Our preferred Treatment for PCL Sprain is BMC
Learn MorePCL Sprain
causes, symptoms, treatments, and other resources
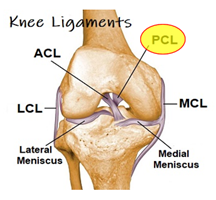
What is a PCL Sprain? To answer that question we need to begin with some knee anatomy. Your knee is held together by ligaments, which are tough connective tissues that have a lot of strong collagen fibers in it. These structures provide stability from all motion. You have ligaments on the medial side (inside of the knee), the lateral side (outside of the knee) and these are referred to as the “Collateral” ligaments. You also have 2 paired ligaments in the middle of the knee which crisscross going in opposite directions, referred to as the “Cruciate ligaments.”
PCL
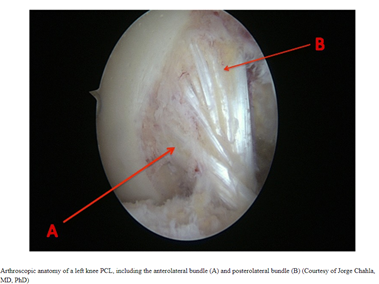
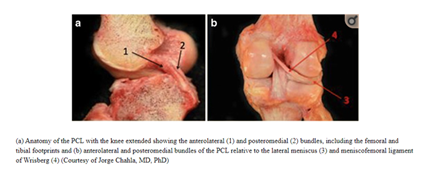
The Posterior Cruciate Ligament is one of the paired ligaments in the middle of the knee. It is made up of 2 separate bundles: The two bundles of the PCL, and the ALB (anterior lateral bundle), and the PMB (posterior medial bundle), function synergistically to provide stability. The PCL functions as one of the main stabilizers of the knee joint and serves primarily to resist excessive posterior translation of the tibia relative to the femur. The PCL also acts as a secondary stabilizer of the knee preventing excessive rotation specifically between 90° and 120° of knee flexion (1,2).
A PCL sprain happens when force is applied beyond what the PCL tensile strength is capable of resisting. The tensile strength of the PCL is well documented in the literature and ranges from 739 to 1627 N (3). Which is about a 300-360lb force!!
What Is Posterior Cruciate Ligament Sprain?
PCL sprain or PCL tears account for only 3% of all knee injuries. These injuries are classified by the severity of the injury meaning how badly the ligament is injured.
Grade 1
Grade 1 is a mild injury that causes only microscopic tears in the ligament. While these small tears can bend the PCL out of shape, they do not significantly affect the knee’s ability to bear weight.
Grade 2
Grade 2 means the PCL is partially torn and the knee becomes unstable. At this level expect the knee to give out periodically while standing and walking.
Grade 3
In Grade 3 the PCL is completely torn or is separated at its end from the bone that it normally anchors. At this point, the knee is very unstable and cannot bear your body weight. It usually takes a tremendous force to cause such an injury, so a grade 3 sprain is often accompanied by damage to the other ligaments of the knee.
PCL sprains or tears rarely exist in isolation as well, with up to 95% of the time there is also some additional ligament damage to other supporting ligaments in the knee.
