EDS is a complex group of inherited disorders that affect and weaken connective tissues such as tendons and ligaments (1). Primary sites of involvement include skin, joint, and blood vessels (2). Joints are typically hypermobile with excessive joint range of motion. EDS headaches are an unfortunate, persistent issue.

Pain can arise from tissue trauma to the tendons, ligaments, and muscles but also arise from injury of an affected joint and cartilage.
Can EDS cause migraines?
Yes!. Due to an inherent disorder in the brain blood flow patients with EDS are prone to migraines (3). Ehler-Danlos syndromes are classified into thirteen subtypes (4). Migraines with or without aura are the most common form of headaches in The EDS, hypermobility type (EDS-HT) (5). A recent study demonstrated that in the EDS-HT group, migraines had an earlier onset and a higher number of episodes per month when compared to non-EDS patients (5).
Can EDS cause other types of headaches?
EDS patients commonly suffer a variety of headache types which include:
- Tension headache (6)
- Occipital neuralgia due to pressure and irritation of the lesser and greater occipital nerves. (7)
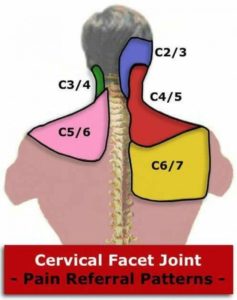
- Facet headache pain due to the instability of the facet capsule and ligaments ligament (7). The facet joint is a posterior joint in the cervical, thoracic and lumbar spine that limits the movement and protects the spine from excessive rotation and flexion. Each cervical facet has a specific referral pattern illustrated below. For example, injury to the C2/3 facet can result in pain radiating from the neck into the head and frontal area.
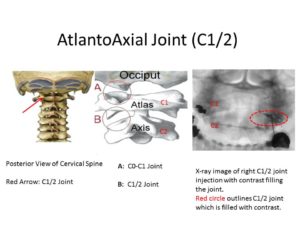
C1/2 Joint Pain
The C1 vertebra is the most superior vertebra in the neck and is called the atlas whereas the C2 vertebrae is called the axis. The C1 and C2 vertebrae stack upon one another and create a joint which is termed the AA (Atlantoaxial) joint. Patients with EDS have ligament instability which makes them prone to AA joint injury and dysfunction(8), AA joint pain is typically referred to the base of the skull. At the Centeno-Schultz Clinic we have extensive experience with C1/2 joint injections for patients with neck and headache pain. Patients with ligament injury or hypermobility are oftentimes plagued with headaches arising from this joint. x-ray guided injections of PRP or bone marrow concentrate containing stem cells can provide significant benefit and stability of supporting ligaments.
CCJ Pain
The neck is connected to the head by several critical ligaments which include the Alar, Transverse and Accessory Ligaments. Trauma, strain, or degeneration of these critical ligaments can result in instability and agroup of neurological and pain symptoms including neck pain, headache, and brain fog. The accurate medical term to describe this condition is Craniocervical junction (CCJ) Instability. It is a life-changing condition as many providers do not understand it and fail to diagnose it. EDS patients are particularly susceptible to CCJ instability, also called craniocervical instability, given the defect in collagen formation and loose ligaments. At the Centeno-Schultz Clinic we are the only clinic in the world to offer a stem cell injection to treat CCJ instability. To review CCJ instability and the injection watch video.
Patients with EDS have significant pain including headaches which can be tension, occipital neuralgia, facets or arising from injury to C1/2 joint or alar and transverse ligaments. The Centeno-Schultz Clinic has extensive experience in the management and treatment of EDS type headaches utilizing both PRP and bone marrow concentrate or “BMC” for short. Schedule an appointment and learn how PRP and BMC can address your debilitating headaches.
Doctors Who Treat Ehlers Danlos Syndrome Headaches

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics.
Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who travel to Colorado to undergo innovative, non-surgical treatments. Dr. Centeno has chaired multiple international research-based conferences. He also maintains an active research-based practice, with multiple publications listed in the US National Library of Medicine. Dr. Centeno has also served as editor-in-chief of a medical research journal dedicated to traumatic injury.
Dr. Centeno trained at the Baylor College of Medicine, Texas Medical Center, and the Institute for Rehabilitation Research. He hails from both Florida and New York and currently resides in Boulder, Colorado with his wife and three children.

John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreReferences:
1.. Zhou Z, Rewari A, Shanthanna H. Management of chronic pain in Ehlers-Danlos syndrome: Two case reports and a review of literature. Medicine (Baltimore). 2018;97(45):e13115. doi:10.1097/MD.0000000000013115
- Hakim AJ, Sahota A. Joint hypermobility and skin elasticity: the hereditary disorders of connective tissue. Clin Dermatol. 2006;24(6):521-33.DOI: 10.1016/j.clindermatol.2006.07.013
- Jacome DE. Headache in Ehlers-Danlos syndrome. Cephalalgia. 1999;19(9):791-6.DOI: 10.1046/j.1468-2982.1999.1909791.x
- Malfait F, Francomano C, Byers P, et al. The 2017 international classification of the Ehlers-Danlos syndromes. Am J Med Genet C Semin Med Genet. 2017;175(1):8-26.DOI: 10.1002/ajmg.c.31552
- Puledda F, Viganò A, Celletti C, et al. A study of migraine characteristics in joint hypermobility syndrome a.k.a. Ehlers-Danlos syndrome, hypermobility type. Neurol Sci. 2015;36(8):1417-24.DOI: 10.1007/s10072-015-2173-6
- Jacome DE. Headache in Ehlers-Danlos syndrome. Cephalalgia. 1999;19(9):791-6.DOI: 10.1046/j.1468-2982.1999.1909791.x
- Castori M, Morlino S, Ghibellini G, Celletti C, Camerota F, Grammatico P. Connective tissue, Ehlers-Danlos syndrome(s), and head and cervical pain. Am J Med Genet C Semin Med Genet. 2015;169C(1):84-96.DOI: 10.1002/ajmg.c.31426
- Mathers KS, Schneider M, Timko M. Occult hypermobility of the craniocervical junction: a case report and review. J Orthop Sports Phys Ther. 2011;41(6):444-57.DOI: 10.2519/jospt.2011.3305