapular pain. Fifteen percent of the population suffers from chronic upper back pain. Finding the source of interscapular pain can be tricky because the upper back houses many important structures like the heart, the upper lobes of the lung, the cervical spine, the scapulas, and a dozen or so of muscles and nerves.
Read More About Upper Back Pain Between The Shoulder BladesAre Annular Tears Painful?
No, not all annular tears are painful. In fact, annular tears are commonly identified in individuals without low back pain. In a recent study of patients with no low back pain who underwent MRI examination, annular tears were found in 56% (2). Similar findings were found in the cervical spine. In a 2005 study of patients with no neck pain, 37% had an annular tear (3). Annular tears can become symptomatic and cause localized lower back pain aggravated by sitting. Patients with annular tears can also have other disc injuries which include protrusion and herniations. Often times the disc protrusions and herniations are the sources of the pain. Annular tears by themselves are not an indicator that a given disc will undergo additional degeneration in the future (4).
Is an Annular Tear the Same as a Herniated Disc?
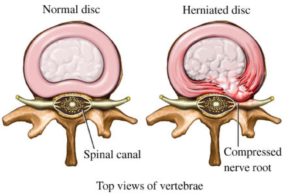
No. An annular tear is a weakness in the outer fibers of the annulus that results in a tear in the collagen fibers. Tears are common in patients with no low back pain. The inside of the disc, the nucleus is not involved. Disc herniation, on the other hand, is when the outer annular fibers are so severely weakened that the gelatinous center of the disc passes through the annulus and is extruded out into the spinal canal. An annular tear may not be associated with low back pain whereas a disc herniation is typically associated with severe low back and often times leg pain.
How Long Does it Take Annular Tear to Heal?
Healing times vary significantly based on the severity of the annular tear and whether or not the tear is associated with disc protrusion or disc herniation. The annulus has very poor blood flow which can impact healing.
Annular Tear Treatment Options
L 4/5 Fusion Surgery
Spinal fusion is a major surgery where one or more spinal bones (vertebrae) are fused together using screws, bolts, and or plates. The hardware may be placed in the front (anterior) or the back (posterior) of the spine. The disc between the spinal bones is often times removed and replaced with bone or a spacer. L 4/5 refers to the level of the surgery. There are 5 spinal bones in the low back which are numbered from top to bottom L1, L2, L3, L4, and L5. Sandwiched between each of the spinal bones is a disc. The disc is named for the two spinal bones it is sandwiched between.
Read More About L 4/5 Fusion SurgeryL5 S1 Fusion Surgery
Spinal fusion is a major surgery where one or more spinal bones (vertebrae) are fused together using screws, bolts, and or plates. The hardware may be placed in the front (anterior) or the back (posterior) of the spine. The disc between the spinal bones is often times removed and replaced with bone or a spacer. L5 S1 Fusion refers to the level of the surgery. There are 5 spinal bones in the low back which are numbered from top to bottom L1, L2, L3, L4, and L5. Sandwiched between each of the spinal bones is a disc. The disc is named for the two spinal bones it is sandwiched between.
Read More About L5 S1 Fusion SurgeryNSAIDs
The other day I was evaluating a patient and reviewing the treatment options for their spine condition. After discussing prior treatments, we got to the topic of medications taken for pain relief. She explained that she mainly utilized anti-inflammatory (NSAID) medications and then she told me to hold much she takes and has been for many years…..she takes close to 2 grams (2000 milligrams) on a daily basis which equated to about 9-10 capsules of medication per day. I was shocked, considering she was pre-diabetic and with high blood pressure plus the kicker of it is that her PCP (primary care physician) is ok with this…
Read More About NSAIDsPerc-FSU – Trusted Alternative to Spinal Fusion
The Perc-FSU Procedure is an injection-based treatment that utilizes the patients’ own blood platelets to bring stability to the spine without the need for the rods, nuts, bolts, and hardware of fusion surgery. “Perc” stands for percutaneous, and “FSU” stands for “Functional Spinal Unit,” which means that the spine is treated as one functioning unit. Up and down the spine, the discs, facet joints, ligaments, and muscles that assist in stabilizing the spine are treated with image-guided injections of PRP and Platelet Lysate to help bring stability to the spine as a whole. It is the trusted alternative to spinal fusion.
