Patellar Tendon Tear
Causes, Symptoms, Treatments, and Other Resources
Last month while in the park you injured your knee. You heard a pop followed by an immediate onset of intense pain and swelling. Walking was impossible. The swelling has continued and you have noticed bruising. Your doctor thinks you may have injured your patellar tendon. What is a Patellar tendon? Are there different types of Patellar tendon tears? What are the symptoms of a Patellar tendon tear? What are the five most common causes of Patellar tendon tears? How to diagnose a Patellar tendon tear?
Patellar Tendon Tear & Why You Should Care
Tendons are thick pieces of connective tissue that connect muscle to bone. They are important for the movement and stability of our joints. Small tears of a tendon can make it difficult to walk. Large tears can be debilitating preventing activity. Is a Patellar tendon tear responsible for your ongoing knee pain and dysfunction?
What Is a Patellar Tendon ?
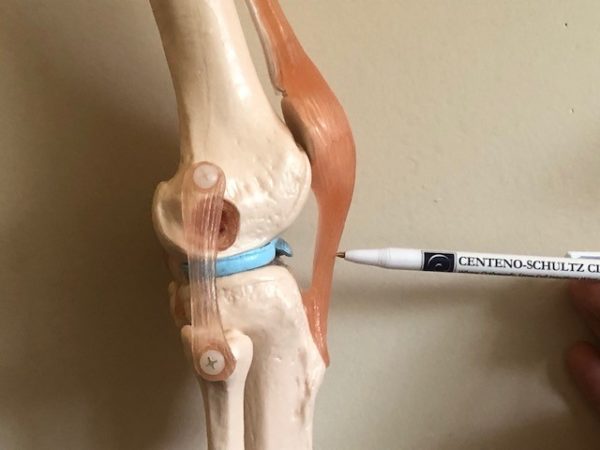
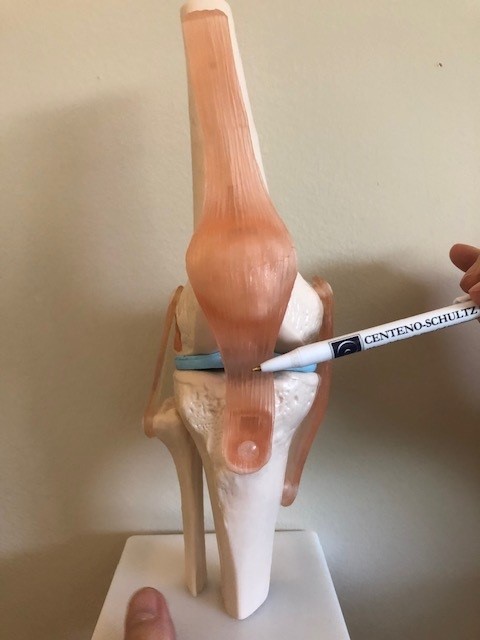
The Patellar tendon is the thick connective tissue that starts at the base of the kneecap (Patella) and extends down to the shin. The is an extension of the Quadriceps tendon (1). The Quadricep is the large thick muscle that is often referred to as our thigh. The Patellar tendon works together with the Quadriceps muscle to straighten (extend) the knee. It is easy to touch your Patellar tendon as it is immediately below the knee cap.
Are there Different Types of Patellar Tendon Tears? (Strain, Partial and Complete Tear)

Yes! There are three principal types of Patellar tendon tears which are graded 1-3.
Grade 1: Stretching of the Patellar tendon fibers. Also referred to as a sprain.
Grade 2: Partial-thickness tear. A portion of the Patellar tendon is torn but the surrounding fibers are intact.
Grade 3: Complete tear. Tear has extended across all the Patellar tendon fibers and the tendon ruptures. A rupture is similar to when a rubber band breaks when overstretched. There are two loose ends that are physically separated. When the Patellar tendon is completely torn, the tendon is separated from the kneecap. Without this attachment, you cannot straighten your knee.
Symptoms of Patellar Tendon Tear
Anterior Lateral Knee Pain
The knee joint is one of the most complex joints of the human body. The femur, the tibia, patella, and fibula all contribute to this joint. They are held together by a myriad of strong ligaments that stabilize and support the joint. Anterior lateral knee pain is pain that occurs in the anterior and the anterior lateral region of the knee joint. A person may experience this pain front and center, in the outer aspect of the knee, or diffusely throughout the joint. The cause of the pain is some pathology in the anterior and lateral aspect of the knee.
