Avascular Necrosis of the Shoulder
Causes, symptoms, Treatments, and Other Resources
Today, we’re talking about Avascular Necrosis in the shoulder. Avascular Necrosis is essentially a lack of blood flow, eventually resulting in necrosis, or dying of the bone. This happens in multiple joints. And today we’re talking specifically about the shoulder. So talking about AVN in the shoulder, patients typically come up with two main questions.
Number one, can this heal on its own? And if not, how long or how fast will this progress?
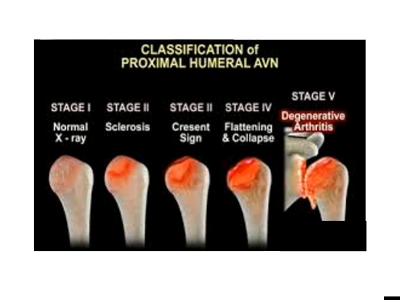
Now we classify AVN in multiple different stages:
- Number one: we have stage one, where it’s very normal X-ray — usually, typically, someone just has pain with activity.
- Two: is the bone itself continues to deteriorate, then we start getting some changes on your X-ray.
- Number three: as that lack of blood flow to the bone progresses, we’re getting what we call a crescent-shaped lesion in the bone. And we start changing some of the architecture of the joint.
- Stage four and stage five is when we start losing full architecture, where we have collapse or flattening of the joint’s surface. That flattening of the joint’s surface essentially leads to severe degeneration or secondary arthritis of the joint.
Symptoms of Shoulder AVN
Avascular necrosis of the shoulder causes pain and a crackling sound when moving your arms and shoulder. The humeral head may collapse, causing discomfort and dysfunction. Changes in the cartilage on the humeral head can cause shoulder joint pain as well.
Left Shoulder Blade Pain
Learn to know the symptoms and causes of shoulder blade pain as well as the diagnostic tests to run for it and its treatment options. Shoulder blade pain can be a common, annoying, hard to diagnose problem. There are many different causes of shoulder blade pain and the exact cause of the shoulder blade pain will determine what type of treatments would be recommended.
Read More About Left Shoulder Blade PainMuscle Spasm In Shoulder
A muscle spasm, also known as a muscle cramp, is a sudden and involuntary contraction or tightening of a muscle or group of muscles. This can occur in any part of the body but is most commonly experienced in the legs, arms, and back. These spasms can last for a few seconds up to many minutes. Occasional muscle spasms may not be something to worry about, but chronic muscle spasms can be a serious issue. In the shoulder, there are many muscles that can go into spasm. These spasms or cramps can cause pain, stiffness, and limited mobility.
Read More About Muscle Spasm In ShoulderShoulder Cracking
The Scapula is your shoulder blade. It is a large triangular bone that compromises part of the shoulder joint. The Scapula is positioned over the back chest wall and ribs where it moves in different directions with shoulder movements (1). The Scapula meets with the arm bone (humerus) to form the shoulder joint. It also meets with the clavicle to form the AC joint. Multiple structures attach onto the Scapula which provides important support and movement for the scapulae and shoulder joint (2). These include:- Muscles/Tendons: Multiple muscles attach to the Scapula which include the deltoid, supraspinatus, infraspinatus, triceps, and teres minor.
Read More About Shoulder CrackingShoulder Pain Radiating Down Arm to Fingers
Common Cervical Radiculopathy symptoms include neck pain, arm pain, shoulder pain radiating down arm to fingers, numbness, tingling, and weakness. Cervical Radiculopathy is a clinical condition in which a nerve or nerves in your neck become irritated or compressed. It is also known as ” a pinched nerve,” The causes are discussed below. It can affect individuals of any age with peak prominence between ages 40-50 years of age. Cervical Radiculopathy is due to spinal nerve inflammation, irritation, or compression. The most common causes of Cervical Radiculopathy are: Disc Injury – The disc is an important shock absorber. Unfortunately, it is susceptible to injury.