Read More About Perc-FSU – Trusted Alternative to Spinal FusionProlotherapy Injections
It has been successful in the treatment of many disorders including neck, shoulder, knee, and ankle pain. Dr. Centeno recently published an article in The Journal of Prolotherapy in which he discusses the use of x-ray guidance with prolotherapy. This ensures that the injection is in the correct place to maximize clinical results. Dr. Centeno discusses the use of prolotherapy for the treatment of neck, knee, sacroiliac joint, ankle, ischial tuberosity, and shoulder pain. At the Centeno-Schultz Clinic x-ray guided prolotherapy is just one of the therapies utilized in the successful treatment of pain. Regenerative injection therapy (RIT) or prolotherapy…
Read More About Prolotherapy InjectionsPRP Injections
PRP is short for platelet-rich plasma, and it is autologous blood with concentrations of platelets above baseline values. The potential benefit of platelet-rich plasma has received considerable interest due to the appeal of a simple, safe, and minimally invasive method of applying growth factors. PRP treatments are a form of regenerative medicine that utilizes the blood healing factors to help the body repair itself by means of injecting PRP into the damaged tissue. In regenerative orthopedics, it is typically used for the treatment of muscle strains, tears, ligament and tendon tears, minor arthritis, and joint instability. There have been more than 30 randomized controlled trials of PRP…
Read More About PRP InjectionsThoracic Spine Surgery
Thoracic spine surgery is a major surgery aimed at treating injuries in the thoracic spine. Because of the complex anatomy and close proximity to the heart and lungs, there are significant surgical risks and complications. Surgery on the thoracic spine can take hours and may require deflating the lung in order to gain access to the thoracic injury. Recovery can be lengthy depending upon the specific thoracic spine surgery performed. There are several different types of thoracic spine surgery. The specific thoracic spine performed depends upon the underlying thoracic injury and a symptoms of the patient. For example, a thoracic disc herniation…
Read More About Thoracic Spine SurgeryTransforaminal Lumbar Interbody Fusion (TLIF)
Transforaminal Lumbar Interbody Fusion is a variant of the Posterior Lumbar Interbody Fusion (PLIF) technique described by Cloward in the 1950s. PLIF has been associated with the high incidences of neurological complications, up to 13.6% of permanent neurologic lesions in Barnes’ et al. study, in particular of the traversing nerve root (2,3) This is due to the fact that a great amount of traction on the dural sac is required to implant the interbody fusion devices. Surgeons have transitioned to TLIF in efforts to reduce complication rates. Success rates vary depending on what literature you read and recently all orthopedic surgery literature has come under fire…
Read More About Transforaminal Lumbar Interbody Fusion (TLIF)Annular tears that are painful are typically associated with disc protrusion or herniations. When conservative care in the form of PT, activity modification, or safe anti-inflammatory medications fail to provide significant or sustained benefit, lumbar injections are often recommended. Steroid injections have significant side effects which include risk of osteonecrosis, increased risk of fracture in older women, cartilage breakdown, and stem cell toxicity (5). PRP is an alternative and has been demonstrated to be effective in reducing low back pain due to disc injury (6). PRP injected directly into the disc has been effective at 5-9 years after the injection in reducing pain and increasing function in patients with low back pain (7).
The Centeno-Schultz Clinic was the first clinic in the world to inject bone marrow-derived stem cells into a lumbar disc. We have extensive experience in the treatment of annular tears and other disc injuries. We have published our results which demonstrated bone marrow-derived stem cells injected into a lumbar disc were both safe and effective in reducing pain and increasing function (8). Bone marrow-derived stem cells and or PRP can be injected directly into the annulus to treat painful annular tears. The procedure is called a Perc-Orthobiologic Annuloplasty. To watch a lumbar disc stem cell procedure please click on the video.
Do Annular Tears Require Surgery?
Surgery is often recommended for the treatment of lumbar disc injuries including annular tears. Unfortunately, surgery is associated with a number of problems including infection, failure, escalation in pain, nerve damage, and atrophy of supporting muscles. Lumbar fusion is a surgery whereby the spine bones are bolted together. A major complication from this procedure is disc degeneration above and below the fusion which is called adjacent segment disease. To better understand fusion surgery and adjacent segment disease.
In Conclusion
The annulus is a thick ring of collagen fibers that surrounds the gelatinous inside portion of the disc. The annulus is susceptible to injury due to trauma or degeneration. Annular tears are diagnosed by MRI examinations and are oftentimes not associated with any pain. Patients with annular tears may also have other disc injuries including disc protrusions and herniations. Annular tears are different than disc herniations. Activity modification, PT, and anti-inflammatory medications are conservative annular tear treatment options. Steroids are associated with significant side effects. PRP and stem cell injections are effective non-surgical treatment options for annular tears and other back conditions.
Doctors Who Help With Annular Tear

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics. He is board-certified in physical medicine and rehabilitation with a subspecialty of pain medicine through The American Board of Physical Medicine and Rehabilitation. Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who…
Read more
John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreMore Resources for Annular Tear

The Spine Owner’s Manual: How to Avoid Back Pain & Life-Altering Surgery
This e-book from Dr. Chris Centeno focuses on the spine and how it functions within the human musculoskeletal system and the body as a whole. Everything in our bodies works together like a well-tuned symphony to support our well-being, and a strong spine (including all of its component parts, such as spinal nerves, ligaments, muscles, etc.) is critical to complete health.