Read More About Anterior Lateral Knee PainBruising in Knee
Bruising in the knee, also known as a knee contusions, is an uncomfortable yet common condition that occurs when you strike your knee with force or a symptom of a knee condition. When the tiny blood vessels are damaged and blood leaks out beneath the skin, causing the typical swelling and red/purple discoloration seen in these injuries, it is termed a bruise or contusion. Although a knee contusion does not usually require medical intervention, you may need to visit your doctor to ensure that you do not have a more significant problem. If you hurt your knee and have swelling/pain that gets worse instead of better…
Read More About Bruising in KneeCan’t Straighten Knee
Your knee is capable of moving in a number of directions. The most common are flexion and extension. Flexion is when you bend your knee and the shin bone moves towards the buttock. Knee extension is when you straighten out your knee. The extension is the opposite of flexion. PT, trainers, and physicians alike measure the degree of knee flexion and extension. When lying flat on an examination table or hard surface your knee should be able to extend so that there is no angle between the thigh and shin bone. The inability to straighten the knee is also known as an extension lag and is a reason for concern.
Read More About Can’t Straighten KneeKnee Hurts When I Bend It and Straighten It
Your knees bend countless times throughout the day. Running up the stairs, down the hall after kids, and getting into the car. You straighten the knee as you walk, descend stairs or get into and out of the car. Bending and straightening the knee are necessary for daily activities. Knee pain with bending or straightening may be a mild, transient irritation or may indicate a more significant problem. Learn more below and avoid further injury and dysfunction. Knee pain can vary significantly depending upon many factors including the actual source of the pain, the severity of the injury, general health, and level of activity…
Read More About Knee Hurts When I Bend It and Straighten ItKnee Pain
Knee pain can be caused by many factors. Overuse injuries, direct trauma to the knee and arthritis are the most common causes of knee pain. Damage to the knee structures may cause swelling, scar tissue formation (fibrosis), and loss of function of the joint. Pain is often accompanied by difficulty walking, weakness, and instability. When the knee is overused, the thigh and shin bones (femur and tibia), cartilage, or tendons may experience stress. This leads to pain and discomfort as well as stiffness in the knee. Overuse injuries are common among athletes who participate in sports that involve running, jumping…
Read More About Knee PainKnee Swelling
Swelling of the knee, also known as water on the knee, is a condition in which fluid collects around the knee joint. Swelling can occur for a variety of reasons and affect patients of any age. Some swelling can be treated with over-the-counter medicines, but persistent and continuous swelling might result in tissue damage, bone softening, and cartilage deterioration. Over-the-counter medicines will assist relieve pain for individuals with a history of osteoarthritis and swelling following physical activity, such as exercise or running. During and after activity, the patient may apply compression sleeves to reduce the inflammation. Ice is another method…
Read More About Knee SwellingLoud Pop in Knee followed by Pain
If you hear a loud pop in your knee and then experience pain, it is possible that you have torn a ligament. Ligaments are the bands of tissue that connect bones to other bones and help stabilize the joint. There are four main ligaments in the knee: the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL), and lateral collateral ligament (LCL). The ACL is the most commonly injured ligament in the knee. It runs diagonally across the front of the knee and is responsible for rotational stability. A tear in the ACL can cause severe pain, swelling, and instability in the knee….