Symptoms of PCL Sprain
Back of Knee Swollen
Back of knee swollen? Swelling in the back of the knee is not something that is talked about too often. It can be uncomfortable or sometimes painful with the movement of the knee or, even with rest. It often stems from an orthopedic-related issue or, perhaps some other medical condition. Let’s dive in…What’s Causes Swelling in the Back of Your Knee? The back of the knee contains a variety of anatomical structures that can be affected and result in pain, swelling, numbness, tingling, etc. Muscles and tendons behind the knee that could be the source of pain or pathology could be one or more of the following: Gastrocnemius, Soleus…
Read More About Back of Knee SwollenKnee Buckling
Knees can buckle, causing a sensation of one or both knees giving out that affects nearly 17% of adults. The knees are regarded to be one of the most essential (and biggest) joints in the human body because they play significant roles in basic activities such as walking and sitting. When our knees begin to feel unstable, weak, or begin giving out, it is easy to become stressed since we rely so heavily on them for movement. The knee can become stable from numerous types of injuries. The knee is kept stable by the following structures: Tendons attach the leg muscles…
Read More About Knee BucklingKnee Hurts When I Bend It and Straighten It
Your knees bend countless times throughout the day. Running up the stairs, down the hall after kids, and getting into the car. You straighten the knee as you walk, descend stairs or get into and out of the car. Bending and straightening the knee are necessary for daily activities. Knee pain with bending or straightening may be a mild, transient irritation or may indicate a more significant problem. Learn more below and avoid further injury and dysfunction. Knee pain can vary significantly depending upon many factors including the actual source of the pain, the severity of the injury, general health, and level of activity…
Read More About Knee Hurts When I Bend It and Straighten ItKnee Hyperextension
The knee is a hinge joint between the femur and the tibia along with an accessory bone, the fibula. These bones are held together via ligaments that keep the bones aligned while the joint goes through its natural range of motion. These ligaments are: Medial Collateral Ligament (MCL), Lateral Collateral Ligament (LCL), Anterior Cruciate Ligament (ACL), Posterior Cruciate Ligament (PCL). from zero degrees fully extended to 140 degrees fully flexed. BUT when a force from the front to the back overcomes the strength of the ligaments the knee is forced into an unnatural position called “Hyperextension” which, in turn, can…
Read More About Knee HyperextensionKnee Pain
Knee pain can be caused by many factors. Overuse injuries, direct trauma to the knee and arthritis are the most common causes of knee pain. Damage to the knee structures may cause swelling, scar tissue formation (fibrosis), and loss of function of the joint. Pain is often accompanied by difficulty walking, weakness, and instability. When the knee is overused, the thigh and shin bones (femur and tibia), cartilage, or tendons may experience stress. This leads to pain and discomfort as well as stiffness in the knee. Overuse injuries are common among athletes who participate in sports that involve running, jumping…
Read More About Knee PainKnee Popping
Knee popping can be a sensation that something is moving around in the knee. There may also be an audible sound associated with the popping, which in medical terms is called crepitus. This can also cause what we call mechanical catching or locking, which may make the knee feel like it is stuck in an extended or flexed position, and you have to move it in certain ways to get out of that. This knee popping sensation or sound or could be a very simple issue or it could be a sign that more serious damage is going on in the knee, so determining what is causing it is very important. So, the knees may pop and get in a certain position….
Read More About Knee PoppingKnee Swelling
Swelling of the knee, also known as water on the knee, is a condition in which fluid collects around the knee joint. Swelling can occur for a variety of reasons and affect patients of any age. Some swelling can be treated with over-the-counter medicines, but persistent and continuous swelling might result in tissue damage, bone softening, and cartilage deterioration. Over-the-counter medicines will assist relieve pain for individuals with a history of osteoarthritis and swelling following physical activity, such as exercise or running. During and after activity, the patient may apply compression sleeves to reduce the inflammation. Ice is another method…
Read More About Knee SwellingLoose Knee Joint
Ligaments are fibrous bands that connect the bones together. If the ligaments inside your knee become damaged, your knee could feel loose (with or without pain). While walking, exercising, or simply standing, it may feel like your knee could collapse at any moment. If the knee muscles are damaged, they will be unable to contract properly, resulting in lack of strength and discomfort. Swelling might have a similar result. What Causes Laxity in the Knee Joint? Knee injuries are generally sports-related, although they may occur during any physical activity that puts stress on the knee and causes bending or trauma…
Read More About Loose Knee JointPain Behind Knee
First off, this is where the hamstrings and calf muscles attach. They have tendons here that are inserted into the bone. So if there’s a problem in the muscle or the tendon, you’re going to feel it right here. This is also where deep muscles like the popliteus and plantaris live. So, if these have issues, you’re going to feel it in the back of the knee. In addition, the tibial nerve is back here. So if there’s an issue with a nerve in your back or a nerve locally, behind the knee, you’re going to feel it here. And the meniscus or the joint spacer lives back here. And the meniscus or the joint spacer lives back here. So a tear in the meniscus could cause pain…
Read More About Pain Behind KneeReduced Range of Motion in Knees
A knee can feel stiff if there is some swelling in or around the joint or muscle tightness can caused restricted motion This can occur from a problem in the knee joint, such as inflammation, arthritis, or infection, or an injury. The distance and direction that a joint may move are referred to as its range of motion. Various joints in the human body have specific normal ranges set by doctors and therpists. One study, for example, found that a normal knee should be able to bend to between 133 and 153 degrees. A typical knee should also be able to extend fully straight. Limitation of motion occurs when a person range of motion in any limb is reduced below the normal range….
