I snore a bit. Not anything serious (unless I’m on my back which causes my wife to relocate elsewhere). I know I have minor sleep apnea, so should I treat it? So, I thought it would be a great addition to the Aging Athlete series. Let’s dig in.
Denial Ain’t Just a River in Egypt
If you snore, you generally can’t hear yourself because you’re sleeping. Hence, you need an independent third party to assess your snoring. This is a spouse who will generally offer up unsolicited assessments of your nighttime symphony. When I see patients, I generally break this into the following comments from the spouse:
- “I can’t sleep through that…”
- “The dog can’t even sleep through it, we often need to find another place to sleep”
When I’m on my back I’m in the latter category. If you don’t have a spouse or third party assessor, you may want to download one of the many apps that can quantify sleep and snoring. Here are a few:
A Sleep Study
A sleep study is usually where you go to the hospital and have someone watch your sleep, oxygen saturation, and breathing. I actually had one done at home a few years ago by a friend who was a medical sleep specialist and who gave me a device that was taped to my chest. I got my diagnosis and I consulted with him about my CPAP settings. In the meantime, if you suspect you have these issues, please get a referral from your family doctor for a sleep study. There are now many at-home options, see this Google search for those, so hopefully, you can skip the hospital part.
Sleep Apnea
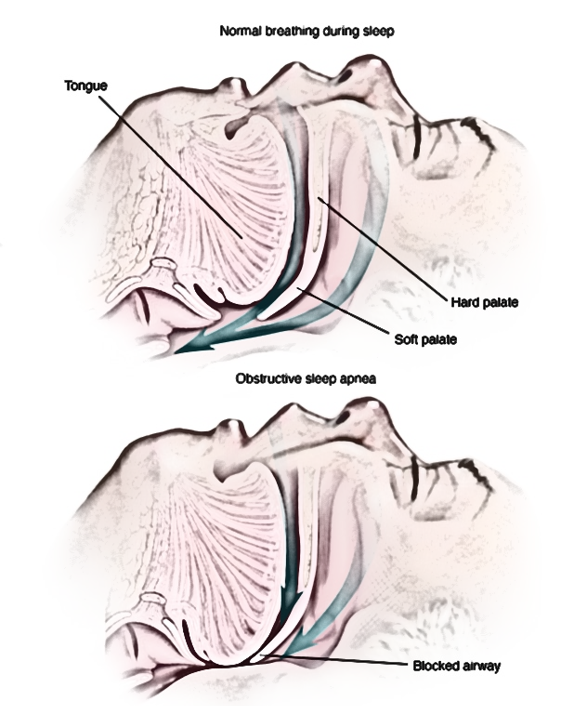
The type of sleep apnea that I have is called obstructive. When I sleep on my back my airway closes off and I snore. This means that I likely stop breathing at night or my oxygen saturation drops. So is this a big deal? Should I treat it? How does this connect with an aging athlete trying to stay active?
Sleep apnea can wreak havoc with the body. Let’s review.
Sleep Apnea and Metabolic Syndrome
If you snore this may be totally screwing up your blood sugar and adding on the pounds (1). This can also increase your risk of a heart attack, stroke, or afib. Meaning if you want to live well and stay active as you age rather than dropping dead at an early age, fixing your snoring is a good idea.
Can you fix snoring? Yes, CPAP has been shown to help reduce the harsh aging effects of snoring like type 2 diabetes (2). What’s CPAP?
What is CPAP?
CPAP stands for Continuous Positive Airway Pressure, which is a machine that connects to a mask that blows positive pressure in your airway to keep it open as you sleep. There are lots of different types of machines, big and small. If you sleep with a spouse, quiet should be the feature you seek. You also may want to hide this thing on date night (see my picture above).
I definitely have needed to do this for years, but I procrastinated and put it off. However, I’m diving in with both feet now as part of my aging athlete series, so I’d like to invite you to my little CPAP experiment. First, I bought this unit online, the IntelliPAP 2 Auto. It’s super quiet, so my wife can’t hear it. But can I do this?
The first thing I did, since this is close to Halloween, is to scare the snot out of my wife and younger son. Why? Why not? I look like the love child of Freddy Krueger and a science experiment gone bad. My wife nearly had a heart attack as I added breathing sounds through the mask for effect.
Wearing a CPAP Is Not for the Faint of Heart
I began just figuring out how I would wear this damn thing. It goes over your head with connectors on the side that come around the neck and then back up to the mask (the lower white strips above). If you don’t have it on just right and sealed against your face, it blows air through that lost seal, as it’s trying to reach a certain pressure. This is really weird, so the first night I tried CPAP I ended up parched and dehydrated and maxed out at two hours of blowing wind on my face. I felt like a dog with his head out the car window.
By night 2, I had figured out how to get the mask sealed through better adjustment and put the head of my bed up so I could sleep on my back. I lasted for 2 hours as well, mostly because I’ve been training myself for years not to sleep on my back. However, last night was the third night with the best mask fit and I lasted 4 hours, so maybe I can do this?
Does It Work?
I’ve heard from CPAP users that once they get used to this thing they have great sleep without all of the interruptions that snorers notice. Meaning if you snore, you likely wake up quite a few times during the night. I’m not there yet, so it’s hard to say. Tonight I’ll try for 6 hours. In the meantime, it’s a bit like a Nazi sleep science experiment, but I’m trying hard to make this thing work!
The upshot? Snoring is bad for the aging athlete. Hence, if you snore, you need to get a sleep study as you likely have lots of episodes where you stop breathing and that’s beating up your system. I’ll report back once I figure out my Freddy Krueger mask!
Metformin Update from Episode 4 of Aging Athlete Series
I am now officially on Metformin sustained release 500mg twice a day. My blood sugar control is better. The first few days for me came with some “GI disturbance”, but that got better over a few more days. Interestingly, I’ve had irritable bowel symptoms for years, which is now improved on the Metformin. This makes sense, as it acts in the gut. So far so good. Am I any younger? Not sure, but I thought today I looked a bit better in the mirror, so does that count? I also have yet to begin the growth hormone part of that medication triad of DHEA, Metformin, and HGH. Hopefully, that will be episode 6.
_____________________________________________
References:
(1) Meurling IJ1, Shea DO, Garvey JF. Obesity and sleep: a growing concern. Curr Opin Pulm Med. 2019 Nov;25(6):602-608. doi: 10.1097/MCP.0000000000000627.
(2) Abud R, Salgueiro M, Drake L, Reyes T, Jorquera J, Labarca G. Efficacy of continuous positive airway pressure (CPAP) preventing type 2 diabetes mellitus in patients with obstructive sleep apnea hypopnea syndrome (OSAHS) and insulin resistance: a systematic review and meta-analysis. Sleep Med. 2019 Jan 7;62:14-21. doi: 10.1016/j.sleep.2018.12.017.