Read More About Loud Pop in Knee followed by PainTightness in Knee
What could tightness in your knee mean? When fluid builds up inside the knee as a result of an injury, overuse, or medical problem, the knees become swollen and tight. Swelling might be mild, so you may not always notice it unless it is serious damage. You may feel this as stiffness in the knee since swelling may not be visible. Swelling restricts movement since there is less room in the knee. Fluid buildup can be caused by irritation, internal bleeding, and injuries to the knee. Arthritis, gout, tumors, and baker cysts are all causes of swelling. Pain and swelling are the responses of your body to damage. Together they can lead to stiffness in your knee…
Read More About Tightness in KneeSymptoms will vary depending upon the severity of the injury (2). Many patients report a snapping or popping sensation at the time of the injury. Common symptoms include:
- Pain
- Swelling
- Bruising
- Difficulty or inability to walk
- Cramping
- Tenderness to the touch
Five Most Common Causes of Patellar Tendon Tear
There are many different causes of Patellar tendon tears. Patellar tendon tears are a common sport injury but can also occur from overuse or a motor vehicle injury. The tendon is typically injured in the area where the blood flow is poor and the tendon is the weakest. This area is also called the watershed region. The most common causes of Patellar tendon tears are:
Impact from Running and Jumping
Continued running and jumping can place significant strain on the Patellar tendon. Increasing mileage in preparation for a competition or event can place additional stress on the tendon. Chronic tendon overload is thought to be a leading cause of Patellar tendon tears (3). Patellar tendinosis, inflammation of the tendon can easily progress to Patellar tendon tears if not treated successfully in the acute phase. Chronic Patellar tendinosis oftentimes leads to Patellar tendon tears as the tendon fibers are weakened and susceptible to injury.
Tendon Weakness
The Patellar tendon may be weakened which makes it susceptible to tearing and possible rupture. Medical conditions that can weaken tendons include:
- Rheumatoid Arthritis
- Chronic Renal Failure
- Systemic Lupus
- Diabetes.
Tendons can also be weakened by steroids and certain antibiotics. Ciprofloxacin and other Fluoroquinolones have black-boxed warnings issued by the FDA for their known association with tendon ruptures (4). Sport experts have identified nine risk factors that contribute to Patellar tendon weakness (5). they include weight, increased body mass index, leg length differences, the arch height of the foot, quadriceps flexibility, and hamstring flexibility.
Trauma
Soccer, Lacrosse, and other field sports are rich in forceful contacts in addition to abrupt starts and stops. These forces can lead to Patellar tendon injuries. Trauma can also occur off the playing field and include simple falls around the house or cabin or motor vehicle accidents. Some patients when rear-ended are forcefully pushed forward striking their knee on the dashboard or steering wheel leading the Patellar tendon tears.
Aging
Aging is an unfortunate process when there is a general decline in bodily function. This includes the integrity of tendons and the overall function of the knee. As we age the Patellar tendon does not fold back upon itself during extension which puts it at risk for strain and tearing (6).
Prior Knee Surgery
Prior knee surgery increases the risk of a Patellar tendon tear. Often times orthopedic knee surgeries weaken the stability of the knee joint, changing the biomechanics of the knee and placing additional stress and strain on the Patellar tendon.
How to Diagnose Patellar Tendon Tear
Clinical presentation will vary depending upon the severity of the injury. Pain, swelling, and inability to walk are the most common hallmarks. Diagnosis of a patellar tendon tear requires a review of past medical history, physical examination, and possible imaging studies.
Medical History
Your doctor will discuss your past medical history, medications, and current symptoms. Questions you might be asked include:
- Have you had previous knee injuries?
- Have you had tendonitis?
- Have you had knee surgery?
Physical Examination
Examination of the knee will include an inspection to identify swelling, redness, and bruising. You will be asked to bend and extend the knee to assess its range of motion. Special physical examination maneuvers may be performed to assess knee function and integrity.
Imaging
To confirm a Patellar tendon tear imaging tests may be ordered. An x-ray is useful to identify a Patellar tendon rupture as the knee cap will slide up as it is no longer tethered by the tendon. MRI is useful to evaluate the location and size of Patellar tendon tears. At the Centeno-Schultz Clinic, ultrasound is used in our evaluation and management of patients with knee pain. Ultrasound is a powerful imaging modality that is readily available in the clinic, does not need prior authorization or scheduling, and can easily identify Patellar tendon tears.
Common Treatments for Patellar Tendon Tear
Treatment options will depend on the severity of the injury, past medical history, and access to care. When appropriate conservative care should always be first-line treatment. Treatment options include
Immobilization
During the acute phase, your physician may recommend you wear a knee immobilizer. This will keep the knee straight, limit additional injury, and allow the swelling to decrease. It will also allow for the healing to start.
Physical Therapy
Physical therapy is a cornerstone in the treatment of most Patellar tendon tears. Therapy will focus on increasing strength, stability, and range of motion. The most popular physical therapy involves eccentric exercise (7).