Read More About Reduced Range of Motion in KneesTightness in Knee
What could tightness in your knee mean? When fluid builds up inside the knee as a result of an injury, overuse, or medical problem, the knees become swollen and tight. Swelling might be mild, so you may not always notice it unless it is serious damage. You may feel this as stiffness in the knee since swelling may not be visible. Swelling restricts movement since there is less room in the knee. Fluid buildup can be caused by irritation, internal bleeding, and injuries to the knee. Arthritis, gout, tumors, and baker cysts are all causes of swelling. Pain and swelling are the responses of your body to damage. Together they can lead to stiffness in your knee…
Read More About Tightness in KneeWeak in Knees
Weakness in the knee can be a symptom of many different knee conditions. Some of the most common causes of weakness in the knee include ligament tears, meniscus tears, and arthritis. Another important but often overlooked cause of knee weakness is irritation or injury of the nerves in the low back. If you are experiencing any type of weakness in your knee for long durations of time (3 weeks), it is important to see a doctor to determine the cause. Some of the most common symptoms of knee weakness include difficulty standing up from a seated position, difficulty walking, climbing or descending stairs…
Read More About Weak in KneesWith PCL sprain (grade 1) or tear (grade 2 or 3), patients typically get an inflammatory response in the knee that will lead to a multitude of symptoms.
With Mild To Moderate Pain In the Knee localized swelling in the ligament can create pain in the back of the knee where the PCL attaches.
Swelling
A higher grade PCL sprain (grade 2 or 3) can cause bleeding into the joint from the ligament which produces knee effusion/swelling.
Mild To Moderate Pain In Knee
Localized swelling in the ligament can create pain in the back of the knee, where the PCL attaches.
Knee mobility – Loss of Range of Motion
As a result, both the ligament swelling and knee swelling can cause loss of range of motion. Meaning, you will not be able to fully extend or fully flex the knee.
Knee Instability
High grade (2 or 3) PCL sprain impairs the ligament’s function as well, which can lead to instability and the knee giving out!
Common Causes of PCL Sprain
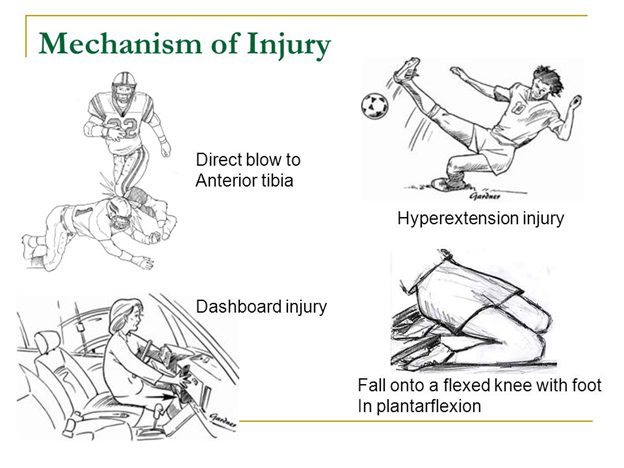
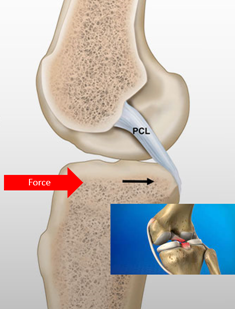
PCL sprain/injuries typically occur in high velocity / high force collisions where there is a strong force applied to the tibia pushing the tibia backward in relation to the femur. At some point, the force is too much for the PCL to resist and then fibers are torn or stretched. There are common instances where this occurs.
Car Accidents
The faster a car is going, the higher the number of forces are applied to the body creating a risk for a multitude of injuries. One being the knee. If the accident pushes the knee into the dashboard this can create a backward force on the shin bone.
Sudden Twist Or Over-Extension Of The Knee
A sudden twist or a moment of hyperextension such as kicking a soccer ball or landing from a high jump in the air where your knee hyper-extends, pushes the tibia backward stressing the PCL.
Contact Sports / Significant Impact On Knee Or Shin
In multiple sports both in contact and non-contact sports, a fall or if someone falls into you can lead to a PCL injury. Commonly in American football, a tackle called a “chop block” or tackling below the pads was outlawed because of the potential for a catastrophic knee injury! But these injuries are seen in more than just American football. They are also seen in rugby, soccer, and many other sports where the players collide in this manner and can lead to PCL and ACL injuries. There has been a conscious effort in many leagues to teach better techniques in avoiding severe knee injuries when taking down your opponent.

