Iliotibial Band Syndrome
Iliotibial band syndrome (ITBS) is one of the many causes of pain in the lateral or outer side of the knee. It is commonly diagnosed in long-distance athletes like marathon runners and cyclists. Iliotibial band syndrome can further progress with time if left untreated.
In this post, we’ll discuss the iliotibial band syndrome, its causes, symptoms, and treatments. If you’re someone with lateral knee pain, you may want to understand how ITBS affects the lateral knee and what can you do to treat it before it gets worse.
What Is Iliotibial Band Syndrome?
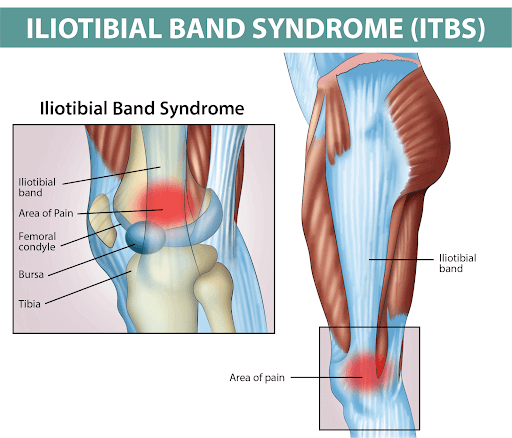
Iliotibial band syndrome is an overuse injury. It is an inflammation of the iliotibial band and the surrounding connective tissues which leads to lateral knee pain.
The iliotibial band (ITB) is the continuation of the tensor fascia lata, gluteus medius, and gluteal maximus distally towards the knee joint. It travels superficially to the vastus lateralis and inserts on the Gerdy tubercle of the lateral tibial plateau. It also inserts slightly partial to the supracondylar ridge of the lateral femur.
It has an anterior extension called the iliopatellar band. This band connects the lateral patella and prevents the patella from turning medially. The ITB functions as a knee extensor when the knee is less than 30 degrees of flexion. Beyond 30 degrees of flexion, it becomes a knee flexor.
Symptoms of ITBS are often present on the lateral side of the knee and the thigh. It is often associated with repetitive motion like running, cycling, long-distance walking, jogging, and similar activities or sports like soccer and skiing.
Symptoms of ITBS
Here are some symptoms that can present with ITBS. Keep in mind that it is not necessary that all of them be present for a clinical diagnosis.
Burning, Aching, or Tenderness Outside the Knee
ITBS may start off with discomfort or burning in the lateral knee. There may be some tenderness to the touch of the knee. The pain may turn achy or dull and spread to the outer thigh as well.
Clicking, Popping or Snapping Outside the Knee
As the condition progresses, there may be a snapping, clicking, or popping. In ITBS, this is due to inflammation which can cause knee misalignment. And so, as the knee tracks with movement, the patella rubs against the surrounding structures and produces a sound. In ITBS, this clicking is felt in the lateral knee.
Pain Throughout the Leg
Pain can also progress to the lower leg because the inflamed ITB may compress structures below it. As the inflammation worsens, the strain on the knee joint increases and the pain spreads throughout the leg.
Redness and Warmth Outside the Knee
It’s not unusual for the outer part of the knee to turn warm and red due to the inflammation of the ITB. Redness and warmth are signs of inflammation that occur when there is injury and inflammatory cells and chemicals are drawn to the area to repair the injury.
Anterior Lateral Knee Pain
The knee joint is one of the most complex joints of the human body. The femur, the tibia, patella, and fibula all contribute to this joint. They are held together by a myriad of strong ligaments that stabilize and support the joint. Anterior lateral knee pain is pain that occurs in the anterior and the anterior lateral region of the knee joint. A person may experience this pain front and center, in the outer aspect of the knee, or diffusely throughout the joint. The cause of the pain is some pathology in the anterior and lateral aspect of the knee.