Steroid Injections
When physical therapy, immobilization, and other conservative treatments fail to provide significant benefits some patients are referred for a steroid injection. Steroids are powerful anti-inflammatory agents which can reduce swelling and pain. Unfortunately, they are toxic to most orthopedic tissue and have been demonstrated to damage cartilage, tendons, and ligaments (8). Steroids can cause tendon rupture (9). For this reason, steroids should be avoided.
Surgery
Surgery is rarely indicated with the exception of the complete tear. When this occurs the tendon ruptures into two pieces. Surgery is required to unite the two ends together. If the patellar tendon has ruptured from the patella bone, surgery may require the surgeon to drill a series of small holes into the patella bone in order to create a new anchor site. Complications exist and include weakness, loss of range of motion, and Patellar tendon re-tears (10).
Regenerative Options
The Physicians at the Centeno-Schultz Clinic are experts in the management of Patellar tendon tears. Treatment options include the use of PRP or Bone Marrow Concentrate. PRP is rich is growth factors that can decrease inflammation and increase blood flow both of which can accelerate healing. Bone Marrow Concentrate contains stem cells which are the body’s powerhouses of healing. All injections are performed under ultrasound guidance. This ensures accurate placement of the PRP or Bone Marrow Concentrate into the patella tendon tear.
We also pioneered the successful use of Bone Marrow Concentrate in the treatment of ACL tears. Much of the same technology is used in the treatment of Patellar tendon tears.
Rehab and Recovery from a Patellar Tendon Tear
Rehabilitation and recovery will vary depending upon the severity of the injury, past medical history, level of activity, and access to care. Physical therapy is essential and progressive over the course of treatment. Strengthening and range of motion are critical. Recovery can take between 6 weeks and 6 months. The advantage of PRP is that it can promote the acceleration of healing and recovery (11).
In Conclusion
Tendons are thick pieces of connective tissue that connect muscle to bone.
The Patellar tendon is the thick connective tissue that starts at the base of the kneecap and extends down to the shin.
The Patellar tendon works together with the Quadricep to extend (straighten) the knee.
There are three different types of Patellar tendons tears which are graded 1-3.
Grade 1 is a stretching of the Patellar tendon whereas Grade 2 is a partial thickness tear.
Grade 3 is a complete tear.
Common symptoms include pain, swelling, bruising, difficulty walking, and tenderness to the touch.
The five most common causes of a Patellar tendon tear are:
- Repetitive Running and Jumping
- Tendon Weakness
- Trauma
- Aging
- Prior Knee Surgery
A Patellar tendon tear is diagnosed by reviewing medical history, physical examination, and imaging.
Treatment options for Patellar tendon tear depend upon the severity of the injury. Common options include
- Immobilization
- Physical Therapy
- Steroid Injections
- Surgery
- Regenerative Options which include precise injections of PRP and Bone Marrow Concentrate.
If you or a loved one has sustained an injury with a Patellar tendon tear that has not responded to conservative care please schedule a telephone candidacy discussion with a board-certified, fellowship-trained physician. At the Centeno-Schultz Clinic in Broomfield and Denver, Colorado we are experts in the evaluation and treatment of knee injuries. From the comfort of your home or office learn what treatment options for knee pain are available for you.
Our Doctors Who Can Assist With a Patellar Tendon Tear

Christopher J. Centeno, MD
Christopher J. Centeno, M.D. is an international expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate in orthopedics. He is board-certified in physical medicine and rehabilitation with a subspecialty of pain medicine through The American Board of Physical Medicine and Rehabilitation. Dr. Centeno is one of the few physicians in the world with extensive experience in the culture expansion of and clinical use of adult bone marrow concentrate to treat orthopedic injuries. His clinic incorporates a variety of revolutionary pain management techniques to bring its broad patient base relief and results. Dr. Centeno treats patients from all over the US who…
Read more
John Schultz, MD
John R. Schultz M.D. is a national expert and specialist in Interventional Orthopedics and the clinical use of bone marrow concentrate for orthopedic injuries. He is board certified in Anesthesiology and Pain Medicine and underwent fellowship training in both. Dr. Schultz has extensive experience with same day as well as culture expanded bone marrow concentrate and sees patients at the CSC Broomfield, Colorado Clinic, as well the Regenexx Clinic in Grand Cayman. Dr. Schultz emphasis is on the evaluation and treatment of thoracic and cervical disc, facet, nerve, and ligament injuries including the non-surgical treatment of Craniocervical instability (CCI). Dr. Schultz trained at George Washington School of…
Read more
John Pitts, M.D.