Common Treatments for Sprained PCL
Many times when a PCL sprain occurs you don’t know exactly what the injury is. You only get symptoms and signs that a significant injury has occurred as mentioned above. Treatment for acute knee injuries should always be assumed to be more severe than you think so you can act cautiously until a specific diagnosis is found and severity established to further guide your rehabilitation! You want to react with maximal protection of the joint to allow natural healing to occur and help facilitate the resolution of the swelling and pain.
RICE Treatment
Anti-Inflammatory Medications
- Avoid excessive amounts of over the counter NSAIDs (non-steroidal anti-inflammatory medications) as these can actually inhibit the proper healing of the injury. To learn more please read my in depth look at NSAIDs
- Listed in the article are healthy alternatives to the over the counter NSAIDs.
Using Supports
Weight-bearing can cause pain, and using supports can help you get through your day-to-day activities while you’re recovering.
Crutches
if weight-bearing causes significant amounts of pain then you want to minimize weight bearing on the knee until a clear diagnosis is known. Until then, off-loading the knee with crutches can be helpful. This allows for pain reduction as well as prevents further damage to the knee.
Knee Brace
If you have a sense of instability where the knee will not support itself and gives out then using a brace for support is needed. This will help with maximal protection of the knee to prevent additional damage
Physical Therapy
Once there is a clear diagnosis but still a substantial amount of limitations to the knee, physical therapy will be the main component of getting you back to “normal” activity. PT can help reduce the swelling in the joint and start getting the muscles that support the knee back online and working! Long-term PT is an important part of being proactive, meaning it can help prevent future knee injuries!
Surgical Treatment
Like its counterpart ACL-reconstruction, PCL reconstruction surgeries come with significant risk! Like most surgical procedures major risks are known such as a 1-3% chance of infection (4) and an 8-9% risk of a blood clot (5). Given the unique location of the PCL, there is an inherent risk of neurovascular injury can happen during the procedure. The Popliteal Nerve and Artery live just millimeters away from the PCL posterior attachment. If injured this can lead to devastating vascular injury which in turn can create a compartment syndrome, requiring fasciotomy (6).
Long term, PCL reconstruction is similar to ACL reconstruction in that “Patients with PCL tears have a significantly higher risk of meniscus tear, OA (osteoarthritis) and subsequent TKR (total knee replacement) than patients without PCL tears” (7).
Alternative Treatment To Ligament Surgery For Sprained PCL
For the past 15+ years, we have been utilizing Regenexx procedures to promote your body’s natural ability to heal orthopedic conditions without surgery to get you back to doing what you love faster and without the risks associated with major surgery!
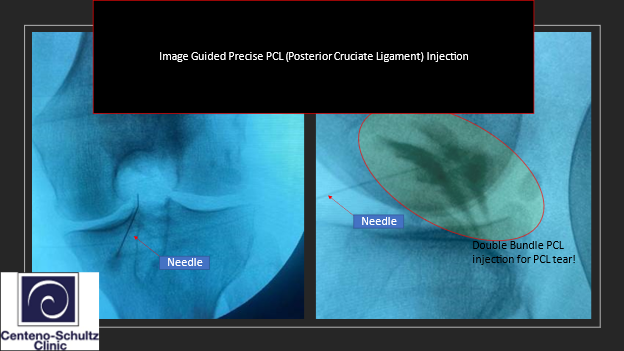
A PCL strain or tear can easily be treated with bone marrow concentrate or platelet-rich plasma precise injection to maximize the healing potential of the PCL! We have completed randomized control trials with before and after pictures using bone marrow concentrate showing that even cruciate ligaments can heal (learn more here).
Knee Arthroscopy Surgery
Knee arthroscopy surgery is a very common procedure performed by orthopedic surgeons in an attempt to treat knee pain. Knee arthroscopic surgery is typically performed in an outpatient surgical facility where a small camera is inserted into the knee joint, which allows the surgeon an inside view of one’s knee to operate. It is used both to diagnose and treat a wide variety of knee problems. Utilizing arthroscopic surgery the surgeon can trim any damaged ligaments which are called knee ligament surgery. Alternatively, if ‘damaged’ meniscus is detected, it also is trimmed and or removed, which is called meniscus knee surgery.
