PRP for ACL Tears & Sprains
Platelet-Rich Plasma for ACL Injuries in Denver, Colorado
Am I a Candidate?ACL Tears
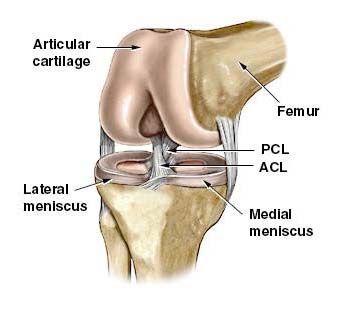
The ACL is one of the main ligaments of the knee. Its most important role is to prevent your tibia (shin bone) from moving forward on your femur (thigh bone). ACL injuries commonly occur when you twist or rotate while running, planting, and stopping suddenly or landing hard on your leg after a jump. However, sometimes people without any of these factors involved will also get this injury. Athletes are at high risk for ACL tears because they often play sports that require quick starts, stops, and jumps. If you tear your anterior cruciate ligament (ACL), it usually means surgery followed by months of downtime before you can return to activities like basketball, skiing, or soccer. However, PRP has been shown to be an effective treatment option for mild forms of ACL tears.
PRP Injections into the ACL
“PRP” is short for platelet-rich plasma, and it is autologous blood with concentrations of platelets above baseline values (1). Platelet-rich plasma (PRP) has been growing in popularity since it was discovered to have the potential to improve overall joint function, decrease pain and inflammation, and help the body repair itself via injections into damaged or diseased joints. PRP treatments are a type of regenerative medicine that uses your blood’s healing factors to help the body heal itself by injections of PRP into injured tissues. It is commonly used in regenerative orthopedic therapies for muscular strains or tears, ligament tears, tendon ruptures, minor arthritis, and joint instability.
There have been more than 30 randomized controlled trials of PRP, and it has been shown to help the body heal itself by its stimulating effect on the stem cells within the targeted area. In fact, our own Dr. Chris Centeno has used the analogy of “expresso shots” to explain how PRP and our patented Platelet Lysate work within and with the body.
Grade 1 Tears
A partial-thickness ACL tear is where only a portion of the ACL is torn. On ultrasound or MRI, a portion of the ACL would be torn but the remaining fibers would be normal. These types of tears can be treated with ultrasound-guided PRP or bone marrow concentrate.
Grade 2 Tears
A grade 2 ACL tear involves a tear that extends across the entire ACL and therefore is referred to as a full-thickness tear. The ligament has not pulled apart or snapped back upon itself and therefore is referred to as non-retracted. These types of tears can be treated with ultrasound-guided PRP or bone marrow concentrate.
Grade 3 Tears
A grade 3 tear is a full-thickness tear that extends across the ACL and, unlike a Grade 2, the ligament has pulled apart. This means that the two pieces of the ligament have pulled apart or maybe even snapped back like a rubber band. This type of tear requires surgery.
Why Regenexx PRP Mixtures Are Superior
In most clinics that offer PRP therapies, the method of developing PRP involves removing a patient’s blood and running it through a simple bedside centrifuge machine to separate the plasma and concentrate the blood platelets, which are then immediately extracted and used as the injectate. These devices are not great at getting rid of unfavorable cells from the resulting mixture. Our lab tests show that white and red blood cells have an inhibiting effect on the same stem cells the platelets are attempting to stimulate and might cause excessive inflammation following the injection.
Our PRP is purer, concentrated, and customizable because it is produced in a laboratory setting by an experienced technician who can separate and concentrate all the blood’s good components and remove the unfavorable ones.
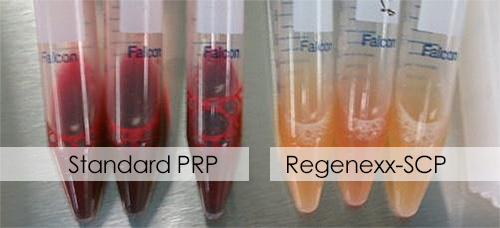
Invented at Centeno-Schultz Clinic, Regenexx’s Super Concentrated PRP procedures are an advanced type of PRP therapy that uses lab-processed PRP mixtures that have been found to provide up to 10 – 40 times more platelet concentrations than the traditional “bloody” PRP. Our PRP, due to its high levels of platelets, has an amber color (see image below).
Our Doctors That Treat ACL Injuries
PRP injection procedures in Denver and Broomfield, Colorado clinics are performed by the following Interventional Orthopedics doctors:

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics. He is board-certified in physical medicine and rehabilitation with a subspecialty of pain medicine through The American Board of Physical Medicine and Rehabilitation. Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who…
Read more
John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreRead more about ACL Injuries
-
Partial ACL Tear
A partial ACL (anterior cruciate ligament) tear occurs when the ligament in the knee is partially damaged, often leading to instability, pain, and limited range of motion. This injury typically results from sudden stops, pivots, or direct impacts, commonly seen in athletes. Early diagnosis and appropriate management are crucial to preventing further damage and ensuring…
-
What Is Golfer’s Knee, And What Can I Do About It?
The nature of golf is such that both the backswing and downswing affect the knee. The entire swing takes a little over one second. However, it can exert a force of 4 times the body weight on the front knee and 3 times the weight on the back knee (1). This makes knee injuries just as…
-
Knee Pain Location Chart: What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
Does a Torn Hamstring Require Surgery? Learn Your Best Alternative
Hamstring injuries range from mild strains to complete ruptures. The need for surgery often depends on the severity of the injury and the specific requirements of the individual, especially if the person is an athlete or has specific functional demands. Several factors influence the outcome of the surgery: Return to sport/activity: Many athletes can return…
-
Everything You Need to Know about Hip Ligaments
The hip joint is a large ball and socket joint that’s important for lower extremity movement. The joints consist of the articulation of the femur (upper thigh bone/ball) and the acetabulum (the socket). The bones are lined with cartilage and the acetabulum is lined with a fibrocartilage called the labrum. The hip joints, as with…
-
Understanding Knee Pain Symptoms To Get The Best Treatments
Knee pain affects about 25% of the population (1). The knee joint involves three bones, namely the patella, the femur, and the tibia. Knee pain can be a sign of damage to the ligaments, bones, bursae, or muscle tendons because there are so many structures within the knee joint. In this post, we’ll discuss the…
References:
- Jones IA, Togashi RC, Thomas Vangsness C Jr. The Economics and Regulation of PRP in the Evolving Field of Orthopedic Biologics. Curr Rev Musculoskelet Med. 2018;11(4):558-565. doi:10.1007/s12178-018-9514-z
Am I a Candidate?
To answer this question, fill out the candidate form below to request a new patient evaluation, and a patient advocate will reach out to you to determine your next steps. Your one-hour, in-office or telemedicine evaluation will be with one of the world’s experts in the field of Interventional Orthopedics.