Dr. Pitts is originally from Chicago, IL but is a medical graduate of Vanderbilt School of Medicine in Nashville, TN. After Vanderbilt, he completed a residency in Physical Medicine and Rehabilitation (PM&R) at Emory University in Atlanta, GA. The focus of PM&R is the restoration of function and quality of life. In residency, he gained much experience in musculoskeletal medicine, rehabilitation, spine, and sports medicine along with some regenerative medicine. He also gained significant experience in fluoroscopically guided spinal procedures and peripheral injections. However, Dr. Pitts wanted to broaden his skills and treatment options beyond the current typical standards of care.
Read more
Jason Markle, D.O.
Post-residency, Dr. Markle was selected to the Interventional Orthopedic Fellowship program at the Centeno-Schultz Clinic. During his fellowship, he gained significant experience in the new field of Interventional Orthopedics and regenerative medicine, honing his skills in advanced injection techniques into the spine and joints treating patients with autologous, bone marrow concentrate and platelet solutions. Dr. Markle then accepted a full-time attending physician position at the Centeno-Schultz Clinic, where he both treats patients and trains Interventional Orthopedics fellows. Dr. Markle is an active member of the Interventional Orthopedic Foundation and serves as a course instructor, where he trains physicians from around the world.
Read more
Brandon T. Money, D.O., M.S.
Dr. Money is an Indiana native who now proudly calls Colorado home. He attended medical school at Kansas City University and then returned to Indiana to complete a Physical Medicine and Rehabilitation residency program at Indiana University, where he was trained on non-surgical methods to improve health and function as well as rehabilitative care following trauma, stroke, spinal cord injury, brain injury, etc. Dr. Money has been following the ideology behind Centeno-Schultz Clinic and Regenexx since he was in medical school, as he believed there had to be a better way to care for patients than the status quo. The human body has incredible healing capabilities…
Read moreView Our Resources on the Patellar Tendon
Free Download: The Knee Owner’s Manual

This e-book by Dr. Chris Centeno examines the knee and its role in the human musculoskeletal system and the body as a whole. The Knee Owner’s Manual provides a series of tests and clearly defined exercises that you can perform on your own to assess and monitor your own knee health. It will allow you to look for trouble spots where your own body may be having difficulty with stability, articulation, symmetry, and neuromuscular function. You’ll be able to see how these deficits in other regions of the body relate to the knee.
The Knee Owner’s Manual also discusses how Regenexx is pioneering the development of interventional orthopedics, a new branch of medicine that employs regenerative biologic therapies such as adult bone marrow concentrate and platelet-rich plasma to help repair and strengthen damaged tissues in other areas of the body.
This is contrasted with invasive knee surgeries, which often remove important tissues or replace the entire knee itself when it becomes damaged. With hyperlinks to more detailed information, related studies, and commentary, this book condenses a vast amount of data, images, and resources into an enjoyable and informative read. This is the first edition of The Knee Owner’s Manual, a companion book to Orthopedics 2.0.