Read More About Knee Arthroscopy SurgeryKnee Ligament Surgery
Knee ligament surgeries have become quite common, ACL (anterior cruciate ligament) surgeries average 250,000+ surgeries alone every year! These invasive surgeries have come under investigation in recent years, wondering the necessity, or need to be done. Your knee has 3 points of contact or compartments that house the cartilage of your knee: the patella-femoral compartment, lateral (outside) compartment, medial (inside) compartment. These compartments are held together by a network of ligaments that hold each bone together and allow the knee to move properly. The main knee ligament surgery…
Read More About Knee Ligament SurgeryNSAIDs
The other day I was evaluating a patient and reviewing the treatment options for their spine condition. After discussing prior treatments, we got to the topic of medications taken for pain relief. She explained that she mainly utilized anti-inflammatory (NSAID) medications and then she told me to hold much she takes and has been for many years…..she takes close to 2 grams (2000 milligrams) on a daily basis which equated to about 9-10 capsules of medication per day. I was shocked, considering she was pre-diabetic and with high blood pressure plus the kicker of it is that her PCP (primary care physician) is ok with this…
Read More About NSAIDsPRP for PCL Sprains & Tears
Physical therapy and RICE are the first-line treatments for PCL injuries. Prolotherapy is also an option in less severe cases, but where ligaments are more severely damaged, PRP and/or bone marrow concentrate (containing stem cells) may be called for as the next nonsurgical treatment option. Platelet-Rich Plasma for PCL Tears & Sprains “PRP” is short for platelet-rich plasma, and it is autologous blood with concentrations of platelets above baseline values. Platelet-rich plasma (PRP) has been growing in popularity since it was discovered to have the potential to improve overall joint function, decrease pain and inflammation, and help the body…
Read More About PRP for PCL Sprains & TearsPRP Injections
PRP is short for platelet-rich plasma, and it is autologous blood with concentrations of platelets above baseline values. The potential benefit of platelet-rich plasma has received considerable interest due to the appeal of a simple, safe, and minimally invasive method of applying growth factors. PRP treatments are a form of regenerative medicine that utilizes the blood healing factors to help the body repair itself by means of injecting PRP into the damaged tissue. In regenerative orthopedics, it is typically used for the treatment of muscle strains, tears, ligament and tendon tears, minor arthritis, and joint instability. There have been more than 30 randomized controlled trials of PRP…
Read More About PRP InjectionsPRP Knee Injections
PRP stands for Platelet-Rich Plasma. Platelets are blood cells that prevent bleeding. They contain important growth factors that aid in healing. Plasma is the light yellow liquid portion of our blood. So PRP is simply a concentration of a patient’s own platelets that are suspended in plasma and are used to accelerate healing. PRP is NOT stem cell therapy. Regrettably, blood contains few circulating stem cells. Rich sources of stem cells are bone marrow and fat. PRP is rich in growth factors. There are many different types of growth factors with different properties. VEGF is a very important one as it can increase the blood flow to an area.
Read More About PRP Knee InjectionsDiagnosing Your PCL Sprain
If you have injured your knee and would like an extensive evaluation, feel free to contact us today so we can further examine your knee and order an MRI to further delineate the injury and extent the injury. With that known then we can come up with a game plan to best get you back on the field, on the trail, or whatever it is that the injury is preventing you from doing!
Preventing PCL Injury
There are many ways to avoid a PCL sprain.
- Stretching / mobility of hips / knees and ankle
- Strengthening leg muscles that protect your knees such as hamstrings and quadriceps
- Listen to your body: if you’re not getting paid millions of dollars to play a sports then if your body isn’t 100% then its not worth the injury.
PCL Sprain Is Common but Not to Be Underestimated
A PCL sprain can happen to any one of us. Regardless of how it happens (car accident, sports injury or just having fun outside) there are several ways to get you back on the field that does not involve surgery. So if you have been dealing with a knee injury, PCL strain or not, come to Centeno Schultz Clinic or contact us, so one of our top physicians can evaluate you and see if you are a candidate for our non-surgical knee procedure for PCL!
Doctors That Can Assist with PCL Sprains

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreOther Resources for PCL Injuries
Free Download: The Knee Owner’s Manual

This e-book by Dr. Chris Centeno examines the knee and its role in the human musculoskeletal system and the body as a whole. The Knee Owner’s Manual provides a series of tests and clearly defined exercises that you can perform on your own to assess and monitor your own knee health. It will allow you to look for trouble spots where your own body may be having difficulty with stability, articulation, symmetry, and neuromuscular function. You’ll be able to see how these deficits in other regions of the body relate to the knee.