Read More About Anterior Lateral Knee PainBurning Pain on Outside of Knee When Kneeling
There are many possible causes of burning pain on the outside of the knee while kneeling. One possibility is that you may have patellofemoral syndrome, which is a condition that results in pain around the kneecap. This pain can be aggravated by activities such as kneeling or squatting. Other potential causes of this type of pain include iliotibial band syndrome, runners knee, and meniscal tears. If you are experiencing burning pain on the outside of your knee while kneeling, it is important to see a doctor for evaluation. Some of these conditions can be treated with conservative measures such as rest, ice, and physical therapy…
Read More About Burning Pain on Outside of Knee When KneelingKnee Hurts When I Bend It and Straighten It
Your knees bend countless times throughout the day. Running up the stairs, down the hall after kids, and getting into the car. You straighten the knee as you walk, descend stairs or get into and out of the car. Bending and straightening the knee are necessary for daily activities. Knee pain with bending or straightening may be a mild, transient irritation or may indicate a more significant problem. Learn more below and avoid further injury and dysfunction. Knee pain can vary significantly depending upon many factors including the actual source of the pain, the severity of the injury, general health, and level of activity…
Read More About Knee Hurts When I Bend It and Straighten ItCommon Causes of ITBS
These are the most common causes of ITBS.
Excessive Friction Between the Iliotibial Band and Thigh Bone
One cause of ITBS is the repetitive friction of the ITB and the lateral epicondyle of the femur. This occurs during flexion and extension leading to inflammation of the area of the ITB that comes in contact with the bone.
Contact between the ITB and lateral epicondyle takes place at 30 degrees of flexion. This is the degree of knee flexion when the foot strikes the ground while walking or during motion also known as foot strike.
Poor Alignment of the Lower Body
Poor alignment of the lower body can occur due to internal tibial torsion and weakness of the hip abductors. This puts additional pressure on the ITB and muscles of the lower extremity during motion.
Excessive pronation of the foot and medial compartment arthritis can also lead to genu varum (outward curving of the knee). All of the above conditions cause a misaligned lower extremity which increases the muscle tension of the ITB. This causes ITBS.
Repetitive Bending and Extending of the Knee
Any motion that forces the knee to turn inward repeatedly during knee extension can cause ITBS. This could be running on an uneven surface and even using worn shoes. This strains the ITB leading to inflammation of the ITB.
Dysfunction or Tightness in the Glute Muscles and TFL muscle
The muscles that contribute to the IT band can be weak and tight leading to pulling on the IT band. Also, if the nerves that innervate the TFL and Glutes (L4-S1 spinal nerves) are irritated due to back problems, that can cause spasms and trigger points in the muscles causing IT band stress as well.
Who Is at Risk for ITB Syndrome?
The following people are at risk for developing iliotibial band syndrome:
- Long-distance runners, cyclists, tennis players, soccer players, skiers, and weight lifters are at risk due to the strain on the iliotibial band.
- It is also present in a high proportion in military recruits who run and walk long distances.
How Doctors Examine and Diagnose ITB Syndrome
Doctors diagnose ITB syndrome via the following ways.
- History: Since ITB syndrome is a clinical diagnosis, history is very important. The doctor will inquire about the symptoms, changes in the level of activity, mileage of long-distance activity, and the state of the training shoes.
He or she will want to find out about any recent changes in prolonged aerobic activities and the presence of any injuries, exacerbating symptoms like foot striking the ground, and any relieving symptoms. - Physical examination: The doctor will examine the knee for misalignments which can increase the tension on the ITB. He or she will palpate the knee for effusions or lax ligaments. The doctor will also try to palpate the crepitus with motion. In addition, the doctor can feel for trigger points in the glutes and TFLs.
- Special tests: Special tests like the Noble and Ober tests are done. In the Noble test, the doctor palpates the lateral femoral epicondyle. The doctor then extends the knee from 90 degrees of flexion to 0 degrees of extension. If there is pain at 30 degrees of flexion, there will likely be a positive diagnosis.
The Ober test is when the patient is in the lateral recumbent position with the knees flexed to 90. The doctor stands behind the patient, and abducts and extends the affected hip while supporting the knee. The test is considered positive when there is pain and restriction to the lateral knee when the knee is adducted. - Imaging: X-rays are only done to rule out a fracture, patella misalignment, and osteoarthritis. In ITBS, the X-rays are usually normal. If the diagnosis is not clear with history and the physical exam, then an MRI may be done.