Read More About Shoulder Pain Radiating Down Arm to FingersShoulder Pain When Reaching Across Body
Shoulder pain can make simple chores almost impossible. Have you ever reached for an object high on a shelf only to have pain that takes your breath away? What causes shoulder pain when reaching across the body? What is shoulder impingement? What does shoulder impingement feel like? Can a shoulder X-ray show shoulder impingement? What are the treatment options for shoulder pain when reaching across the body? ulder impingement and rotator cuff injuries are among the most common causes of shoulder pain (1). Both can cause shoulder pain when reaching across the body. Shoulder impingement is a painful condition in which the bursa and muscles of the shoulder are pinched or compressed.
Read More About Shoulder Pain When Reaching Across BodyShoulder Pain When Sleeping
There are several reasons why shoulder pain at night occurs or is aggravated; The common explanations include: Sleep typically involves a static position lasting hours at a time with little or no movement. Sleeping on your side places additional pressure on the tendons and bursa of the shoulder. Sleep can cause muscles and tendons to settle in a slightly different position resulting in additional pressure and reduced blood flow. Identifying the underlying problem is important! This allows therapy to focus exclusively on the exact problem or problems. When appropriate conservative care is always the first line of treatment. Focus is typically on strengthening and improving range of motion.
Read More About Shoulder Pain When SleepingShoulder Popping
Noises in the joints, such as popping, cracking, or clicking, can be quite disturbing and cause concern. That popping feeling is called crepitus. That’s something to be ignored, right? It certainly seems harmless enough—after all, there’s no pain, just that annoying popping when you move your shoulder this way or that. But just because there’s no pain doesn’t mean there’s no problem. There’s actually good news and bad news here. The good news? All that shoulder popping really could be no big deal. The bad news? That popping could be slowly chewing up your shoulder joint, and it may be a warning sign that arthritis is on its way.
Read More About Shoulder PoppingHow Fast Is this Progress?
For each individual, it can be extremely different. It could progress over a number of months — could progress over a number of years. Typically, at the time of diagnosis, if someone is symptomatic, the chances of progressing over a three-year period are probably in the 85/90 percent range. If someone is asymptomatic, meaning this was found just by chance, or for a different reason, someone has a chance progression of probably 65 percent.
And that progression looks like this. Where, initially, you have some mild changes on the X-ray. Typically, the symptoms are very mild. As we progress, here is that crescent shape lesion. And, on the bottom right, total destruction of the joint.
Is AVN of the Shoulder Serious?
In one word: yes. It’s extremely serious from the perspective of joint preservation. Now, the earlier we are able to identify this, the quicker we’re able to identify some of the causes of the AVN, remove those causes, and, hopefully, stop the progression. And if we treat this early enough, the goal is joint preservation, so we can avoid the need for a total joint replacement.
What Is the Best Treatment for Avascular Necrosis of the Shoulder?
If we look at the last 15 to 20 years from a research standpoint, there have been two main treatments that become the standard of care.
Remove the Cause of AVN
One is the removal of whatever is causing Avascular Necrosis, such as if it is high-dose cortical steroids; stop the steroid use. Or, if someone’s consuming high amounts of alcohol. Ideally, abstaining from alcohol use itself will, ideally, help stop the progression.
Early Diagnosis is Key
From a treatment standpoint, trying to get the Avascular Necrosis to reverse or cure. That’s why identifying early on and getting in that early stage one to stage three is extremely important.
An orthopedic surgeon typically does what’s called a core decompression, where they take a large drill bit, go into the bone itself and ideally try to stimulate the bone, to regenerate it. Aside from that, a less invasive option would be a bone marrow concentrate, utilizing the repair cells in your bone marrow — concentrating them, and, with a small needle, injecting them directly into the lesion to stimulate your body to regenerate the blood flow, as well as try to heal the bone itself.