The Knee Owner’s Manual also discusses how Regenexx is pioneering the development of interventional orthopedics, a new branch of medicine that employs regenerative biologic therapies such as adult bone marrow concentrate and platelet-rich plasma to help repair and strengthen damaged tissues in other areas of the body.
This is contrasted with invasive knee surgeries, which often remove important tissues or replace the entire knee itself when it becomes damaged. With hyperlinks to more detailed information, related studies, and commentary, this book condenses a vast amount of data, images, and resources into an enjoyable and informative read. This is the first edition of The Knee Owner’s Manual, a companion book to Orthopedics 2.0.
-
What Is Golfer’s Knee, And What Can I Do About It?
The nature of golf is such that both the backswing and downswing affect the knee. The entire swing takes a little over one second. However, it can exert a force of 4 times the body weight on the front knee and 3 times the weight on the back knee (1). This makes knee injuries just as…
-
Knee Pain Location Chart: What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
ACL Tear Treatment Without Surgery: Our New Publication!
It all happened so suddenly. You were running down the field and made a quick cut. You heard an audible pop followed by searing knee pain and then collapsed to the ground. Your doctor thinks your tore your ACL and has referred you to a surgeon. What is the Anterior Cruciate Ligament? What is the…
-
How to Read a Knee MRI for Meniscal Tear
Dr. Chris Centeno discusses how to read a knee MRI for meniscal tears and what you need to know about such tears. Transcript Hi, this is Dr. Centeno. And I’d like to go over today How to Read Your Knee MRI: Focus on the Meniscus. I have a whole series of these and reading a…
-
How to Read Knee MRI
Transcript for “How to Read Knee MRI” Hi, this is Dr. Centeno and I’d like to go over how to read knee MRI. I got the idea for this when a friend had a knee injury, got an MRI, was sent home with the CD, and just jumped on the internet to try to figure…
-
Regenexx ACL Repair vs Reconstruction Surgery for Knee ACL
Regenexx ACL Repair vs Reconstruction Surgery for Knee ACL Today I’d like to highlight a patient named Joe’s story. Joe is unique in that he has had the non-surgical Regenexx Perc-ACLR procedure which uses your own cells injected via a small needle, and a surgical ACL reconstruction, so he can compare the two. So let’s…
References:
- Papannagari R, DeFrate LE, Nha KW, Moses JM, Moussa M, Gill TJ, Guoan L. Function of posterior cruciate ligament bundles during in vivo knee flexion. The American journal of sports medicine. 2007 Sep;35(9):1507-12.
- Ahmad CS, Cohen ZA, Levine WN, Gardner TR, Ateshian GA, Mow VC. Codominance of the individual posterior cruciate ligament bundles: an analysis of bundle lengths and orientation. The American journal of sports medicine. 2003 Mar;31(2):221-5.
- Logterman SL, Wydra FB, Frank RM. Posterior Cruciate Ligament: Anatomy and Biomechanics. Curr Rev Musculoskelet Med. 2018;11(3):510-514. doi:10.1007/s12178-018-9492-1
- Gupta R, Sood M, Malhotra A, Masih GD, Raghav M, Khanna T. Incidence, Risk Factors, and Management of Infection Following Anterior Cruciate Ligament Reconstruction Surgery. Indian J Orthop. 2018;52(4):399-405. doi:10.4103/ortho.IJOrtho_379_17
- Keller RA, Moutzouros V, Dines JS, Bush-Joseph CA, Limpisvasti O. Deep Venous Thrombosis Prophylaxis in Anterior Cruciate Ligament Reconstructive Surgery: What Is the Current State of Practice?. Sports Health. 2018;10(2):156-159. doi:10.1177/1941738117730576
- Shahrulazua A, Rafedon M, Mohd Nizlan MN, Sullivan JA. Delayed compartment syndrome of leg and foot due to rupture of popliteal artery pseudoaneurysm following posterior cruciate ligament reconstruction. BMJ Case Rep. 2014;2014:bcr2013202098. Published 2014 Jan 23. doi:10.1136/bcr-2013-202098
- Wang SH, Chien WC, Chung CH, Wang YC, Lin LC, Pan RY. Long-term results of posterior cruciate ligament tear with or without reconstruction: A nationwide, population-based cohort study. PLoS One. 2018;13(10):e0205118. Published 2018 Oct 3. doi:10.1371/journal.pone.0205118