An MRI will show a hyperintense lateral epicondyle with a thickened distal ITB. An ultrasound can also visualize abnormal distal ITB thickening.
How Can I Prevent ITB Syndrome?
ITB syndrome can be prevented. This is an inflammatory condition and if you are careful, you can prevent this inflammation from occurring. Here are a few ways listed below with the following preventative measures:
- If you run or cycle long miles, start with a quarter-mile walk first to loosen up the muscles.
- Limit training on concrete surfaces.
- Always run on flat surfaces and avoid steep inclines. The friction on the ITB increases as the quads get fatigued.
- Cover the knee joint when training in temperatures below 60 F. This is because the ITB tightens up in colder temperatures and is less flexible which increases the probability of injury.
- Increase your training intensity gradually. This should ideally be about 10% increments per week. This applies not just to intensity but also to distance, the amount of weight lifted, and the duration of your workout. It will allow the muscles to slowly get accustomed to the increase in stress.
- If your shoes have worn out on the side, replace them with new ones.
- Activate your core and glutes before working out and mobilize your hips.
- Do your glute, TFL, and hamstring stretches after a workout. This will prevent the ITB from tightening up.
- Strength train all the muscle groups of the lower extremity so the stress distribution is uniform across the joints.
- If you experience any pain in the knee, stop training for a few days and allow the ITB to recover.
- If there is any tightness in the ITB, use a foam roller across it as well as the TFL and Glutes to stretch it out.
Common Iliotibial Band Syndrome Treatments
There are many treatment options for ITB syndrome. They are listed below.
Stop Activities That Trigger the Pain
Stopping activities that trigger or worsen the pain is the best and most natural treatment. If you have pain while running or cycling in the lateral part of the knee, stop at once. Decrease your mileage for a few days. If the pain persists, stop training until the pain has subsided.
Stretching and Core Exercises
If there is tightness in the ITB, then stretching exercises like side-lying leg raises, and seated spinal twists can help stretch out the ITB. A foam roller can be used to stretch out the ITB. Apart from this, exercise to strengthen core muscles, hamstrings, quadriceps, and glutes will also help by reducing the strain on the ITB band.
Ice Packs
Ice packs will reduce inflammation by constricting the blood vessels. This will reduce any swelling and pain in the lateral knee.
Corticosteroid Injections
Local corticosteroid injections into the iliotibial band can reduce inflammation in the iliotibial area. These injections can reduce swelling, pain, and inflammation for a few months.
NSAIDs
The other day I was evaluating a patient and reviewing the treatment options for their spine condition. After discussing prior treatments, we got to the topic of medications taken for pain relief. She explained that she mainly utilized anti-inflammatory (NSAID) medications and then she told me to hold much she takes and has been for many years…..she takes close to 2 grams (2000 milligrams) on a daily basis which equated to about 9-10 capsules of medication per day. I was shocked, considering she was pre-diabetic and with high blood pressure plus the kicker of it is that her PCP (primary care physician) is ok with this…
Read More About NSAIDsWhen Is it Time to Consider Surgery?
Surgical intervention is only considered in refractory cases where the conservative treatment has not improved the condition for more than six months. There are several surgical options which include the percutaneous or open ITB release, ITB lengthening with a Z-plasty, open ITB bursectomy, and ITB debridement via arthroscopy.
- The open ITB release can be done via many techniques like resecting a triangular portion of the distal posterior iliotibial band, resecting the 2 cm x 4 cm portion that overlies the lateral femoral epicondyle, and also making a V-shaped incision in the ITB. There are limited studies showing one technique is better than the other.
- ITB bursectomy is usually done where there are symptoms of ITBS but there’s no finding of ITBS demonstrated on MRI. The procedure involves excising the underlying ITB bursa while allowing the ITB to remain completely intact.
- Minimal invasive techniques to resect the lateral synovial recess connecting the ITB to the lateral femur and innervated synovial fat have been done via arthroscopy.