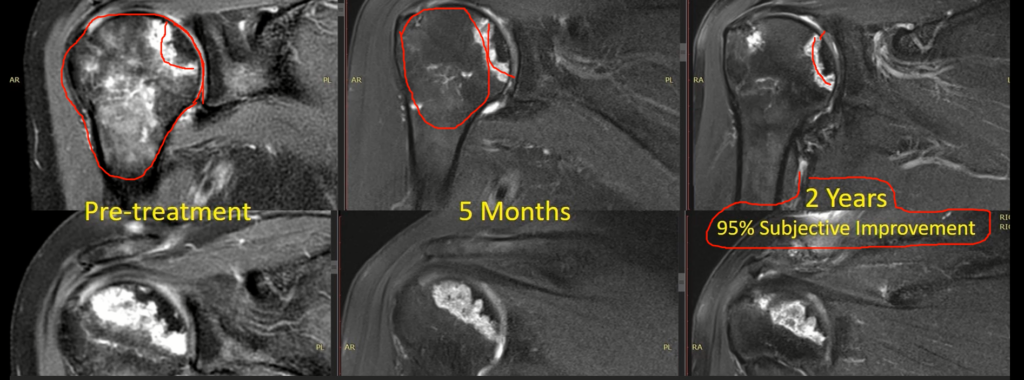
Here’s a nice progression from someone that was diagnosed from stage three (see above). All this area is Avascular Necrotic lesions. We can see the crescent-shaped lesion here (where it says “Pre-treatment,” to the left). But the good news is they still had preservation of the joint structure. After treatment, we can see five months (middle). We have a resolution of the majority of the bone swelling. We still have a small lesion, but it hasn’t progressed, and, if we fast forward several years, the patient themselves is 95 percent improved from pain and function after two years. And there’s been no progression of the Avascular Necrosis lesion, as well as the joint preservation aspects are maintained (the right-most image).
So, if you or any loved one have been dealing with any issues with Avascular Necrosis in the shoulder, feel free to give us a call. If you have any questions, you can always reach out to us on social media, such as Instagram, Facebook, and we’re always more than welcome to do Telemedicine evaluations. You can send in your imaging and set up a review of your imaging to see if you are a candidate for these advanced regenerative techniques. Have a good day.
Related: Avascular Necrosis Staging
Our Doctors Who Assist with Shoulder AVN

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreOther Resources for AVN
-
Avascular Necrosis Staging [VLOG]
Dr. Markle talks about Avascular Necrosis staging, reversing AVN, and treatment options. Transcript Hello, Dr. Markle here at Centeno-Schultz Clinic in Broomfield and Denver, Colorado. Today, we’re talking about avascular necrosis staging. Now, the staging of avascular necrosis is critical in someone’s long term prognosis and moving forward to form an appropriate treatment option. Avascular…
-
Avascular Necrosis of the Knee: The Best Treatment Options
Dr. Jason Markle presents the causes, progression, and the best treatment options for Avascular Necrosis of the knee. Transcript Dr. Jason Markle Hello, Dr. Markle here, of Centeno-Schultz Clinic, talking about Avascular Necrosis of the knee, also known as osteonecrosis. Causes of AVN So let’s talk about some of the causes of AVN…
-
Matt Chan’s Journey with CrossFit Injuries and Regenexx Treatments
Matt Chan, a Denver Firefighter, and National CrossFit Champion undergoes treatment at the Centeno-Schultz Clinic. Dr. Schultz discusses how athletes and others can successfully use stem cells to treat knee and back injuries.
-
Dramatic Shoulder Fracture Nonunion and AVN Stem Cell Treatment Results
We love following up with our patients to find out how they are doing weeks, months, and even years following their treatments. Perhaps the most exciting of these are those patients whose issues were so severe that even surgery had nothing to offer them, yet they turned to interventional orthopedics and report successful outcomes following…
-
The Stem Cell Count in Your Injections Matter!
Why Stem Cell Count Matters! As a society, we are obsessed with numbers and precise detail. In the grocery store, we scour labels to ensure that our foods are low in both sodium and carbohydrates. With mobile phones, we compare LCD screen sizes, pixel resolutions, storage options, and battery life. When selecting vehicles, we drill…
-
Can Osteonecrosis Be Treated Without Surgery?
Osteonecrosis, directly translated, means death (necrosis) of bone (osteo-). It can be a frightening diagnosis for a patient to hear. First, a patient will likely wonder if there is anything that can be done to stop the bone from dying, and if the physician advises surgery, which they almost always do, a patient might wonder…