Using the Regenexx SANS approach, The Spine Owner’s Manual provides a series of tests and clearly defined exercises that you can do on your own to measure and monitor your own spinal health. These musculoskeletal tests will allow you to monitor where your own body might be struggling to maintain proper stability, articulation, symmetry, and neuromuscular function.
-
Back Fusion
Spinal fusion, also known as back fusion, is a surgical procedure designed to help severe spinal instability that causes severe pain or nerve injuries. It involves permanently connecting two or more vertebrae in your spine to eliminate motion between them. This article will delve into the intricacies of spinal fusion, exploring the reasons behind the…
-
Understanding the Thoracic and Lumbar Spines
The thoracic spine and lumbar spine make up a vital nexus of stability and mobility in the human body. In this exploration, we delve into the biomechanics and complexities that define these regions, unraveling their significance in posture, movement, and overall well-being. Understanding the thoracic and lumbar spine not only illustrates the mechanics of our…
-
Understanding the Role Of The Thoracic Spine Muscles
The thoracic spine plays a critical role in the stability and mobility of the upper body. Comprised of twelve vertebrae and an intricate network of muscles and ligaments, it serves as a central pillar supporting the structure and movement of the body. Understanding the role and function of thoracic spine muscles is pivotal for anyone…
-
Exploring the Lumbosacral Joint: What Should You Be Wary Of?
The L5 S1 joint, or the lumbosacral joint, is a critical joint. It lies between the lumbar segment of the spine and the auricular processes of the sacrum. The L5-S1 joint plays a vital role in transmitting the weight of the body via the sacrum and ilium downwards. The weight is distributed to the femur…
-
What Is The Cervical Spine? Understanding Its Role And Functions
Neck pain is a significant contributor to worldwide disability, affecting people of all ages and both sexes. According to the Global Burden of Disease Study 2019, neck pain is the fourth leading cause of years lived with disability (YLD) globally, accounting for 43.9 million YLDs. Neck pain can be caused by various factors such as…
-
What is a Cervical Disc?
There are 23 discs in the spine: 6 in the cervical region (neck), 12 in the thoracic region (middle back), and 5 in the lumbar region (lower back). The disc’s function is to provide flexibility and stability to the spine. The disc absorbs approximately 70% of the forces placed on the spine in multiple movements…
__________________
1.Park KW, Song KS, Chung JY, et al. High-Intensity Zone on L-spine MRI: Clinical Relevance and Association with Trauma History. Asian Spine J. 2007;1(1):38-42. doi: 10.4184/asj.2007.1.1.38
2. Stadnik TW, Lee RR, Coen HL, Neirynck EC, Buisseret TS, Osteaux MJ. Annular tears and disk herniation: prevalence and contrast enhancement on MR images in the absence of low back pain or sciatica. Radiology. 1998;206(1):49-55. DOI: 10.1148/radiology.206.1.9423651
3. Ernst CW, Stadnik TW, Peeters E, Breucq C, Osteaux MJ. Prevalence of annular tears and disc herniations on MR images of the cervical spine in symptom free volunteers. Eur J Radiol. 2005;55(3):409-14.DOI: 10.1016/j.ejrad.2004.11.003
4. Farshad-Amacker NA, Hughes AP, Aichmair A, Herzog RJ, Farshad M. Is an annular tear a predictor for accelerated disc degeneration. Eur Spine J. 2014;23(9):1825-9.
5. Wyles CC, Houdek MT, Wyles SP, Wagner ER, Behfar A, Sierra RJ. Differential cytotoxicity of corticosteroids on human mesenchymal stem cells. Clin Orthop Relat Res. 2015;473(3):1155-64.DOI: 10.1007/s11999-014-3925-y
6.Akeda K, Yamada J, Linn ET, Sudo A, Masuda K. Platelet-rich plasma in the management of chronic low back pain: a critical review. J Pain Res. 2019;12:753-67.DOI: 10.2147/JPR.S153085
7. Monfett M, Harrison J, Boachie-Adjei K, Lutz G. Intradiscal platelet-rich plasma (PRP) injections for discogenic low back pain: an update. Int Orthop. 2016;40(6):1321-8.DOI: 10.1007/s00264-016-3178-3
8. Centeno C, Markle J, Dodson E, et al. Treatment of lumbar degenerative disc disease-associated radicular pain with culture-expanded autologous mesenchymal stem cells: a pilot study on safety and efficacy. J Transl Med. 2017;15(1):197.DOI: 10.1186/s12967-017-1300-y