Regenexx
Regenexx® procedures use sophisticated image-guided injections to place high-dose platelet-rich plasma (PRP) or bone marrow concentrate which contains stem cells, in critical areas to promote the body’s ability to heal itself. As the headquarters of Regenexx, Centeno-Schultz is where all of these procedures used by our national network began and were invented. These are breakthrough, non-surgical treatments for people suffering from joint and spinal pain. So, if you’re looking for an alternative to surgery for ITBS in Denver or Boulder, Colorado, or anywhere else, we’d be happy to help.
In the case of ITBS, these platelets are reintroduced into the iliotibial band under direct ultrasound visualization to ensure accurate placement to promote the body’s natural healing of the micro-injuries in the ITB and reduce the surrounding inflammation.
Furthermore, at the Centeno Schultz Clinic, our physicians do a thorough examination to see if the IT band syndrome is related to low back problems or nerve irritation. If so, those can be treated with PRP and our specialized PRP growth factor solution called Platelet Lysate to stimulate the body’s natural healing response of the affected nerves.
As discussed, you can look to manage the pain from ITBS with many different medications or treatments. However, the CSC approach to treating ITBS with Regenexx procedures is geared to not just managing the pain but treating the structural causes of the pain.
If you have ITBS and would like to consider Regenexx, then contact one of our board-certified doctors to see if this is a good option for you.

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreAre you a Candidate?
Other Resources on Iliotibial Band Syndrome (ITBS)
Free Download: The Knee Owner’s Manual

This e-book by Dr. Chris Centeno examines the knee and its role in the human musculoskeletal system and the body as a whole. The Knee Owner’s Manual provides a series of tests and clearly defined exercises that you can perform on your own to assess and monitor your own knee health. It will allow you to look for trouble spots where your own body may be having difficulty with stability, articulation, symmetry, and neuromuscular function. You’ll be able to see how these deficits in other regions of the body relate to the knee.
The Knee Owner’s Manual also discusses how Regenexx is pioneering the development of interventional orthopedics, a new branch of medicine that employs regenerative biologic therapies such as adult bone marrow concentrate and platelet-rich plasma to help repair and strengthen damaged tissues in other areas of the body.
This is contrasted with invasive knee surgeries, which often remove important tissues or replace the entire knee itself when it becomes damaged. With hyperlinks to more detailed information, related studies, and commentary, this book condenses a vast amount of data, images, and resources into an enjoyable and informative read. This is the first edition of The Knee Owner’s Manual, a companion book to Orthopedics 2.0.
-
What Is Golfer’s Knee, And What Can I Do About It?
The nature of golf is such that both the backswing and downswing affect the knee. The entire swing takes a little over one second. However, it can exert a force of 4 times the body weight on the front knee and 3 times the weight on the back knee (1). This makes knee injuries just as…
-
Knee Pain Location Chart: What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
Understanding Knee Pain Symptoms To Get The Best Treatments
Knee pain affects about 25% of the population (1). The knee joint involves three bones, namely the patella, the femur, and the tibia. Knee pain can be a sign of damage to the ligaments, bones, bursae, or muscle tendons because there are so many structures within the knee joint. In this post, we’ll discuss the…
-
KT Tape For Hamstring Tendonitis
Hamstring tendinosis is a condition that causes pain and inflammation in the hamstring tendons. The hamstring tendons are the tough bands of tissue that attach the hamstring muscles to the bones in the back of the thigh. Hamstring tendinosis is a degenerative condition, meaning that it is a condition that causes the tissue to break…
-
6 Meniscus Tear Types And How To Treat Them Properly
Even a small meniscus tear can make walking difficult for you. If you are experiencing any of these symptoms, you may want to seek medical help as soon as possible, depending on the type of tear you have. Needless to say, a lot depends on understanding the meniscus tear types there are and what each…
-
How To Heal A Torn Meniscus Naturally
If you have, or suspect you have a torn meniscus, and you’re wondering how to heal a torn meniscus naturally, you’ve landed on the right post. You may be wondering: Do I need surgery? Can you heal a torn meniscus naturally? The short answer is: It depends. What Is a Meniscus? The meniscus is a…