-
Knee Pain Location Chart: Know What The Pain In Your Knee Means
The knee joint is the largest compound synovial joint of the human body. The joint has bones, cartilage, muscles, and bursae that are held together by ligaments and tendons. Damage to any of these structures can give rise to knee pain. The location of knee pain can be very telling, and can help narrow down…
-
Learn About Your Knee Pain Symptoms To Get The Best Treatments
Knee pain affects about 25% of the population (1). The knee joint involves three bones, namely the patella, the femur, and the tibia. Knee pain can be a sign of damage to the ligaments, bones, bursae, or muscle tendons because there are so many structures within the knee joint. In this post, we’ll discuss the…
-
KT Tape For Hamstring Tendonitis
Hamstring tendinosis is a condition that causes pain and inflammation in the hamstring tendons. The hamstring tendons are the tough bands of tissue that attach the hamstring muscles to the bones in the back of the thigh. Hamstring tendinosis is a degenerative condition, meaning that it is a condition that causes the tissue to break…
-
6 Meniscus Tear Types And How To Treat Them Properly
Even a small meniscus tear can make walking difficult for you. If you are experiencing any of these symptoms, you may want to seek medical help as soon as possible, depending on the type of tear you have. Needless to say, a lot depends on understanding the meniscus tear types there are and what each…
-
How To Heal A Torn Meniscus Naturally
If you have, or suspect you have a torn meniscus, and you’re wondering how to heal a torn meniscus naturally, you’ve landed on the right post. You may be wondering: Do I need surgery? Can you heal a torn meniscus naturally? The short answer is: It depends. What Is a Meniscus? The meniscus is a…
-
How to Read a Knee MRI for Meniscal Tear
Dr. Chris Centeno discusses how to read a knee MRI for meniscal tears and what you need to know about such tears. Transcript Hi, this is Dr. Centeno. And I’d like to go over today How to Read Your Knee MRI: Focus on the Meniscus. I have a whole series of these and reading a…
1.Reinking MF. CURRENT CONCEPTS IN THE TREATMENT OF PATELLAR TENDINOPATHY. Int J Sports Phys Ther. 2016;11(6):854-866. [Google Scholar]
2.Rosso F, Bonasia DE, Cottino U, Dettoni F, Bruzzone M, Rossi R. Patellar tendon: From tendinopathy to rupture. Asia Pac J Sports Med Arthrosc Rehabil Technol. 2015;2(4):99-107. Published 2015 Aug 7. doi:10.1016/j.asmart.2015.07.001
3.Lavagnino M, Arnoczky SP, Elvin N, Dodds J. Patellar tendon strain is increased at the site of the jumper’s knee lesion during knee flexion and tendon loading: results and cadaveric testing of a computational model. Am J Sports Med. 2008 Nov;36(11):2110-8. doi: 10.1177/0363546508322496. Epub 2008 Sep 3. PMID: 18768702.
4.Tanne JH. FDA adds “black box” warning label to fluoroquinolone antibiotics. BMJ. 2008;337(7662):a816. Published 2008 Jul 15. doi:10.1136/bmj.a816
5.van der Worp H, van Ark M, Roerink S, Pepping GJ, van den Akker-Scheek I, Zwerver J. Risk factors for patellar tendinopathy: a systematic review of the literature. Br J Sports Med. 2011 Apr;45(5):446-52. doi: 10.1136/bjsm.2011.084079. Epub 2011 Mar 2. PMID: 21367808.
6.Slane LC, Dandois F, Bogaerts S, Vandenneucker H, Scheys L. Patellar tendon buckling is altered with age. Med Eng Phys. 2018;59:15-20. doi:10.1016/j.medengphy.2018.04.024
7. Visnes H, Bahr R. The evolution of eccentric training as treatment for patellar tendinopathy (jumper’s knee): a critical review of exercise programmes. Br J Sports Med. 2007 Apr;41(4):217-23. doi: 10.1136/bjsm.2006.032417. Epub 2007 Jan 29. PMID: 17261559; PMCID: PMC2658948.
8. Wernecke C, Braun HJ, Dragoo JL. The Effect of Intra-articular Corticosteroids on Articular Cartilage: A Systematic Review. Orthop J Sports Med. 2015;3(5):2325967115581163. Published 2015 Apr 27. doi:10.1177/2325967115581163.
9. Paavola M, Kannus P, Järvinen TA, Järvinen TL, Józsa L, Järvinen M. Treatment of tendon disorders. Is there a role for corticosteroid injection? Foot Ankle Clin. 2002 Sep;7(3):501-13. doi: 10.1016/s1083-7515(02)00056-6. PMID: 12512406.
10. Volk WR, Yagnik GP, Uribe JW. Complications in brief: Quadriceps and patellar tendon tears. Clin Orthop Relat Res. 2014;472(3):1050-1057. doi:10.1007/s11999-013-3396-6.
11.Dragoo JL, Wasterlain AS, Braun HJ, Nead KT. Platelet-rich plasma as a treatment for patellar tendinopathy: a double-blind, randomized controlled trial. Am J Sports Med. 2014 Mar;42(3):610-8. doi: 10.1177/0363546513518416. Epub 2014 Jan 30. Erratum in: Am J Sports Med. 2016 Jul;44(7):NP38. PMID: 24481828.